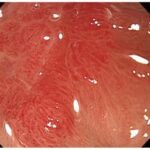
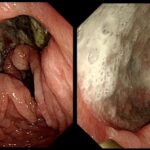
Erosive esophagitis is a severe form of gastroesophageal reflux disease (GERD) characterized by inflammation and erosion of the esophageal lining due to prolonged acid exposure. If left untreated, it can lead to complications such as esophageal strictures, ulcers, and Barrett’s esophagus. After initial treatment, maintaining the healing of erosive esophagitis is essential to prevent recurrence and further damage.
Key Strategies for Maintenance Therapy
1. Pharmacological Management
The cornerstone of long-term management is acid suppression therapy. The most effective medications include:
Proton Pump Inhibitors (PPIs)
- Omeprazole, lansoprazole, esomeprazole, and pantoprazole are commonly prescribed.
- PPIs reduce gastric acid production, allowing the esophagus to heal.
- Long-term use should be monitored due to potential side effects such as osteoporosis and vitamin deficiencies.
H2 Receptor Antagonists (H2RAs)
- Famotidine and ranitidine (where available) can be considered for patients with mild symptoms or those requiring step-down therapy from PPIs.
- Less effective than PPIs but beneficial for nighttime acid suppression.
Antacids and Alginate Therapy
- Provide immediate symptom relief but do not promote long-term healing.
- Often used as adjunct therapy for breakthrough symptoms.
2. Dietary Modifications
Adopting an esophagus-friendly diet can significantly reduce the recurrence of symptoms:
- Avoid trigger foods: Spicy foods, citrus fruits, tomatoes, caffeine, alcohol, and chocolate.
- Consume alkaline foods: Bananas, melons, oatmeal, and lean proteins help neutralize stomach acid.
- Eat smaller, frequent meals: Reduces stomach distension and acid reflux episodes.
- Limit late-night eating: Avoid eating at least three hours before bedtime to prevent nocturnal reflux.
3. Lifestyle Changes
Certain habits can exacerbate reflux and should be modified:
- Maintain a healthy weight: Excess weight increases intra-abdominal pressure, worsening reflux.
- Elevate the head of the bed: Using a wedge pillow or raising the bed frame can prevent acid reflux during sleep.
- Avoid smoking and alcohol: Both relax the lower esophageal sphincter, allowing acid to escape into the esophagus.
- Practice good posture: Sitting upright after meals and avoiding tight clothing around the abdomen can reduce reflux episodes.
4. Regular Monitoring and Follow-up
Patients with a history of erosive esophagitis should undergo periodic evaluation:
- Endoscopic surveillance: Recommended for patients with persistent symptoms or complications.
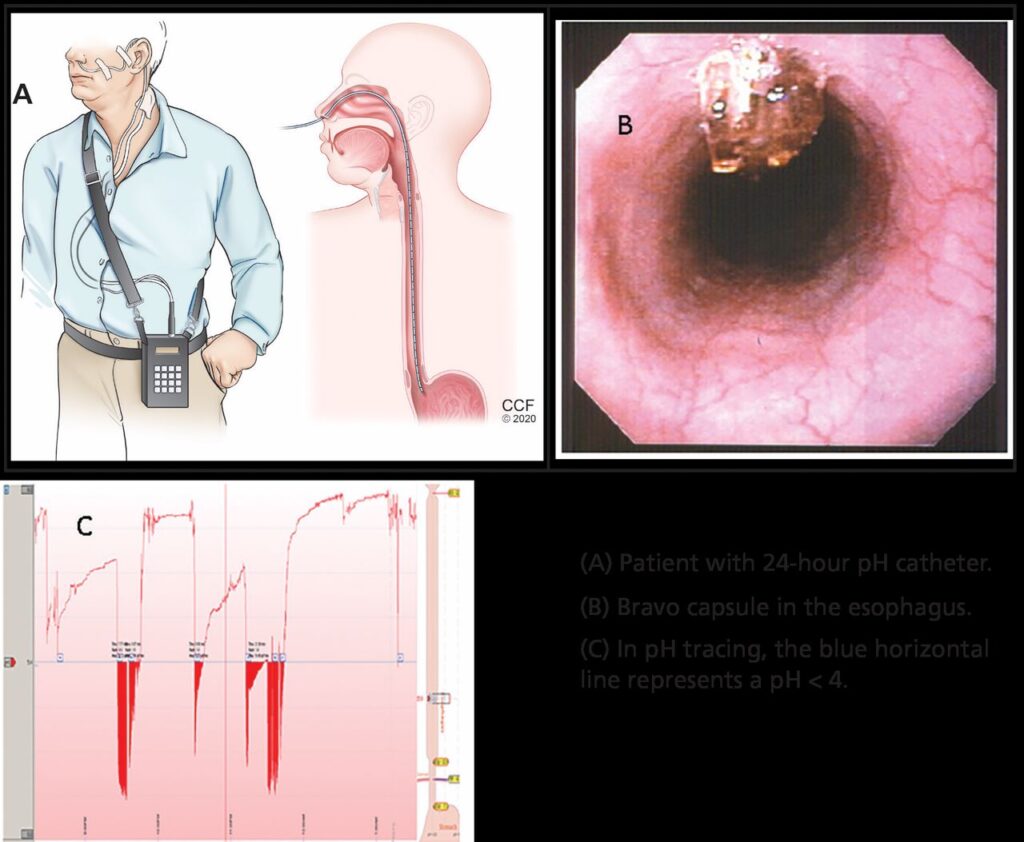
- pH Monitoring and Manometry: Used in refractory cases to assess acid exposure and esophageal motility.
- Adjustment of Therapy: Physicians may alter medication regimens based on symptom control and side effects.
5. Alternative and Adjunct Therapies
While medical therapy remains the primary treatment, some patients explore additional options:
- Probiotics: May help in maintaining gut health and reducing symptoms.
- Herbal remedies: Licorice root, chamomile, and aloe vera are believed to soothe the esophagus, though evidence is limited.
- Acupuncture and Stress Management: Can help reduce symptoms in some individuals.
Complications of Poor Maintenance
Failing to maintain healing can lead to severe complications, including:
- Barrett’s Esophagus: A precancerous condition requiring careful monitoring.
- Esophageal Strictures: Narrowing of the esophagus due to scarring, leading to swallowing difficulties.
- Recurrent Ulcers: Increased risk of bleeding and further esophageal damage.
Long-term maintenance of healing erosive esophagitis requires a combination of pharmacological therapy, dietary changes, lifestyle modifications, and ongoing medical monitoring. Patients should work closely with healthcare providers to tailor an appropriate maintenance plan, ensuring sustained esophageal health and reducing the risk of complications. By implementing these strategies, individuals can achieve lasting relief and improved quality of life.