Mycosis fungoides (MF) is a rare type of non-Hodgkin’s lymphoma that primarily affects the skin. It is classified as a cutaneous T-cell lymphoma (CTCL), where malignant T-cells accumulate in the skin, causing chronic and progressive skin lesions. While the disease advances slowly, early diagnosis and treatment are essential for managing symptoms and preventing complications.
Causes and Risk Factors
The exact cause of mycosis fungoides remains unknown, but certain factors may contribute to its development:
- Genetic mutations – Abnormal changes in T-cells may trigger malignancy.
- Chronic immune system dysfunction – Individuals with weakened immune responses may be at higher risk.
- Environmental exposure – Exposure to certain chemicals or infections might play a role.
- Viral infections – Some studies suggest a link between human T-lymphotropic virus (HTLV-1) and CTCL.
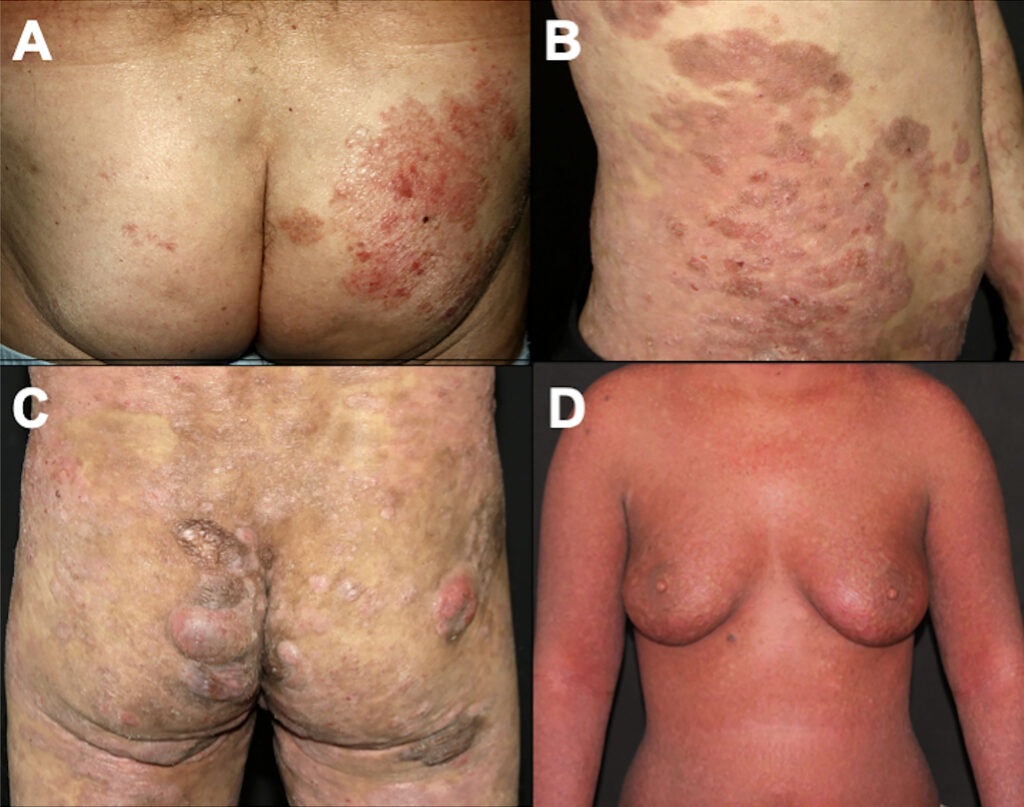
Stages and Symptoms of Mycosis Fungoides
Mycosis fungoides progresses in distinct stages, each characterized by different skin changes and severity levels.
1. Patch Stage (Early Stage)
- Flat, scaly, and itchy skin patches
- Often mistaken for eczema or psoriasis
- Common on areas like the buttocks, thighs, and lower back
2. Plaque Stage
- Thick, raised, reddish-brown lesions
- More persistent and widespread compared to patches
- May cause discomfort and mild pain
3. Tumor Stage
- Large nodular tumors develop on the skin
- Risk of ulceration and secondary infections
- May spread to deeper tissues
4. Advanced Stage (Systemic Involvement & Sezary Syndrome)
- Cancer spreads to lymph nodes, blood, and internal organs
- Sezary Syndrome: A more aggressive form of CTCL with circulating malignant T-cells in the blood, leading to erythroderma (generalized redness and scaling of the skin)
Diagnosis of Mycosis Fungoides
1. Clinical Examination
A dermatologist evaluates the appearance and distribution of skin lesions.
2. Skin Biopsy
A small sample of affected skin is examined under a microscope to detect abnormal T-cell infiltration.
3. Immunohistochemistry and Flow Cytometry
- Identifies CD4+ T-cell markers associated with mycosis fungoides.
4. Blood Tests (Peripheral Blood Analysis)
- Detects Sezary cells in cases of Sezary syndrome.
5. Imaging Tests
- CT scan & PET scan: Determines the extent of systemic spread.
Treatment Options for Mycosis Fungoides
1. Topical Therapies (For Early Stages)
- Corticosteroids – Reduces inflammation and itching.
- Topical chemotherapy (Mechlorethamine, Carmustine) – Targets cancerous skin cells.
- Phototherapy (PUVA, UVB) – Uses ultraviolet light to slow disease progression.
2. Systemic Treatments (For Advanced Stages)
- Oral retinoids (Bexarotene, Acitretin) – Helps regulate T-cell function.
- Targeted therapy (Mogamulizumab, Brentuximab vedotin) – Monoclonal antibodies targeting malignant cells.
- Chemotherapy (Methotrexate, Doxorubicin) – Used for aggressive or refractory cases.
3. Radiation Therapy
Localized radiation may be effective in reducing tumors and alleviating symptoms.
4. Stem Cell Transplantation
For patients with severe disease progression, stem cell transplants offer potential long-term remission.
Prognosis and Life Expectancy
The prognosis of mycosis fungoides depends on the stage at diagnosis:
- Early-stage patients – Often live for decades with proper management.
- Advanced-stage patients – Require aggressive treatment but can achieve remission with targeted therapies.
Mycosis fungoides is a rare but manageable cutaneous lymphoma. Early diagnosis, stage-appropriate treatment, and continuous monitoring can significantly improve patient outcomes.