Neonatal apnea is a respiratory disorder in newborns characterized by temporary pauses in breathing lasting more than 20 seconds. It primarily affects preterm infants due to immature brainstem control of respiration. In some cases, oxygen desaturation and bradycardia (slow heart rate) accompany apnea, requiring immediate medical intervention.
This condition is classified into three types: apnea of prematurity (AOP), central apnea, and obstructive apnea. Proper diagnosis and timely treatment are essential to prevent long-term complications, including developmental delays and chronic lung issues.
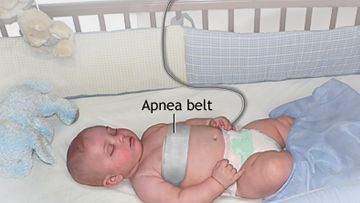
Types of Neonatal Apnea
1. Apnea of Prematurity (AOP)
- Occurs in infants born before 37 weeks gestation
- Caused by immature respiratory control in the brainstem
- Common in infants <30 weeks gestation, affecting up to 80% of extremely preterm neonates
- Improves as the infant’s nervous system matures, usually by 36-37 weeks postmenstrual age
2. Central Apnea
- Failure of respiratory effort due to temporary disruption of the brain’s breathing control center
- Common in neurologically compromised infants (e.g., hypoxic-ischemic encephalopathy, brain malformations)
- No chest movement observed during apneic episodes
3. Obstructive Apnea
- Occurs due to airway obstruction from floppy airway structures, secretions, or improper head positioning
- Seen in infants with craniofacial abnormalities (Pierre Robin sequence, micrognathia)
- Chest movement is present, but there is no airflow
4. Mixed Apnea
- A combination of central and obstructive apnea
- Represents the majority of cases in preterm infants
Causes and Risk Factors
1. Immaturity of the Respiratory System
- Underdeveloped brainstem control leads to irregular breathing patterns
- More common in very low birth weight (VLBW) infants (<1500g)
2. Neurological Disorders
- Hypoxic-ischemic encephalopathy (HIE)
- Intraventricular hemorrhage (IVH)
- Periventricular leukomalacia (PVL)
3. Metabolic and Infectious Causes
- Hypoglycemia, hypocalcemia, or electrolyte imbalances
- Sepsis, meningitis, or pneumonia can trigger apnea episodes
4. Respiratory Conditions
- Transient tachypnea of the newborn (TTN)
- Respiratory distress syndrome (RDS)
- Meconium aspiration syndrome (MAS)
5. Gastroesophageal Reflux Disease (GERD)
- Reflux-induced airway irritation may cause apnea episodes
Clinical Presentation and Symptoms
1. Common Signs of Neonatal Apnea
- Breathing pauses lasting >20 seconds
- Cyanosis (bluish skin discoloration)
- Bradycardia (heart rate <100 bpm)
- Hypotonia (decreased muscle tone)
2. Severe Symptoms Indicating Critical Apnea
- Prolonged desaturation (oxygen levels dropping below 85%)
- Unresponsiveness or limpness
- Recurrent apnea requiring resuscitation
Diagnosis of Neonatal Apnea
1. Clinical Evaluation
- Detailed birth history and gestational age assessment
- Observation of apnea episodes with timing, duration, and associated symptoms
2. Laboratory and Imaging Tests
| Test | Purpose |
|---|---|
| Blood Gas Analysis | Detects hypoxemia, hypercapnia |
| Blood Culture | Rules out sepsis or infection |
| Electrolyte Panel | Checks for metabolic imbalances |
| Brain Ultrasound (HUS) | Identifies IVH or PVL |
| Polysomnography (PSG) | Assesses sleep-related apnea patterns |
3. Continuous Monitoring in NICU
- Cardiorespiratory monitoring to detect bradycardia and oxygen desaturation
- Pulse oximetry and capnography for real-time tracking of oxygen levels
Treatment and Management of Neonatal Apnea
1. Supportive Care and Monitoring
- Positioning: Keeping the infant’s head in a neutral position to prevent airway obstruction
- Thermal regulation: Avoiding hypothermia, which can trigger apnea
2. Pharmacological Treatment
- Caffeine citrate (first-line treatment)
- Stimulates the central respiratory drive
- Reduces apnea episodes by 50-70%
- Typically given until 34-35 weeks postmenstrual age
- Theophylline (alternative therapy)
- Less commonly used due to narrower therapeutic window
3. Respiratory Support
- Nasal Continuous Positive Airway Pressure (NCPAP)
- Prevents airway collapse in obstructive or mixed apnea
- Improves lung recruitment in preterm infants
- High-Flow Nasal Cannula (HFNC)
- Provides gentle positive airway pressure
- Mechanical Ventilation (for severe cases)
- Required if apnea is refractory to caffeine and NCPAP
4. Managing Apnea Due to GERD
- Thickened feeds or anti-reflux positioning
- Proton pump inhibitors (PPIs) only in selected cases
Prognosis and Long-Term Outcomes
1. Recovery Timeline
- Apnea of prematurity resolves by 36-37 weeks gestation
- No long-term effects in mild cases
2. Risk of Neurodevelopmental Impairments
- Infants with severe apnea requiring intubation may have:
- Cognitive delays
- Motor dysfunction
- Increased risk of SIDS (sudden infant death syndrome)
3. Follow-Up Recommendations
- Neonatal follow-up clinic visits to monitor developmental progress
- Sleep studies for persistent apnea beyond term gestation
Neonatal apnea is a common yet serious condition, particularly in preterm infants, requiring continuous monitoring and early intervention. Caffeine therapy and respiratory support significantly improve outcomes, while long-term follow-up ensures normal neurological development. Advances in NICU care and apnea management protocols continue to reduce complications and improve survival rates for vulnerable neonates.