Neonatal bronchopulmonary dysplasia (BPD) is a chronic lung disease primarily affecting preterm infants who require prolonged oxygen therapy and mechanical ventilation. It results from lung immaturity, inflammation, and oxygen toxicity, leading to impaired alveolar development and long-term respiratory complications. Advances in neonatal intensive care have improved survival rates in very low birth weight (VLBW) infants, but BPD remains a significant cause of morbidity in preterm neonates.
Pathophysiology of BPD
BPD is characterized by disrupted lung development, leading to simplified alveolar structures, impaired vascularization, and chronic inflammation. The primary mechanisms include:
- Mechanical Ventilation Injury – High-pressure ventilation causes barotrauma and lung damage.
- Oxygen Toxicity – Prolonged exposure to high oxygen concentrations leads to oxidative stress and inflammation.
- Inflammatory Response – Prenatal infections, sepsis, and chorioamnionitis contribute to lung inflammation.
- Vascular Dysfunction – Pulmonary hypertension due to poor vascular growth worsens respiratory distress.
Causes and Risk Factors
1. Prematurity and Low Birth Weight
- Infants <30 weeks gestation are at the highest risk.
- Immature lungs lack surfactant, increasing susceptibility to lung injury.
2. Prolonged Mechanical Ventilation and Oxygen Therapy
- Mechanical ventilation damages fragile alveoli, leading to fibrosis.
- High oxygen levels generate free radicals, causing oxidative injury.
3. Infections and Inflammation
- Chorioamnionitis (intrauterine infection) increases neonatal inflammation.
- Postnatal sepsis and pneumonia exacerbate lung damage.
4. Nutritional Deficiencies
- Vitamin A deficiency is associated with impaired lung growth.
- Poor postnatal weight gain increases the risk of severe BPD.
5. Genetic and Environmental Factors
- Genetic predisposition may influence lung development.
- Exposure to pollutants (e.g., maternal smoking) worsens outcomes.
Clinical Presentation and Symptoms
1. Respiratory Distress in the NICU
- Persistent tachypnea (rapid breathing)
- Intermittent oxygen desaturation requiring supplemental oxygen
- Retractions and nasal flaring indicating increased respiratory effort
2. Oxygen Dependency Beyond 28 Days
- Preterm infants who require oxygen support for >28 days are likely developing BPD.
- Severity is classified based on oxygen and ventilatory needs at 36 weeks postmenstrual age (PMA).
3. Long-Term Pulmonary Symptoms
- Recurrent wheezing and bronchospasms
- Increased susceptibility to respiratory infections
- Exercise intolerance in later childhood
Diagnosis of BPD
1. Clinical and Radiological Criteria
BPD is diagnosed based on:
- Oxygen dependence for >28 days post-birth
- Severity assessment at 36 weeks PMA
- Chest X-ray or lung ultrasound showing chronic lung changes
2. Classification of BPD Severity
| Severity | Oxygen Requirement at 36 Weeks PMA | Ventilatory Support |
|---|---|---|
| Mild BPD | Room air | None |
| Moderate BPD | <30% oxygen | Nasal cannula or CPAP |
| Severe BPD | >30% oxygen | Mechanical ventilation |
3. Imaging and Pulmonary Function Tests
- Chest X-ray: Shows diffuse lung haziness and hyperinflation.
- CT Scan: Detects fibrotic lung changes in severe cases.
- Pulmonary function tests (PFTs): Used in older children to assess long-term lung function.
Treatment and Management of BPD
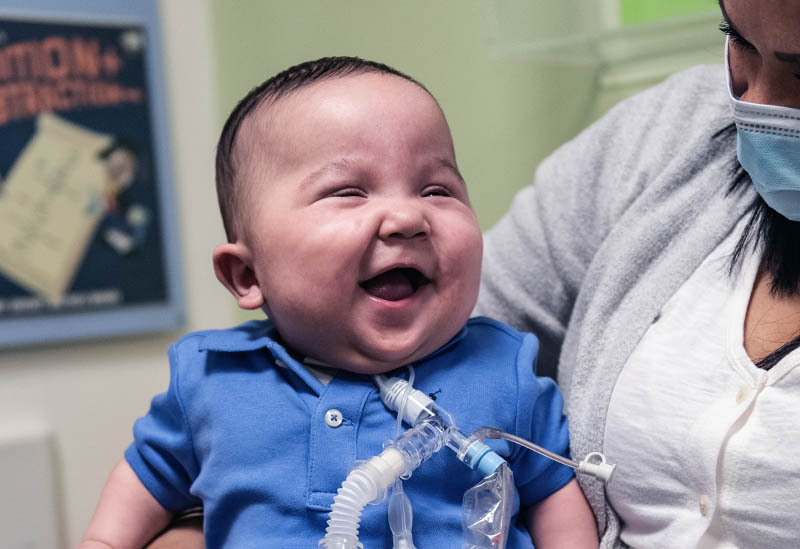
1. Oxygen Therapy and Respiratory Support
- Nasal Continuous Positive Airway Pressure (NCPAP) – Maintains alveolar recruitment.
- High-Flow Nasal Cannula (HFNC) – Reduces work of breathing.
- Mechanical Ventilation (Severe Cases) – Requires careful use to prevent ventilator-associated lung injury.
2. Pharmacological Management
- Caffeine Therapy – Stimulates breathing and reduces apnea episodes.
- Diuretics (Furosemide, Spironolactone) – Manage pulmonary edema.
- Corticosteroids (Dexamethasone, Budesonide) – Reduce inflammation, but long-term risks exist.
- Bronchodilators (Albuterol, Ipratropium) – Improve airway function in reactive airways.
3. Nutritional Support
- High-caloric intake promotes lung and tissue growth.
- Vitamin A supplementation improves lung development.
4. Infection Prevention
- Palivizumab (RSV prophylaxis) reduces severe infections.
- Routine vaccinations (Influenza, Pneumococcus) lower the risk of complications.
Prognosis and Long-Term Outcomes
1. Recovery Timeline
- Many infants wean off oxygen by 1-2 years of age.
- Severe BPD cases may develop chronic lung disease into childhood.
2. Long-Term Respiratory Risks
- Increased risk of asthma-like symptoms and exercise intolerance.
- Higher incidence of hospitalization for respiratory infections.
3. Neurodevelopmental Impact
- Infants with severe BPD have a higher risk of cognitive and motor delays.
- Early intervention programs improve developmental outcomes.
Prevention of BPD
1. Antenatal Strategies
- Antenatal corticosteroids (Betamethasone) enhance fetal lung maturation.
- Delayed cord clamping improves neonatal circulation and lung function.
2. Gentle Ventilation Approaches
- Non-invasive ventilation (NIV) reduces lung injury.
- Early surfactant therapy improves lung compliance.
3. Postnatal Care
- Minimizing oxygen toxicity by targeting optimal SpO2 levels (90-95%).
- Avoiding fluid overload to reduce pulmonary edema.
Bronchopulmonary dysplasia remains a significant challenge in neonatal care, particularly among preterm infants requiring prolonged respiratory support. Advances in gentle ventilation strategies, pharmacological interventions, and nutritional support have improved outcomes, but long-term pulmonary monitoring is essential. With early intervention and multidisciplinary follow-up, many BPD survivors lead healthy and active lives.