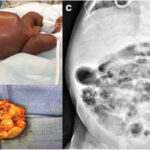
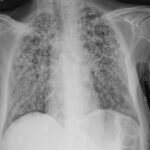
Necrotizing fasciitis streptococcus infection: Necrotizing fasciitis (NF) is a rapidly progressing bacterial infection that destroys the soft tissues and fascia, leading to severe complications if not treated promptly. Often referred to as a “flesh-eating” disease, necrotizing fasciitis is commonly caused by Group A Streptococcus (GAS), though other bacterial strains can contribute. Immediate medical intervention is critical to prevent systemic complications, sepsis, and death.
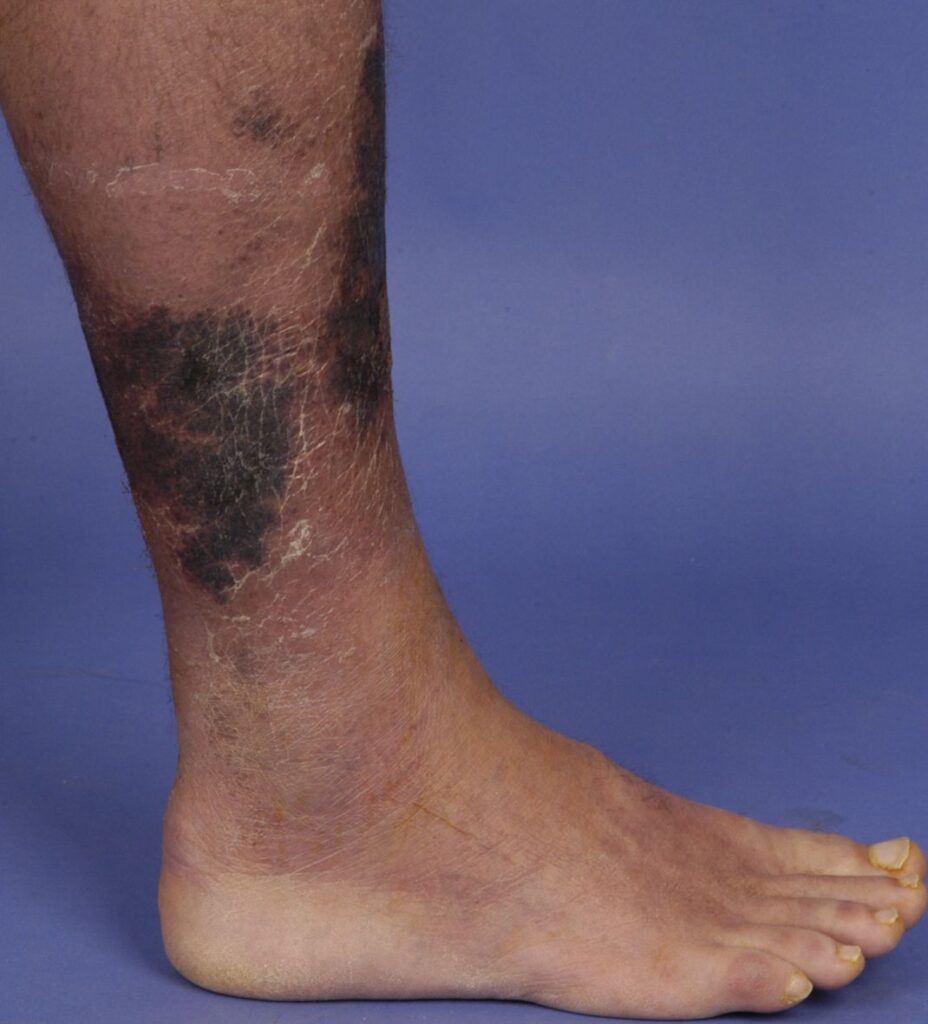
Causes and Risk Factors
Necrotizing fasciitis occurs when bacteria enter the body through cuts, surgical wounds, or blunt trauma. Several risk factors increase susceptibility to infection.
1. Common Causative Bacteria
- Group A Streptococcus (GAS) – The primary cause of necrotizing fasciitis.
- Clostridium species – Produces toxins that accelerate tissue destruction.
- Klebsiella, Escherichia coli, Pseudomonas aeruginosa – Common in polymicrobial infections.
2. Risk Factors
- Weakened immune system (e.g., diabetes, cancer, chronic diseases)
- Recent surgery or trauma (open wounds, burns, or surgical incisions)
- Intravenous drug use
- Obesity (linked to poor circulation and wound healing)
- Peripheral vascular disease (limits blood supply to affected tissues)
Symptoms of Necrotizing Fasciitis
Early symptoms can resemble less severe infections, making prompt recognition critical.
- Severe pain disproportionate to the visible wound
- Swelling, redness, and warmth at the infection site
- Rapidly spreading tissue damage
- Skin discoloration (purplish, dark patches indicating necrosis)
- Blisters and fluid-filled lesions
- Fever, chills, and nausea
- Hypotension and shock in advanced cases
Diagnosis of Necrotizing Fasciitis
Early diagnosis is essential to prevent severe complications.
1. Clinical Examination
Physicians assess symptoms, including pain severity, skin changes, and systemic signs of infection.
2. Imaging Tests
- X-rays or CT scans – Detect gas in soft tissues, a hallmark of necrotizing infections.
- MRI – Identifies deep tissue involvement and fluid accumulation.
3. Laboratory Tests
- Complete Blood Count (CBC) – Elevated white blood cell count indicates infection.
- C-reactive protein (CRP) – Increased levels signal inflammation.
- Blood cultures – Identify bacterial strains responsible for infection.
Treatment of Necrotizing Fasciitis
Necrotizing fasciitis is a medical emergency requiring aggressive treatment.
1. Surgical Debridement
Immediate removal of infected tissue is essential to prevent bacterial spread.
2. Broad-Spectrum Antibiotics
- Initial IV antibiotics target Streptococcus and other bacteria.
- Common regimens include penicillin, clindamycin, and carbapenems.
3. Intravenous Fluids & Critical Care
Patients often require intensive care, including IV hydration and vasopressors for shock management.
4. Hyperbaric Oxygen Therapy (HBOT)
Some cases benefit from high-pressure oxygen therapy to reduce bacterial load and promote tissue healing.
5. Amputation (Severe Cases)
If gangrene or severe tissue necrosis occurs, limb amputation may be necessary.
Complications of Necrotizing Fasciitis
Even with treatment, complications may arise.
1. Sepsis and Septic Shock
Bacteria can enter the bloodstream, leading to life-threatening multi-organ failure.
2. Limb Loss and Permanent Disfigurement
Severe tissue destruction may require amputation or extensive reconstructive surgery.
3. Long-Term Nerve and Muscle Damage
Loss of function in affected limbs may require physical therapy.
4. Post-Infection Psychological Impact
Survivors may suffer from post-traumatic stress disorder (PTSD) and depression.
Prevention of Necrotizing Fasciitis
Although rare, preventive measures can significantly reduce the risk of developing necrotizing fasciitis.
1. Proper Wound Care
- Clean all cuts and wounds thoroughly with soap and water.
- Use antiseptic solutions and keep wounds covered until healed.
2. Hand Hygiene and Infection Control
- Frequent handwashing minimizes bacterial transmission.
- Avoiding contaminated water in open wounds reduces infection risk.
3. Managing Underlying Health Conditions
- Control diabetes and maintain proper circulation and immunity.
- Avoid high-risk behaviors such as intravenous drug use.
4. Early Medical Intervention
Seeking immediate treatment for unexplained pain, swelling, or fever can prevent severe progression.
Necrotizing fasciitis caused by Streptococcus is a deadly bacterial infection requiring rapid medical intervention. Early symptoms often mimic less severe conditions, making immediate diagnosis and treatment crucial. Surgical debridement, antibiotics, and critical care are essential to prevent fatal complications. Prevention through proper wound care, hygiene, and early medical attention remains the most effective strategy in reducing mortality.