Mycobacteriosis refers to infections caused by non-tuberculous mycobacteria (NTM), a diverse group of bacteria found in soil, water, and dust. Unlike Mycobacterium tuberculosis, which causes tuberculosis, NTM infections are not contagious but can lead to chronic pulmonary disease, skin infections, and disseminated disease in immunocompromised individuals.
Types of Mycobacteria Causing Mycobacteriosis
Non-tuberculous mycobacteria are classified into slow-growing and rapid-growing species:
1. Slow-Growing Mycobacteria
- Mycobacterium avium complex (MAC) – the most common cause of pulmonary infections
- Mycobacterium kansasii – associated with lung disease similar to tuberculosis
- Mycobacterium marinum – responsible for skin and soft tissue infections
- Mycobacterium ulcerans – causes Buruli ulcer, a severe skin disease
2. Rapid-Growing Mycobacteria
- Mycobacterium abscessus – highly resistant to antibiotics, affecting lungs, skin, and soft tissues
- Mycobacterium fortuitum – causes skin and post-surgical infections
- Mycobacterium chelonae – associated with wound and catheter-related infections
Causes and Risk Factors of Mycobacteriosis
Mycobacteria are environmental pathogens that infect individuals through inhalation, ingestion, or direct skin contact.
1. Risk Factors for Pulmonary Mycobacteriosis
- Pre-existing lung diseases (COPD, bronchiectasis, cystic fibrosis)
- Long-term smoking history
- Weakened immune system (HIV/AIDS, immunosuppressive therapy)
- Advanced age
2. Risk Factors for Skin and Soft Tissue Infections
- Open wounds or injuries exposed to contaminated water
- Cosmetic procedures (tattoos, liposuction, mesotherapy)
- Surgical implants and catheters
3. Risk Factors for Disseminated Mycobacteriosis
- Severe immunosuppression, especially in HIV/AIDS patients
- Long-term steroid or immunosuppressant use
Symptoms of Mycobacteriosis
The symptoms of mycobacteriosis vary depending on the site of infection.
1. Pulmonary Mycobacteriosis
- Chronic cough with mucus or blood
- Shortness of breath
- Fatigue and weight loss
- Night sweats and low-grade fever
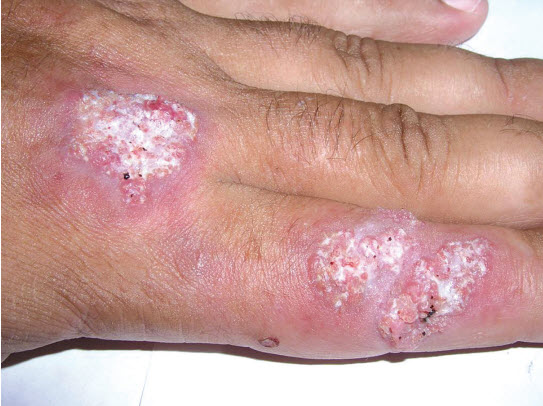
2. Cutaneous Mycobacteriosis
- Skin nodules or abscesses
- Ulcers with draining pus
- Non-healing wounds
3. Disseminated Mycobacteriosis
- Fever and chills
- Severe fatigue
- Organ dysfunction (liver, spleen, bone marrow involvement)
Diagnosis of Mycobacteriosis
1. Laboratory Testing
- Sputum culture and acid-fast bacilli (AFB) staining
- PCR-based molecular testing for species identification
2. Imaging Studies
- Chest X-ray or CT scan to detect lung infections
- Ultrasound or MRI for soft tissue infections
3. Biopsy and Histopathology
- Tissue samples for granuloma detection in skin and organ involvement
Treatment of Mycobacteriosis
The treatment approach depends on the mycobacterial species, infection severity, and patient health status.
1. Antibiotic Therapy
- MAC infection: Clarithromycin or azithromycin combined with ethambutol and rifampin
- M. kansasii infection: Rifampin, isoniazid, and ethambutol
- M. abscessus infection: Amikacin, imipenem, cefoxitin, and macrolides
2. Surgical Intervention
- Lung resection in severe pulmonary infections
- Drainage of abscesses in cutaneous mycobacteriosis
3. Supportive Care
- Pulmonary rehabilitation for lung function improvement
- Nutritional support to combat weight loss and malnutrition
Prognosis and Prevention
1. Prognosis
- Pulmonary mycobacteriosis can be chronic but manageable with long-term treatment.
- Skin infections often resolve with appropriate therapy.
- Disseminated infections require aggressive treatment due to high mortality risk.
2. Prevention Strategies
- Avoid exposure to contaminated water sources
- Proper sterilization of medical and cosmetic equipment
- Early treatment of lung diseases to reduce susceptibility
Mycobacteriosis is a challenging disease that requires early diagnosis and tailored treatment. Advances in molecular diagnostics and antibiotic regimens have improved patient outcomes, but vigilance in prevention remains crucial.