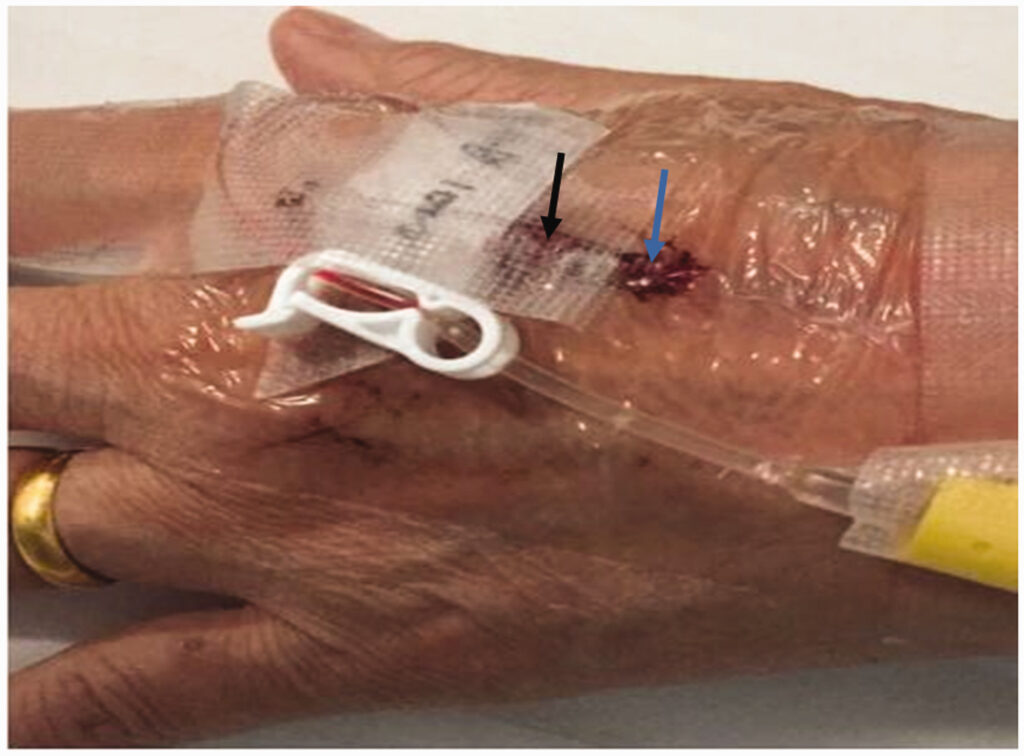
The patency of an indwelling intravenous (IV) catheter is crucial for effective medication administration, fluid therapy, and patient care. Ensuring an unobstructed flow minimizes complications such as occlusion, infection, and thrombosis. This guide outlines best practices, preventive strategies, and troubleshooting techniques to maintain catheter patency.
Understanding Indwelling IV Catheter Patency
IV catheter patency refers to the catheter’s ability to maintain an unobstructed flow of fluids and medications. Loss of patency can lead to serious complications, including treatment delays and increased infection risk.
Factors Affecting IV Catheter Patency
- Thrombotic Occlusion: Blood clot formation can obstruct flow.
- Mechanical Obstruction: Kinks or clamped tubing may impede fluid passage.
- Precipitation of Medications: Incompatible drug combinations can form deposits within the catheter.
- Biofilm Formation: Bacterial colonization can lead to infections and occlusion.
Best Practices for Maintaining IV Catheter Patency
1. Proper Flushing Techniques
- Use Normal Saline: 10 mL saline flush before and after medication administration.
- Pulsatile Flushing (Push-Pause Technique): Helps dislodge small clots and prevent buildup.
- Volume Considerations: Use sufficient volume to clear the catheter lumen effectively.
2. Heparin Lock for Long-Term Use
- Low-Dose Heparin Solution: Prevents clot formation in central venous catheters.
- Frequency: Follow institutional guidelines, typically every 8–12 hours for idle catheters.
3. Regular Monitoring and Assessment
- Visual Inspection: Look for redness, swelling, or leakage.
- Aspiration Test: Check for blood return before administration.
- Flow Rate Verification: Ensure adequate flow without resistance.
4. Proper Dressing and Securement
- Transparent Dressings: Allow easy visual monitoring.
- Securement Devices: Prevent movement and accidental dislodgement.
- Routine Dressing Changes: Follow aseptic techniques and change as per protocol.
5. Avoiding Medication Incompatibilities
- Check Compatibility Charts: Prevent precipitate formation.
- Flush Between Different Medications: Reduces chemical interactions.
6. Prevention of Catheter-Associated Infections
- Hand Hygiene: Essential before handling the catheter.
- Aseptic Technique: Use sterile gloves and disinfecting caps.
- Site Rotation: Change peripheral IV catheters every 72–96 hours.
Troubleshooting IV Catheter Occlusions
1. Identifying Occlusion Type
| Occlusion Type | Symptoms | Recommended Action |
|---|---|---|
| Thrombotic | Resistance to flushing, absent blood return | Administer thrombolytic agent |
| Mechanical | Kinks, clamped tubing, misplaced catheter | Reposition, unclamp tubing |
| Medication Precipitate | White, cloudy deposits | Use enzymatic declogging agents |
2. Declogging Techniques
- Syringe Aspiration: Attempt to withdraw blockage before flushing.
- Thrombolytics: Use low-dose alteplase for persistent thrombotic occlusions.
- Enzyme-Based Solutions: Dissolve medication precipitates effectively.
Maintaining the patency of an indwelling IV catheter is essential for patient safety and effective treatment. By following evidence-based flushing protocols, monitoring for occlusion signs, and preventing infections, healthcare providers can ensure seamless IV therapy and reduce complications.
Frequently Asked Questions:
1. How often should an IV catheter be flushed?
Peripheral IV catheters should be flushed every 8–12 hours when not in use, while central lines may require heparin locks at prescribed intervals.
2. What is the best way to prevent IV catheter occlusion?
Using a push-pause flushing technique with normal saline, ensuring correct securement, and monitoring for occlusion signs help prevent blockages.
3. Can heparin locks be used for all IV catheters?
Heparin locks are primarily used for central venous catheters, while normal saline is preferred for peripheral IV maintenance.
4. What should be done if an IV catheter becomes blocked?
Assess for mechanical kinks first. If the blockage persists, aspiration, thrombolytics, or enzymatic declogging agents may be required.
5. Why is the push-pause flushing technique recommended?
The push-pause method creates turbulence within the catheter lumen, helping to prevent clot formation and buildup of medication residues.