Nocardiosis is a rare but potentially severe opportunistic bacterial infection caused by species of the Nocardia genus. These gram-positive, filamentous bacteria primarily affect the lungs, central nervous system (CNS), and skin. While nocardiosis can develop in healthy individuals, it predominantly occurs in immunocompromised patients, such as those with HIV/AIDS, organ transplant recipients, and individuals undergoing long-term corticosteroid therapy. Early detection and appropriate antibiotic treatment are crucial to managing this condition effectively.
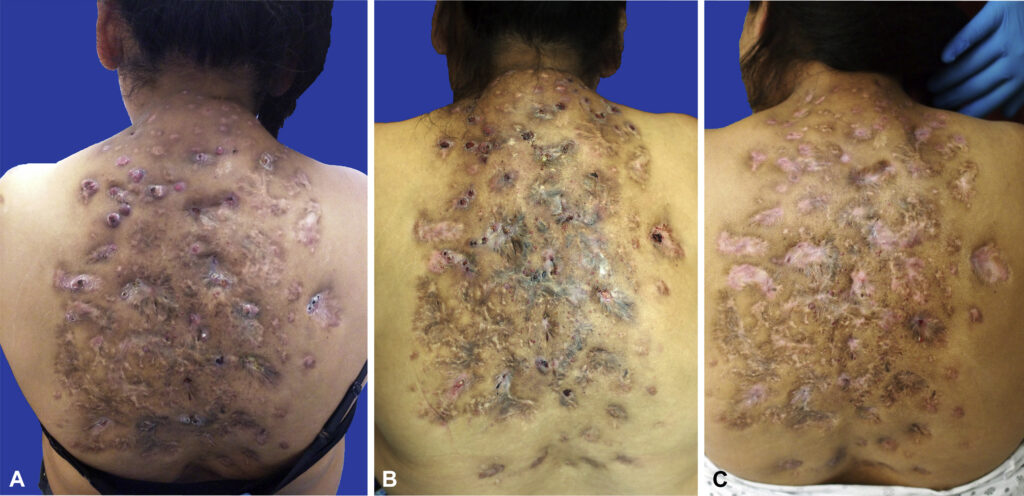
What Causes Nocardiosis?
The Nocardia Bacteria
- Nocardia species are found in soil, water, and decaying vegetation.
- Inhalation or direct contact with contaminated material leads to infection.
- Common pathogenic species include:
- Nocardia asteroides (most common cause of pulmonary nocardiosis)
- Nocardia brasiliensis (frequently associated with skin infections)
- Nocardia farcinica (known for disseminated infections)
Modes of Transmission
- Inhalation: Primary route leading to pulmonary nocardiosis.
- Direct skin contact: Entry through cuts or wounds, causing cutaneous nocardiosis.
- Hematogenous spread: Dissemination from the lungs to other organs, including the brain and kidneys.
Types and Their Symptoms
1. Pulmonary Nocardiosis
The most common form, pulmonary nocardiosis mimics other chronic lung infections such as tuberculosis.
Symptoms:
- Persistent cough (often with purulent sputum)
- Chest pain
- Shortness of breath
- Fever and night sweats
- Weight loss
2. Cutaneous Nocardiosis
Skin infection occurs after direct trauma or exposure to contaminated material.
Symptoms:
- Localized skin abscesses or ulcers
- Swollen lymph nodes
- Pus-filled lesions
3. Central Nervous System (CNS)
This occurs when Nocardia bacteria spread to the brain, leading to abscess formation.
Symptoms:
- Severe headaches
- Seizures
- Confusion and neurological deficits
- Nausea and vomiting
4. Disseminated
A severe, systemic infection affecting multiple organs. It typically begins as pulmonary before spreading through the bloodstream.
Symptoms:
- Multi-organ dysfunction
- Chronic fever
- Severe fatigue and weakness
Who Is at Risk for?
While nocardiosis can affect anyone, certain individuals are at higher risk, including:
- Immunocompromised patients (HIV/AIDS, cancer, organ transplant recipients)
- Individuals on long-term corticosteroids (e.g., prednisone therapy)
- Diabetics
- Patients with chronic lung disease (COPD, bronchiectasis)
- Those undergoing chemotherapy or immunosuppressive treatments
Diagnosis of Nocardiosis
1. Clinical Evaluation
- Detailed medical history and symptom assessment help in suspecting nocardiosis, especially in high-risk individuals.
2. Laboratory Tests
- Sputum culture, blood culture, or pus samples to isolate Nocardia species.
- Gram staining and modified acid-fast staining to identify filamentous, weakly acid-fast bacteria.
3. Imaging Studies
- Chest X-ray or CT scan: Detects lung nodules, cavitations, or infiltrates.
- MRI or CT of the brain: Identifies nocardial brain abscesses.
4. Molecular and Histopathological Techniques
- Polymerase Chain Reaction (PCR): Confirms Nocardia DNA in clinical samples.
- Biopsy and histopathology: Useful for deep tissue infections.
Treatment of Nocardiosis
1. Antibiotic Therapy
- Sulfonamides (e.g., Trimethoprim-Sulfamethoxazole [TMP-SMX]) are the first-line treatment.
- Alternative antibiotics for resistant cases:
- Linezolid
- Carbapenems (Imipenem, Meropenem)
- Amikacin
- Ceftriaxone
- Duration of Treatment:
- Pulmonary and cutaneous nocardiosis: 6–12 months
- Disseminated and CNS nocardiosis: 12 months or longer
2. Surgical Drainage
- Required for large abscesses (especially in the brain or skin).
3. Supportive Care
- Oxygen therapy for respiratory distress.
- Immunosuppressive medication adjustment in high-risk patients.
Prevention of Nocardiosis
1. Reducing Environmental Exposure
- Avoid inhalation of soil dust in construction or gardening activities.
- Use protective gloves when handling soil or organic matter.
2. Strengthening the Immune System
- Immunocompromised individuals should undergo regular health monitoring to detect infections early.
- Proper management of chronic diseases like diabetes and COPD.
3. Prophylactic Antibiotics in High-Risk Individuals
- Patients undergoing solid organ transplantation may receive TMP-SMX prophylaxis to reduce infection risk.
Prognosis of Nocardiosis
- Early diagnosis and appropriate treatment lead to a favorable prognosis.
- Untreated nocardiosis can result in serious complications, including brain abscesses and multi-organ failure.
- Immunocompromised patients require long-term follow-up to prevent relapse.
Nocardiosis is a serious bacterial infection primarily affecting the lungs, CNS, and skin. It poses a significant threat to immunocompromised individuals, with pulmonary and disseminated forms being particularly severe. Early recognition, accurate diagnosis, and prolonged antibiotic therapy are key to successful treatment. Awareness, preventive measures, and appropriate medical intervention can greatly reduce the risk and impact of this condition.