Nosocomial Pneumonia Due to Serratia marcescens: Nosocomial pneumonia, also referred to as hospital-acquired pneumonia (HAP), is a serious and potentially fatal infection occurring 48 hours or more after hospital admission. Among its causative agents, Serratia marcescens, a gram-negative, facultative anaerobic bacillus from the Enterobacteriaceae family, poses a growing clinical challenge due to its ability to develop multidrug resistance and its propensity to cause severe pulmonary infections, particularly in immunocompromised patients and those on mechanical ventilation.
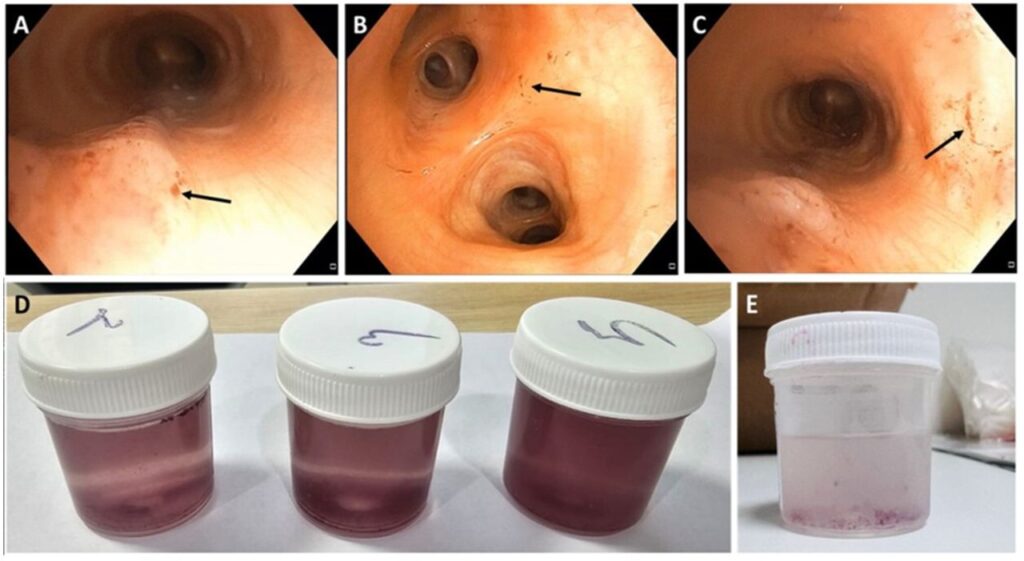
Epidemiology and Risk Factors
Serretia marcescens accounts for a minority of nosocomial pneumonia cases but is associated with high morbidity due to resistance to multiple classes of antibiotics. It is frequently isolated in intensive care units (ICUs) and is associated with the following risk factors:
- Mechanical ventilation (Ventilator-Associated Pneumonia – VAP)
- Prolonged hospitalization
- Immunosuppression or underlying malignancy
- Use of broad-spectrum antibiotics
- Indwelling medical devices (e.g., endotracheal tubes, catheters)
- Recent thoracic surgery or trauma
Pathogenesis and Virulence Mechanisms
Serratia marcescens exhibits several virulence factors that facilitate pulmonary infection:
- Adhesins: Facilitate colonization of respiratory epithelium.
- Lipopolysaccharide (LPS): Induces inflammation and disrupts alveolar barriers.
- Proteases and Hemolysins: Damage host tissue and interfere with immune responses.
- Biofilm Formation: Enhances resistance to antibiotics and immune clearance.
- AmpC β-lactamase Production: Confers resistance to β-lactam antibiotics.
Clinical Manifestations
Nosocomial pneumonia caused by Serratia marcescens often presents with:
- Fever and chills
- Cough with purulent sputum
- Dyspnea and hypoxia
- Leukocytosis or leukopenia
- Radiographic evidence of new infiltrates
- Signs of sepsis or acute respiratory distress syndrome (ARDS) in severe cases
In ventilated patients, a sudden decline in oxygenation or increase in respiratory secretions may be early indicators.
Diagnostic Evaluation
A timely and accurate diagnosis is crucial to improving outcomes in patients with Serratia marcescens pneumonia.
Recommended Diagnostic Tools:
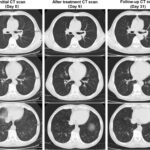
- Chest X-ray / CT scan: To identify new or progressive infiltrates
- Sputum Culture / Tracheal Aspirates / BAL Fluid: For microbial identification and sensitivity testing
- Blood cultures: To detect bacteremia
- PCR-based assays / MALDI-TOF MS: For rapid pathogen identification
- Procalcitonin levels: May help differentiate bacterial pneumonia from non-infectious causes
Early microbiological confirmation is essential to guide appropriate antibiotic therapy and reduce the misuse of broad-spectrum agents.
Antimicrobial Resistance Patterns
Serratia marcescens is intrinsically resistant to:
- Ampicillin
- First-generation cephalosporins
- Macrolides
It may also acquire resistance to:
- Carbapenems (via carbapenemase production)
- Fluoroquinolones
- Aminoglycosides
- Extended-spectrum β-lactamases (ESBLs)
Resistance mechanisms include porin loss, efflux pumps, and plasmid-mediated gene acquisition, making susceptibility testing essential.
Treatment Strategies
Empirical Therapy
Initial empiric therapy should consider local antibiogram data and include agents active against gram-negative bacilli. Common options:
- Carbapenems (e.g., meropenem) – especially in ESBL-producing strains
- Piperacillin-tazobactam
- Cefepime or Ceftazidime
- Aminoglycosides (e.g., amikacin) in combination regimens
- Polymyxins (e.g., colistin) for carbapenem-resistant isolates
Definitive Therapy
Tailor antibiotics based on culture and sensitivity results. De-escalation to monotherapy is recommended once the organism is confirmed and patient shows clinical improvement.
Duration of Therapy
- 7–14 days is standard
- Longer courses may be required for patients with abscesses, empyema, or slow clinical response
Infection Control and Prevention
Preventing Serratia marcescens pneumonia is essential to reducing morbidity and hospital costs. Recommended measures include:
- Strict hand hygiene protocols
- Sterilization of respiratory equipment
- Minimizing duration of mechanical ventilation
- Elevating head of the bed (30–45°) to prevent aspiration
- Closed suctioning systems in ventilated patients
- Regular surveillance cultures in ICUs
- Antibiotic stewardship programs to prevent the emergence of resistance
Prognosis and Outcomes
The prognosis of patients with Serratia marcescens-related nosocomial pneumonia varies by underlying health, timeliness of intervention, and resistance profile. Mortality rates range from 20% to 50% in severe cases, particularly in ventilator-associated pneumonia and in immunocompromised individuals.
Early diagnosis, effective antimicrobial therapy, and rigorous infection control can significantly improve patient outcomes.
Nosocomial pneumonia due to Serratia marcescens remains a clinically significant concern, especially in critical care settings. With its robust arsenal of virulence factors and antibiotic resistance, S. marcescens challenges both clinicians and infection control teams. Vigilant monitoring, accurate diagnosis, targeted treatment, and stringent preventive measures are imperative to manage this formidable pathogen effectively.