Non-24-Hour Sleep-Wake Cycle Disorder (Non-24) is a chronic circadian rhythm disorder where the internal biological clock fails to align with the 24-hour day-night cycle. Most prevalent in individuals who are completely blind, the disorder results in progressively delayed sleep and wake times, severely impacting daily functioning and quality of life.
While it commonly affects the blind due to their inability to perceive light—a primary regulator of circadian rhythms—sighted individuals can also experience Non-24 under certain neurological or psychiatric conditions.
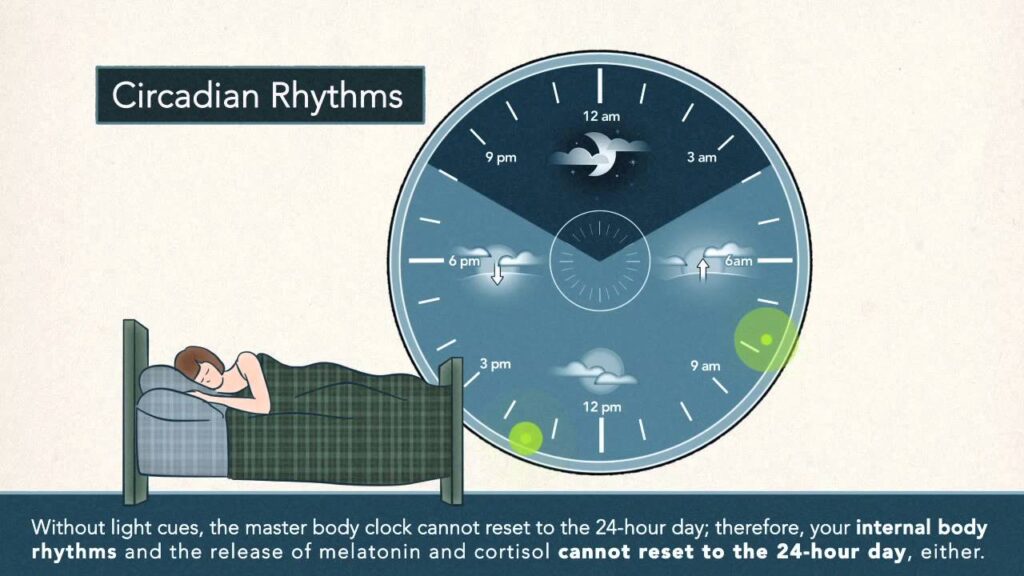
Circadian Rhythm and Its Role in Sleep Regulation
The circadian rhythm is an internal, biological process regulated by the suprachiasmatic nucleus (SCN) in the hypothalamus. This master clock governs physiological cycles such as sleep, wakefulness, hormone secretion, and body temperature, typically synchronized by environmental light-dark cues.
In Non-24, the circadian rhythm runs longer than 24 hours, often around 24.5 to 25 hours, leading to cyclic drift in sleep times.
Causes and Risk Factors
1. Blindness
The most common cause, especially in individuals lacking light perception, where retinal photoreceptors (intrinsically photosensitive retinal ganglion cells) fail to send light cues to the SCN.
2. Neurological Impairments
Lesions or dysfunction in the SCN or hypothalamic pathways can disrupt circadian rhythm synchronization.
3. Psychiatric and Behavioral Factors
In some sighted individuals, lifestyle patterns involving irregular sleep schedules, social isolation, or severe depression may contribute to Non-24.
4. Genetic Predisposition
Variants in clock genes (e.g., PER3, CRY1) have been linked to delayed or free-running sleep cycles.
Symptoms of Non-24-Hour Sleep-Wake Disorder
Patients often experience symptoms that cycle over weeks due to the drifting nature of their sleep-wake timing. As sleep time shifts, patients pass through brief periods of normal alignment followed by misalignment.
Core Symptoms:
- Gradually delayed sleep onset and wake times
- Insomnia during conventional sleep hours
- Excessive daytime sleepiness
- Mood changes such as irritability or depression
- Impaired concentration, alertness, and functionality
These symptoms can interfere with social, occupational, and academic activities, particularly when internal rhythms oppose societal norms.
Diagnosis of Non-24 Sleep-Wake Cycle Disorder
Diagnosis is primarily clinical, based on detailed sleep logs and actigraphy data over several weeks. Objective measurement is essential due to the gradual nature of the cycle.
Diagnostic Tools:
- Sleep Diary: 4–6 weeks of tracking sleep/wake patterns
- Actigraphy: Wrist-worn device recording movement and sleep timing
- Polysomnography (if indicated): To rule out other sleep disorders
- Melatonin Profiling: Measuring dim light melatonin onset (DLMO)
Differentiation from other circadian rhythm disorders, such as Delayed Sleep-Wake Phase Disorder, is crucial, as Non-24 involves a non-fixed pattern.
Non-24 in Blind Versus Sighted Individuals
Blind Individuals:
- Prevalence is significantly higher (up to 70%)
- Lack of light perception disables the brain’s ability to synchronize to the 24-hour cycle
- Melatonin therapy is often effective
Sighted Individuals:
- Less common
- Usually associated with psychiatric illness, neurodevelopmental disorders, or extreme social isolation
- Behavioral therapy is often combined with medication
Treatment and Management of Non-24-Hour Sleep-Wake Disorder
Management focuses on re-entraining the circadian rhythm to the 24-hour cycle using chronobiological, pharmacological, and behavioral interventions.
1. Melatonin and Melatonin Agonists
- Melatonin (0.5–5 mg) taken 1–2 hours before desired bedtime helps phase-advance the rhythm.
- Tasimelteon (FDA-approved for Non-24 in blind individuals) is a selective MT1 and MT2 receptor agonist with demonstrated efficacy.
2. Light Therapy (for sighted patients)
- Exposure to bright light (10,000 lux) in the morning can reset the circadian phase.
- Must be consistently timed and administered daily.
3. Behavioral Sleep Interventions
- Cognitive Behavioral Therapy for Insomnia (CBT-I)
- Sleep hygiene: Fixed sleep/wake times, screen time limitations, and pre-sleep relaxation routines
- Scheduled social and physical activities aligned with the 24-hour cycle
4. Pharmacological Adjuncts
- Short-acting hypnotics may be used for transient insomnia
- Stimulants or wake-promoting agents (e.g., modafinil) for daytime sleepiness