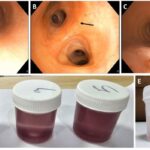
Nosocomial Pneumonia Due to Klebsiella pneumoniae: Klebsiella pneumoniae, a gram-negative, encapsulated bacillus, represents one of the most formidable pathogens implicated in nosocomial pneumonia. It is a leading cause of hospital-acquired pneumonia (HAP) and ventilator-associated pneumonia (VAP), particularly in critically ill and immunocompromised individuals. The organism’s ability to rapidly acquire multidrug resistance (MDR) and produce carbapenemases makes it a high-priority target for infection control and therapeutic strategies.
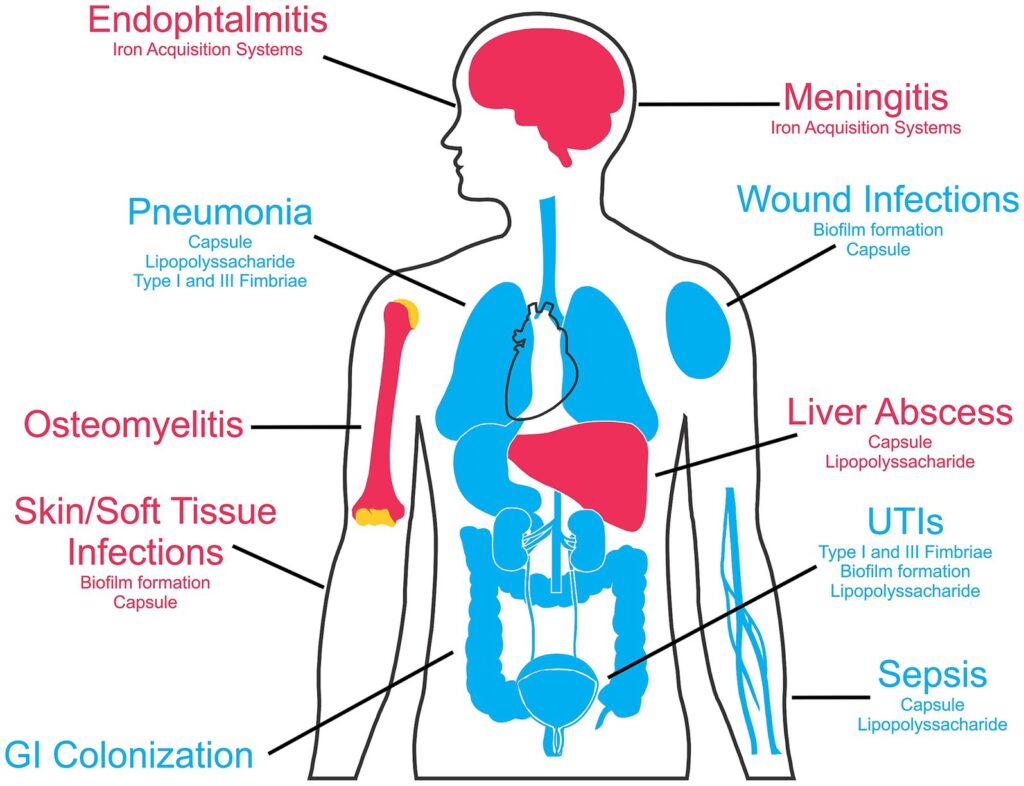
Microbiological Profile and Virulence Mechanisms
K. pneumoniae belongs to the Enterobacteriaceae family and is notorious for its polysaccharide capsule, which contributes to its mucoid phenotype and impairs phagocytosis. It produces a range of virulence factors that facilitate colonization, immune evasion, and tissue destruction.
Key Virulence Factors:
- Capsular Polysaccharide (CPS): Antiphagocytic and enhances biofilm formation
- Fimbriae (Type 1 and 3): Promote adhesion to respiratory epithelium
- Siderophores (e.g., enterobactin): Enhance iron acquisition in iron-depleted environments
- Lipopolysaccharide (LPS): Triggers strong inflammatory responses
- Hypermucoid phenotype regulator genes (rmpA, magA): Associated with hypervirulent strains
Pathogenesis and Transmission in Healthcare Settings
Nosocomial pneumonia caused by K. pneumoniae typically arises from microaspiration of colonized oropharyngeal secretions, hematogenous dissemination, or direct inoculation during mechanical ventilation. Its robust environmental survival and resistance to disinfectants make it a common colonizer in ICUs.
Epidemiology and At-Risk Populations
K. pneumoniae is responsible for approximately 10–20% of nosocomial pneumonia cases worldwide. Its prevalence is significantly higher in units with high antibiotic pressure and invasive interventions.
High-Risk Groups:
- Mechanically ventilated patients
- Individuals with diabetes mellitus or chronic lung disease
- Neutropenic or immunosuppressed patients
- Patients in long-term acute care or with prolonged hospital stay
- Prior antibiotic exposure, especially carbapenems or cephalosporins
Clinical Manifestations of K. pneumoniae Nosocomial Pneumonia
The presentation ranges from classic symptoms of HAP/VAP to fulminant pneumonia with necrotizing features, especially in hypervirulent strains.
Typical Symptoms:
- Fever and rigors
- Productive cough with blood-streaked or “currant jelly” sputum
- Dyspnea and hypoxia
- Chest pain and tachypnea
- New pulmonary infiltrates on imaging
Severe Presentations:
- Lung abscess formation
- Empyema
- Bacteremia and septic shock
- Acute respiratory distress syndrome (ARDS)
Diagnostic Strategy: Rapid Identification and Resistance Detection
Timely and accurate diagnosis is critical for appropriate treatment, particularly due to the rapid emergence of MDR strains.
Recommended Diagnostic Protocols:
1. Imaging Studies
- Chest X-ray: Baseline for infiltrates, lobar consolidation
- CT Scan: Detects cavitation, abscess, or complicated pneumonia
2. Microbiological Sampling
- Endotracheal aspirates, BAL fluid: Preferred in ventilated patients
- Sputum culture and Gram stain: Look for gram-negative bacilli with capsule
- Blood cultures: Mandatory in suspected bacteremia or septic presentation
3. Advanced Testing
- MALDI-TOF MS: Rapid bacterial identification
- PCR and multiplex assays: Detect carbapenemase genes (KPC, NDM, OXA-48)
- Antibiotic susceptibility testing: Guide therapy based on MIC values
Antimicrobial Resistance in Klebsiella pneumoniae
Resistance in K. pneumoniae is driven by multiple mechanisms, making empirical therapy challenging. Notable resistance phenotypes include:
Resistance Mechanisms:
- Extended-spectrum β-lactamases (ESBLs): Hydrolyze penicillins and cephalosporins
- Carbapenemases (KPC, NDM, OXA-48): Confer resistance to carbapenems
- Efflux pumps and porin loss: Reduce intracellular antibiotic concentration
- Plasmid-mediated resistance: Facilitates horizontal gene transfer
Resistance Profile Overview:
| Resistance Type | Mechanism | Impacted Antibiotics |
|---|---|---|
| ESBL-producing strains | Enzymatic degradation | Penicillins, 3rd-gen cephalosporins |
| Carbapenem-resistant | KPC, NDM, OXA-48 enzymes | Imipenem, meropenem |
| MDR/XDR strains | Combination resistance | Nearly all beta-lactams, fluoroquinolones |
Treatment of Nosocomial Pneumonia Due to Klebsiella pneumoniae
Management must be guided by severity of illness, local resistance patterns, and rapid susceptibility data.
Empiric Therapy (Pending Cultures):
- For ESBL producers: Meropenem or ertapenem
- For suspected CRKP (carbapenem-resistant K. pneumoniae):
- Ceftazidime-avibactam
- Meropenem-vaborbactam
- Cefiderocol (for extensively resistant strains)
- Combination therapy with colistin, tigecycline, aminoglycosides (as last resort)
Targeted Therapy:
- Adjust according to MICs and resistance genes
- De-escalation to narrow-spectrum agents is critical
- Duration: Typically 7–10 days; extend if complications arise
Adjunctive Support and ICU Considerations
Adjunctive measures are critical for favorable outcomes, especially in ventilator-associated cases.
ICU Management Includes:
- Adequate ventilator settings and lung-protective strategies
- Daily sedation vacations and early extubation attempts
- Monitoring of renal and hepatic function for drug dosing
- Nutritional support and glycemic control
- Infection source control (e.g., drainage of abscess/empyema)
Infection Control and Prevention of Transmission
Preventing the spread of K. pneumoniae, particularly carbapenem-resistant strains, is vital in healthcare environments.
Key Infection Control Measures:
- Contact precautions for colonized/infected patients
- Routine hand hygiene compliance audits
- Environmental disinfection of high-touch surfaces
- Screening of high-risk patients (rectal swabs for CRKP)
- Antibiotic stewardship to reduce unnecessary use of broad-spectrum agents
Clinical Outcomes and Complications
Nosocomial pneumonia caused by K. pneumoniae has higher morbidity and mortality compared to other gram-negatives, especially with MDR strains.
Common Complications:
- Septic shock
- Respiratory failure requiring prolonged ventilation
- Multiorgan dysfunction
- Prolonged ICU and hospital stays
Mortality Risk Factors:
- Delayed initiation of effective therapy
- Presence of CRKP or XDR strains
- Severe immunosuppression
- High APACHE II or SOFA scores on admission
Frequently Asked Questions:
What causes nosocomial pneumonia due to Klebsiella pneumoniae?
It results from hospital-based exposure and colonization of the respiratory tract, particularly in ventilated or immunocompromised patients.
How is K. pneumoniae pneumonia diagnosed?
Via respiratory cultures, imaging, blood cultures, and PCR tests for resistance genes.
Which antibiotics are effective against MDR Klebsiella pneumoniae?
Agents like ceftazidime-avibactam, meropenem-vaborbactam, and cefiderocol are used against resistant strains.
Is this infection contagious in hospitals?
Yes, CRKP can spread via contact and contaminated equipment, necessitating strict infection control.
Can nosocomial pneumonia from K. pneumoniae be prevented?
Yes, through ventilator bundles, strict hygiene, and antibiotic stewardship.
Nosocomial pneumonia due to Klebsiella pneumoniae remains a critical healthcare challenge due to its aggressive pathogenesis and multidrug resistance. Vigilant diagnostic practices, evidence-based antimicrobial therapy, and robust infection control protocols are essential to curbing its clinical impact. As the global burden of MDR and XDR K. pneumoniae increases, coordinated efforts in surveillance, stewardship, and research must be prioritized to ensure effective and sustainable management strategies.