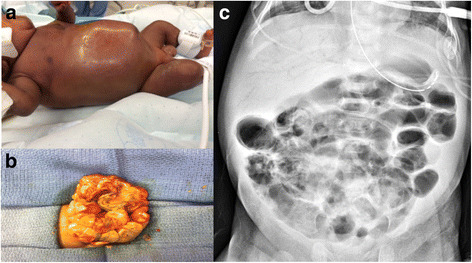
Necrotizing enterocolitis (NEC) is a severe and potentially life-threatening gastrointestinal disease that primarily affects premature and low-birth-weight infants. This condition leads to inflammation and necrosis (tissue death) of the intestinal lining, which can result in perforation and systemic infection. NEC is one of the most common and serious gastrointestinal disorders in neonatal intensive care units (NICUs), with significant morbidity and mortality rates.
Causes and Risk Factors
While the exact cause of NEC is not fully understood, several contributing factors increase the risk of developing this disease.
1. Prematurity
Premature infants, particularly those born before 32 weeks of gestation, have an underdeveloped digestive system, making them more susceptible to NEC.
2. Feeding Practices
- Formula feeding: Studies suggest that formula-fed infants have a higher risk of developing NEC compared to those who receive breast milk.
- Enteral feeding: Rapid introduction of large feeding volumes may contribute to NEC development.
3. Intestinal Ischemia
Reduced blood flow to the intestines can cause tissue damage and increase the risk of NEC.
4. Bacterial Overgrowth
An imbalance in the gut microbiota may lead to increased inflammation and bacterial invasion of the intestinal wall.
5. Immature Immune System
A premature baby’s immune system is not fully developed, making it less capable of fighting infections and inflammation.
Symptoms of NEC
NEC can present with a range of symptoms, varying in severity. Early detection is critical for effective management.
- Abdominal distension (swollen belly)
- Feeding intolerance (vomiting, difficulty digesting food)
- Bloody stools (indicating intestinal damage)
- Lethargy and poor feeding
- Temperature instability
- Apnea and bradycardia (pauses in breathing and slow heart rate)
- Signs of sepsis (low blood pressure, pale or mottled skin)
Diagnosis of NEC
Timely diagnosis is crucial for preventing complications. Physicians use a combination of clinical symptoms, laboratory tests, and imaging studies.
1. Clinical Assessment
Doctors assess the infant’s symptoms, feeding tolerance, and overall condition.
2. Imaging Tests
- Abdominal X-rays: Show signs of bowel wall thickening, gas accumulation, or perforation.
- Ultrasound: Detects fluid in the abdominal cavity and bowel integrity.
3. Laboratory Tests
- Complete Blood Count (CBC): Low platelet count and signs of infection.
- Blood Culture: Identifies bacterial infections.
- C-reactive protein (CRP): Indicates inflammation.
Treatment of NEC
The treatment approach depends on the severity of NEC, ranging from medical management to surgical intervention.
1. Supportive Care (For Mild Cases – Stage I & II)
- Bowel rest: Stopping oral feedings to allow the intestines to heal.
- Nasogastric decompression: Inserting a tube to remove gas and fluids from the stomach.
- Intravenous (IV) fluids: Providing nutrition and hydration.
- Antibiotic therapy: Preventing or treating infection.
- Monitoring: Regular imaging and lab tests to assess progress.
2. Surgical Intervention (For Severe Cases – Stage III)
If the intestine is perforated or necrotic, surgery is necessary to remove the damaged sections.
- Peritoneal drainage: For critically ill infants who are too unstable for surgery.
- Bowel resection: Removing necrotic sections of the intestine.
- Ostomy: Creating a temporary opening in the abdomen to allow stool to exit the body safely.
Complications of NEC
Even with treatment, NEC can lead to serious long-term complications.
1. Short Bowel Syndrome (SBS)
If large sections of the intestine are removed, nutrient absorption is impaired, requiring long-term nutritional support.
2. Intestinal Strictures
Healing from NEC may lead to scar tissue formation, narrowing the intestines and causing feeding difficulties.
3. Neurodevelopmental Delays
NEC survivors, especially those who undergo surgery, have a higher risk of developmental disabilities.
4. Increased Mortality Risk
Severe NEC can lead to life-threatening infections and organ failure, particularly in very low birth-weight infants.
Prevention Strategies
Preventing NEC is a key focus in neonatal care.
1. Breastfeeding
Human milk has protective properties that reduce NEC risk due to its beneficial antibodies and prebiotics.
2. Probiotics
Some studies suggest that probiotic supplements may help balance gut bacteria and reduce inflammation.
3. Controlled Feeding Practices
Gradual feeding introduction and monitoring for intolerance can help prevent NEC.
4. Infection Control
Strict hygiene and infection prevention protocols in NICUs reduce bacterial exposure.
5. Corticosteroids for Lung Maturity
Prenatal corticosteroids help mature the baby’s lungs and digestive system, reducing NEC risk.
Necrotizing enterocolitis is a serious neonatal condition that requires early detection, careful monitoring, and prompt treatment. Premature and low-birth-weight infants are at the highest risk, and supportive medical management or surgery may be required to manage the disease. Preventive measures such as breastfeeding, controlled feeding, and infection control play a crucial role in reducing NEC incidence. Continued research and advancements in neonatal care remain vital to improving outcomes for affected infants.