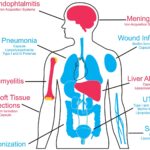
Nosocomial pneumonia due to Haemophilus influenzae (H. influenzae) is a significant concern in hospitalized patients, particularly among those in intensive care units (ICUs), on mechanical ventilation, or with pre-existing pulmonary conditions. As a facultative anaerobic, gram-negative coccobacillus, H. influenzae colonizes the upper respiratory tract and can transition to a pathogenic state under immunocompromised or hospital-acquired stressors.
While classically associated with community-acquired pneumonia, non-typeable H. influenzae (NTHi) is increasingly recognized in hospital-acquired pneumonia (HAP), particularly in elderly and debilitated populations.
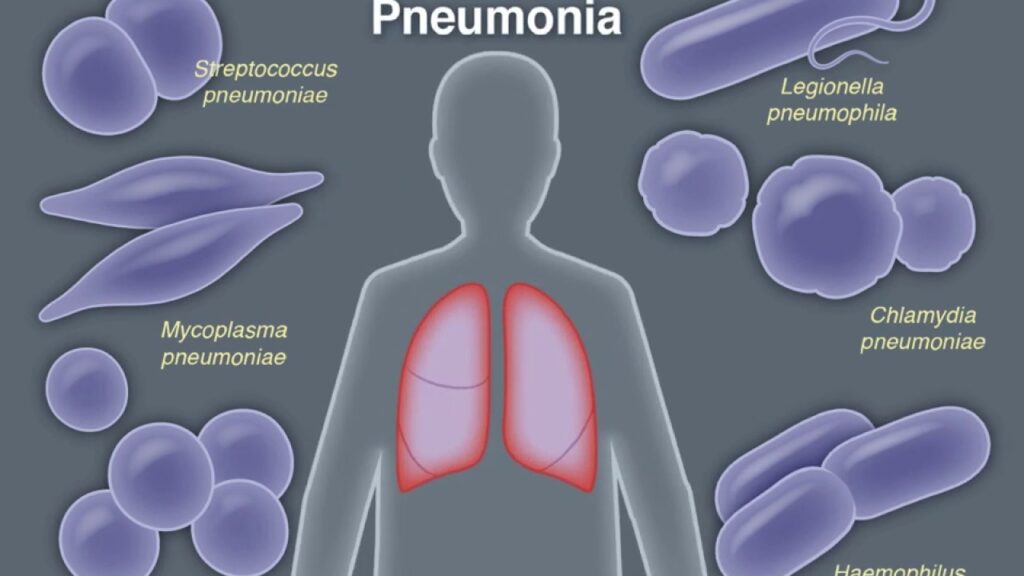
Microbiology and Classification
H. influenzae exists in encapsulated and non-encapsulated forms. Of the six capsular serotypes (a–f), type b (Hib) was historically the most virulent; however, widespread Hib vaccination has significantly reduced its prevalence. In the nosocomial setting, non-typeable strains, which lack a polysaccharide capsule, are more prevalent and adept at forming biofilms.
Virulence Factors:
- Fimbriae: Facilitate adherence to epithelial cells
- IgA protease: Degrades host immunoglobulin A
- Lipooligosaccharide (LOS): Induces strong inflammatory response
- Biofilm formation: Aids in persistence and antibiotic resistance
Pathogenesis of Hospital-Acquired Pneumonia from H. influenzae
Nosocomial pneumonia typically arises from microaspiration of colonized oropharyngeal secretions or through inhalation of contaminated aerosols. Invasive devices like endotracheal tubes further compromise airway defenses, allowing H. influenzae to infiltrate the lower respiratory tract.
Epidemiology and At-Risk Populations
H. influenzae is responsible for approximately 5–10% of nosocomial pneumonia cases globally. It disproportionately affects patients with chronic lung diseases, smokers, elderly individuals, and those with impaired immunity.
Key Risk Groups:
- ICU patients on mechanical ventilation (>48 hours)
- Individuals with COPD, bronchiectasis, or asthma
- Immunocompromised patients (e.g., cancer, transplant, HIV)
- Patients with prior antibiotic exposure or prolonged hospitalization
Clinical Features and Diagnostic Clues
Nosocomial pneumonia due to H. influenzae presents similarly to infections caused by other gram-negative organisms but may feature a more subacute onset, especially in ventilated patients.
Common Signs and Symptoms:
- Fever or hypothermia
- Increased sputum production (often mucopurulent)
- New or worsening infiltrates on chest radiograph
- Hypoxia or increased ventilator requirements
- Leukocytosis or leukopenia
- Elevated C-reactive protein and procalcitonin levels
Diagnostic Workflow for Accurate Identification
Prompt and precise diagnosis is vital to guiding antimicrobial therapy and limiting the spread of infection.
Diagnostic Tools and Tests
1. Radiological Evaluation
- Chest X-ray: Baseline imaging for detection of infiltrates or consolidation
- Chest CT: High-resolution imaging to identify complex or early disease patterns
2. Microbiological Sampling
- Sputum culture: Requires quality assessment for contamination
- Endotracheal aspirate or BAL fluid: Standard in ventilated patients
- Blood cultures: Especially in febrile or hypotensive cases
3. Molecular and Immunological Techniques
- PCR-based assays for rapid identification of H. influenzae DNA
- ELISA for detection of capsular antigens (rarely used due to NTHi predominance)
Antimicrobial Susceptibility and Resistance Mechanisms
H. influenzae has demonstrated increasing resistance to traditional antibiotics, particularly beta-lactams. The resistance mechanisms include:
- Beta-lactamase production (TEM-1 and ROB-1 types)
- Altered penicillin-binding proteins (β-lactamase-negative ampicillin-resistant, or BLNAR strains)
Antibiotic Resistance Overview:
| Resistance Type | Mechanism | Impacted Drugs |
|---|---|---|
| Beta-lactamase producers | Enzymatic degradation of beta-lactams | Ampicillin, amoxicillin |
| BLNAR strains | Altered PBP3 enzyme | Cephalosporins, some penicillins |
| Biofilm-related resistance | Reduced penetration and efflux pumps | Multiple antibiotic classes |
Evidence-Based Management and Antibiotic Therapy
Therapeutic regimens should be tailored based on local antibiogram data and the patient’s risk factors for multidrug-resistant organisms.
Empiric Therapy Options:
- Amoxicillin-clavulanate
- Ceftriaxone or cefotaxime
- Respiratory fluoroquinolones (e.g., levofloxacin, moxifloxacin)
- Cefepime or piperacillin-tazobactam (in severe or polymicrobial cases)
Targeted Therapy:
- Adjusted per culture sensitivity
- Discontinue broad-spectrum agents after de-escalation
- Treatment duration: 7–10 days for uncomplicated HAP; extended in immunocompromised hosts or non-responders
Adjunctive Supportive Measures in Management
Optimal clinical outcomes require more than antibiotic therapy. Supportive strategies are integral, particularly in ICU patients.
Supportive Care Components:
- Adequate oxygenation and ventilation
- Chest physiotherapy and airway clearance techniques
- Fluid and electrolyte management
- Nutritional support in prolonged ICU stays
- Early mobilization when feasible
Prevention of Nosocomial H. influenzae Pneumonia
Reducing the incidence of nosocomial pneumonia due to H. influenzae involves multi-faceted infection control and hospital hygiene protocols.
Key Prevention Strategies:
- Hand hygiene and personal protective equipment
- Decontamination and maintenance of ventilator circuits
- Elevation of the head of the bed in ventilated patients
- Daily sedation interruption and assessment for extubation
- Antimicrobial stewardship to prevent resistance selection
Complications and Prognostic Indicators
Complications are more likely in elderly patients or those with underlying chronic disease. Mortality rates remain significant, especially in polymicrobial infections.
Common Complications:
- Empyema or parapneumonic effusion
- Respiratory failure requiring prolonged ventilation
- Secondary bacteremia and sepsis
- Persistent colonization and relapse
Poor Prognostic Indicators:
- Delayed initiation of effective antibiotics
- Presence of MDR or BLNAR strains
- Co-existing respiratory comorbidities
- Organ dysfunction or septic shock
Frequently Asked Questions:
What is nosocomial pneumonia due to Haemophilus influenzae?
It is a lung infection acquired in hospital settings, caused by H. influenzae, primarily affecting critically ill or ventilated patients.
How is H. influenzae pneumonia diagnosed?
Diagnosis involves imaging, microbiological cultures from lower respiratory tract samples, and sometimes molecular PCR testing.
Which antibiotics are used for treatment?
Beta-lactam/beta-lactamase inhibitors, cephalosporins, and fluoroquinolones are commonly effective, depending on local resistance profiles.
Is Haemophilus influenzae contagious in hospitals?
Yes, particularly non-typeable strains can spread via droplets and contaminated surfaces without proper infection control.
Can H. influenzae pneumonia be prevented?
Yes, through ventilator care bundles, strict hygiene practices, and prudent use of antibiotics in healthcare settings.
Nosocomial pneumonia due to Haemophilus influenzae is a clinically significant and potentially preventable infection. With increasing recognition of its role in hospital-acquired respiratory infections, especially among high-risk individuals, a structured approach involving early diagnosis, targeted antimicrobial therapy, and robust prevention strategies is essential. Vigilance in antimicrobial stewardship and infection control remains paramount in curbing its impact on healthcare systems.