Non-Q Wave Myocardial Infarction (NQMI), a subset of acute coronary syndromes (ACS), represents a form of myocardial infarction without the classic Q wave development on electrocardiogram (ECG). While it does not exhibit full-thickness myocardial necrosis, it signifies a serious ischemic event requiring urgent intervention. NQMI is typically classified under non-ST elevation myocardial infarction (NSTEMI) and warrants attention due to its comparable morbidity and mortality risks relative to Q-wave infarctions.
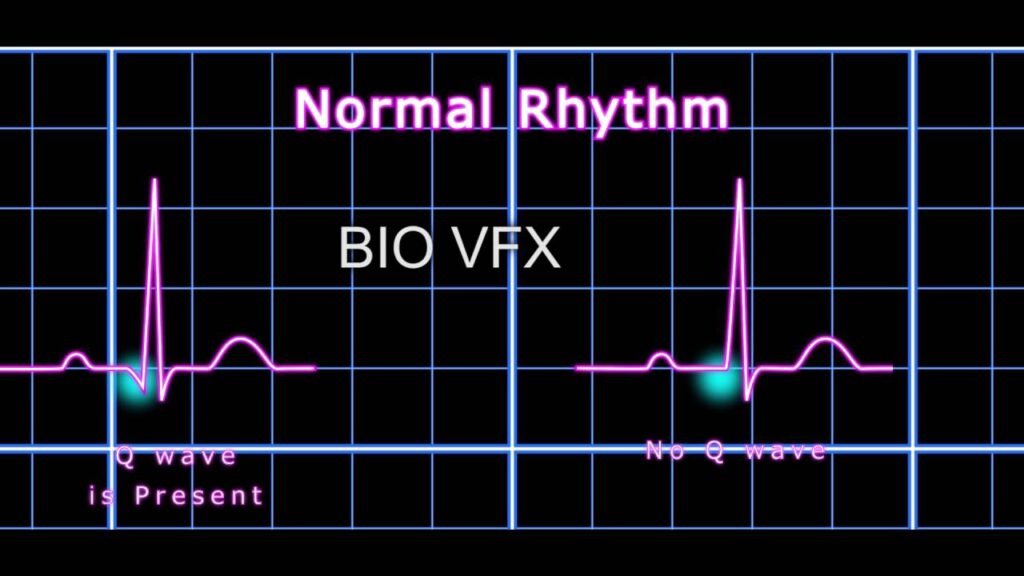
Pathophysiology of Non-Q Wave MI
NQMI arises when a partial or transient occlusion of a coronary artery causes subendocardial infarction. Unlike transmural infarctions seen in Q-wave MIs, the ischemia in NQMI is limited to the inner layers of the myocardium. This event is often driven by ruptured atherosclerotic plaques, platelet aggregation, and a thrombotic cascade without complete vessel occlusion.
Key Pathological Features:
- Subendocardial necrosis
- Incomplete coronary artery occlusion
- Limited myocardial wall involvement
- Absence of Q wave development on ECG
Clinical Presentation and Symptoms
The clinical manifestations of NQMI closely resemble those of other types of myocardial infarction but may be subtler.
Common Symptoms:
- Chest pain or pressure, often radiating to the neck, jaw, or arms
- Dyspnea
- Nausea and diaphoresis
- Fatigue or lightheadedness
- Symptoms may occur at rest or with exertion
The presence of angina-like symptoms, especially in patients with known cardiovascular disease or risk factors such as diabetes mellitus, hypertension, or smoking, should raise suspicion for NQMI.
Diagnostic Criteria and ECG Changes
The diagnosis of NQMI relies on biochemical markers of myocardial necrosis, particularly troponin I and T, alongside ECG findings and clinical evaluation.
Cardiac Biomarkers:
- Elevated troponins (most sensitive and specific)
- Creatine kinase-MB (CK-MB): Less specific but still utilized
ECG Findings in NQMI:
Unlike STEMI, NQMI does not present with persistent ST-segment elevation or pathologic Q waves.
Typical ECG Changes:
- ST-segment depression
- T-wave inversion
- Transient ST-elevation in rare cases
- Absence of Q waves in leads overlying the infarcted area
Differentiating NQMI from Q Wave MI and Unstable Angina
| Feature | Non-Q Wave MI (NQMI) | Q Wave MI | Unstable Angina |
|---|---|---|---|
| Q Wave Presence | Absent | Present | Absent |
| Troponin Elevation | Elevated | Elevated | Normal |
| ECG ST Changes | Depression / Inversion | Elevation | Depression / Inversion |
| Myocardial Damage Depth | Subendocardial | Transmural | Ischemia without necrosis |
Risk Factors and Underlying Causes
NQMI shares the same etiology and risk profile as other coronary artery diseases.
Major Risk Factors:
- Atherosclerosis
- Hypertension
- Diabetes mellitus
- Dyslipidemia
- Smoking
- Sedentary lifestyle
- Chronic kidney disease
Management and Treatment Strategies
The primary goals of managing NQMI are to relieve ischemia, prevent infarct progression, and reduce the risk of future cardiac events.
Immediate Medical Management:
- Aspirin: Antiplatelet therapy to inhibit thrombus formation
- P2Y12 inhibitors: Clopidogrel, ticagrelor
- Beta-blockers: Reduce myocardial oxygen demand
- Nitrates: Relieve chest pain
- Statins: Stabilize plaques and reduce LDL cholesterol
- Heparin or LMWH: Prevent clot propagation
- ACE inhibitors/ARBs: Particularly for patients with LV dysfunction
Invasive Approaches:
- Coronary angiography to assess extent of occlusion
- Percutaneous coronary intervention (PCI) for revascularization
- Coronary artery bypass grafting (CABG) in multi-vessel disease
Risk Stratification Tools:
- GRACE score
- TIMI risk score
Prognosis and Long-Term Outlook
While NQMI may appear less severe due to the absence of Q waves, the long-term outcomes are not benign. The risk of reinfarction and mortality remains significant, especially without adequate secondary prevention.
Prognostic Indicators:
- Elevated troponin levels
- Extensive coronary artery disease
- Left ventricular dysfunction
- Delayed or absent revascularization
Patients with NQMI require lifelong lifestyle modification, medication adherence, and cardiac rehabilitation to improve outcomes and quality of life.
Prevention and Secondary Care
Preventing a recurrence of NQMI involves comprehensive cardiovascular risk management.
Lifestyle Modifications:
- Smoking cessation
- Low-sodium, heart-healthy diet
- Regular physical activity
- Weight control and diabetes management
Medical Surveillance:
- Regular follow-up with a cardiologist
- Routine lipid, glucose, and blood pressure monitoring
- Adherence to prescribed cardioprotective medications
Non-Q Wave Myocardial Infarction is a clinically significant form of ischemic heart disease with subtle ECG findings but substantial prognostic implications. Prompt diagnosis, aggressive medical therapy, and appropriate revascularization are essential to improving patient outcomes. Understanding the nuanced presentation and management of NQMI is crucial for clinicians and patients alike.

