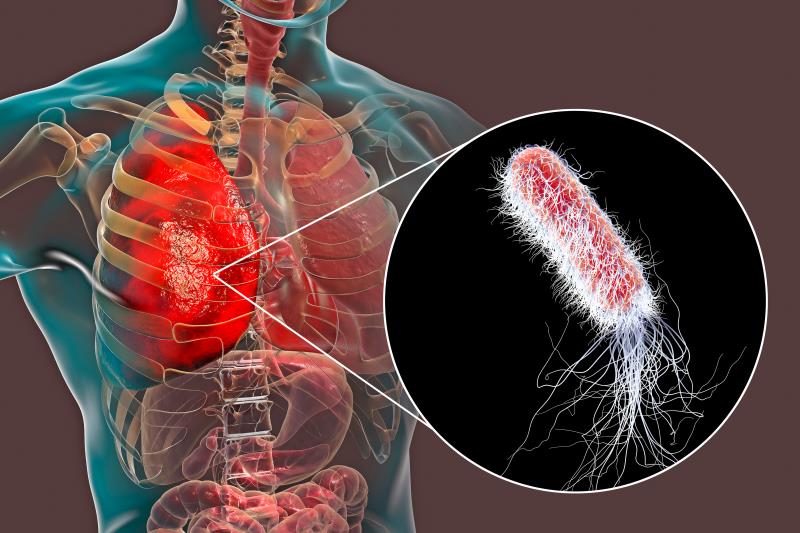
Nosocomial Pneumonia Due to Escherichia coli: Nosocomial pneumonia due to Escherichia coli represents a significant burden in hospital settings, particularly among critically ill and immunocompromised patients. As a gram-negative bacillus from the Enterobacteriaceae family, E. coli has emerged as a notable pathogen in hospital-acquired pneumonia (HAP), especially among those undergoing invasive procedures or prolonged antibiotic exposure.
Epidemiology and Incidence in Healthcare Settings
The frequency of E. coli as a causative agent in nosocomial pneumonia has increased in correlation with the rise in multidrug-resistant (MDR) strains. It is more prevalent in intensive care units (ICUs), especially in ventilator-associated pneumonia (VAP), where colonization and infection rates are elevated due to device use and host vulnerability.
Key Statistics:
- E. coli accounts for 6–12% of nosocomial pneumonia cases.
- ESBL-producing E. coli strains are responsible for over 40% of ICU-related infections in some regions.
- Mortality from E. coli-associated VAP ranges between 25–45%, especially in septic and immunocompromised patients.
Pathophysiology and Mechanism of Infection
Nosocomial pneumonia due to E. coli typically develops via microaspiration of oropharyngeal secretions or through contamination of respiratory equipment. Once colonization occurs, the pathogen overcomes host defenses, leading to infection of the lower respiratory tract.
Virulence factors of E. coli contributing to lung infection include:
- Fimbriae: Facilitate adhesion to epithelial cells
- Lipopolysaccharide (LPS): Triggers inflammatory response
- Capsular polysaccharide: Inhibits phagocytosis
- Siderophores: Iron acquisition mechanisms critical for bacterial growth
Risk Factors for E. coli Pneumonia in Hospitalized Patients
Multiple patient-related and treatment-related risk factors contribute to susceptibility.
Major Risk Factors
- Mechanical ventilation (>48 hours)
- Advanced age (>65 years)
- Diabetes mellitus
- Chronic kidney or liver disease
- Immunosuppressive therapy
- Prior use of broad-spectrum antibiotics
- Recent surgical interventions
- Prolonged hospitalization or ICU stay
Clinical Manifestations of E. coli-Associated Nosocomial Pneumonia
Patients with E. coli-driven nosocomial pneumonia present with a constellation of respiratory and systemic symptoms, often indistinguishable from pneumonia caused by other gram-negative organisms.
Key Clinical Features:
- Sudden or progressive onset of fever (>38°C)
- Dyspnea, tachypnea, or respiratory distress
- Productive cough with purulent sputum
- Hypoxemia or rising oxygen requirement
- New or worsening pulmonary infiltrates on imaging
- Leukocytosis or leukopenia
- Sepsis or septic shock in severe cases
Diagnostic Criteria and Investigations
Prompt identification is essential for targeted therapy and improved outcomes.
Diagnostic Approach
1. Radiological Imaging
- Chest X-ray: Detects lobar or multilobar infiltrates
- Chest CT: Offers higher sensitivity in identifying early or atypical presentations
2. Microbiological Cultures
- Endotracheal aspirate (ETA)
- Bronchoalveolar lavage (BAL)
- Blood cultures in febrile or hypotensive patients
- Quantitative cultures preferred over qualitative for specificity
3. Biochemical Markers
- Procalcitonin (PCT) levels: Assist in identifying bacterial etiology
- C-reactive protein (CRP): Supports infection monitoring
4. Molecular Testing
- PCR assays for rapid detection of resistance genes (e.g., ESBL, carbapenemases)
- Next-generation sequencing in research or high-resource settings
Antimicrobial Resistance Patterns
Antibiotic resistance in E. coli is a growing concern, with significant clinical implications.
Resistance Mechanisms:
- Extended-spectrum beta-lactamases (ESBLs): Inactivate cephalosporins and penicillins
- Carbapenemases (e.g., NDM, KPC): Confer resistance to carbapenems
- Efflux pumps and porin mutations: Reduce antibiotic penetration
Multidrug-Resistant E. coli Phenotypes
| Resistance Profile | Commonly Resistant To |
|---|---|
| ESBL-producing E. coli | Cephalosporins, penicillins, aztreonam |
| Carbapenem-resistant strains | Carbapenems, aminoglycosides, fluoroquinolones |
| MDR/XDR E. coli | Resistance to ≥3 drug classes |
Treatment and Management of Nosocomial E. coli Pneumonia
Treatment hinges on timely initiation of empiric antibiotics, followed by de-escalation based on culture results and susceptibility profiles.
Empiric Therapy (Pending Cultures)
- Piperacillin-tazobactam
- Meropenem or imipenem-cilastatin (in critically ill or resistant cases)
- Cefepime or ceftazidime
- Consider adding colistin or tigecycline in settings with high carbapenem resistance
Targeted Therapy (Post-Susceptibility Results)
- Ceftriaxone or cefotaxime (for sensitive strains)
- Carbapenems (for ESBL-producing strains)
- Ceftazidime-avibactam or meropenem-vaborbactam (for CRE infections)
- Duration: Typically 7–8 days for uncomplicated cases; up to 14 days for VAP with complications
Adjunctive Measures
- Supportive oxygen therapy or ventilation
- Fluid resuscitation and vasopressors if septic shock present
- Removal or replacement of contaminated equipment (e.g., endotracheal tubes)
Infection Control and Prevention Strategies
Preventing nosocomial pneumonia, particularly due to MDR E. coli, requires stringent infection control protocols.
Hospital Measures
- Strict hand hygiene and contact precautions
- Isolation of colonized or infected patients
- Routine disinfection of ventilators and respiratory devices
- Daily assessment for readiness to wean off ventilators
Antimicrobial Stewardship
- Avoid unnecessary use of broad-spectrum antibiotics
- Regular antibiogram surveillance
- De-escalation protocols based on culture and sensitivity
Complications and Prognosis
Delayed or inadequate treatment of E. coli-related nosocomial pneumonia can lead to serious outcomes.
Potential Complications:
- Acute respiratory distress syndrome (ARDS)
- Empyema or pleural effusion
- Sepsis and multiorgan failure
- Persistent bacteremia
- Increased length of ICU stay
- High mortality in resistant infections
Prognosis depends on host factors, early detection, pathogen susceptibility, and timely initiation of appropriate therapy.
Frequently Asked Questions
What is nosocomial pneumonia due to E. coli?
It is a hospital-acquired lung infection caused by Escherichia coli, often linked to prolonged hospitalization or mechanical ventilation.
How is E. coli pneumonia diagnosed?
Through clinical assessment, imaging studies, and microbiological cultures from lower respiratory tract samples.
What antibiotics are effective against E. coli pneumonia?
Therapy is guided by local antibiograms, typically involving cephalosporins, carbapenems, or newer beta-lactamase inhibitors depending on resistance.
Is E. coli pneumonia contagious in hospitals?
Yes, especially MDR strains, through contaminated surfaces, devices, or hands of healthcare workers.
How can hospitals prevent this infection?
By maintaining hygiene standards, ventilator care bundles, isolating infected patients, and antimicrobial stewardship.
Nosocomial pneumonia due to Escherichia coli is a formidable clinical entity, particularly with rising multidrug resistance. Comprehensive risk stratification, early and accurate diagnosis, guided antimicrobial therapy, and robust infection prevention practices are indispensable in mitigating its burden. With advancements in diagnostics and evolving antimicrobial options, outcomes can improve—provided protocols are rigorously followed across all levels of care.