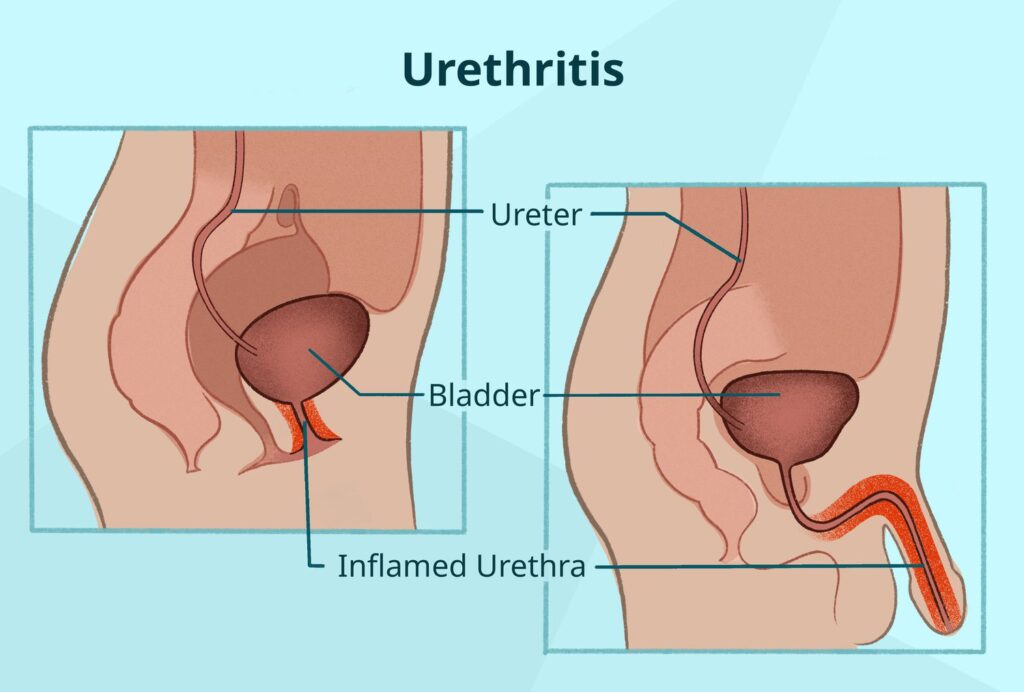
Nongonococcal urethritis (NGU) refers to inflammation of the urethra not caused by Neisseria gonorrhoeae. It is a common urogenital condition, especially in sexually active males, and represents a significant proportion of urethritis cases globally. NGU is primarily transmitted through sexual contact and is commonly caused by bacterial pathogens, particularly Chlamydia trachomatis, though other organisms and noninfectious factors may be involved.
Etiology: Primary Causes of Nongonococcal Urethritis
The majority of NGU cases are infectious, yet up to 40% may have unknown etiology. The most recognized pathogens include:
1. Chlamydia trachomatis
- Most prevalent cause (20–50% of NGU cases)
- An intracellular bacterium, often asymptomatic but highly transmissible
2. Mycoplasma genitalium
- Emerging significant pathogen, especially in persistent or recurrent cases
- Demonstrates resistance to first-line antibiotics
3. Ureaplasma urealyticum
- Frequently isolated; its pathogenicity is debated
- More common in asymptomatic infections
4. Trichomonas vaginalis
- Flagellated protozoan, primarily seen in men who have sex with women from endemic regions
5. Herpes Simplex Virus (HSV)
- Causes ulceration and inflammation of the urethra
- NGU associated with painful lesions
6. Adenovirus and other enteric organisms
- Occasionally implicated in cases with oral-genital contact
Transmission Pathways and Risk Factors
Sexual and Non-Sexual Routes
NGU is primarily a sexually transmitted infection (STI). It can also rarely result from:
- Poor hygiene practices
- Catheterization or instrumentation
- Chemical irritants (e.g., soaps, spermicides)
Risk Factors
- Multiple sexual partners
- Inconsistent or no condom use
- Recent change in sexual partner
- History of previous STIs
- Engaging in unprotected oral or anal sex
Clinical Presentation and Common Symptoms
Patients with NGU may be asymptomatic or present with the following:
| Symptom | Prevalence |
|---|---|
| Urethral discharge (mucoid or clear) | Very common |
| Dysuria (painful urination) | Common |
| Urethral irritation or itching | Common |
| Penile discomfort or burning | Frequent |
| Testicular or scrotal pain (rare) | Occasional |
Symptoms typically develop within 1–3 weeks after exposure.
Diagnostic Approach to NGU
Clinical Evaluation
Initial assessment should include:
- Detailed sexual history
- Physical examination focusing on genital inspection
- Evaluation for other STIs, including gonorrhea, HIV, and syphilis
Laboratory Testing
1. Microscopy
- Urethral swab showing ≥5 polymorphonuclear leukocytes (PMNs)/HPF
- Gram stain to rule out N. gonorrhoeae
2. Nucleic Acid Amplification Tests (NAATs)
- Gold standard for detecting Chlamydia trachomatis and Mycoplasma genitalium
- Can be performed on first-catch urine or urethral swabs
3. Culture or PCR for HSV/Trichomonas
- In atypical or persistent cases
Treatment and Management of Nongonococcal Urethritis
First-Line Antibiotic Therapy
| Pathogen | Recommended Regimen |
|---|---|
| Chlamydia trachomatis | Doxycycline 100 mg orally twice daily for 7 days |
| Mycoplasma genitalium | Moxifloxacin 400 mg daily for 7–14 days |
| Unknown/Empiric | Doxycycline preferred; Azithromycin if compliance is a concern |
Note: Due to rising resistance, azithromycin monotherapy is no longer universally recommended.
Persistent or Recurrent NGU
- Confirm patient adherence
- Exclude reinfection from untreated partner
- Test for Mycoplasma genitalium
- Consider alternative diagnoses such as HSV, adenovirus, or noninfectious causes
Complications and Sequelae of Untreated NGU
If left untreated, NGU can result in several adverse outcomes:
- Epididymitis
- Prostatitis
- Reactive arthritis (Reiter’s syndrome)
- Infertility (due to ascending infection)
- Transmission to partners — particularly significant for Chlamydia, which can cause pelvic inflammatory disease (PID) in women
NGU in Women: A Silent Condition
While the term “nongonococcal urethritis” is used primarily for males, females can harbor the same pathogens with different manifestations:
- Cervicitis
- Vaginal discharge
- Intermenstrual bleeding
- Pelvic pain
Often asymptomatic, routine screening of sexual partners is essential for control.
Prevention and Public Health Measures
Safer Sex Practices
- Consistent condom use
- Mutual monogamy with an uninfected partner
- Avoidance of high-risk sexual behavior
Partner Notification and Treatment
- All sexual partners within the past 60 days must be notified, tested, and treated
- Abstain from sexual contact until 7 days after treatment completion
Follow-Up
- Routine test-of-cure not required for Chlamydia unless using azithromycin or patient is pregnant
- Re-testing in 3 months recommended to detect reinfection
Frequently Asked Questions:
What is nongonococcal urethritis?
Nongonococcal urethritis is inflammation of the urethra not caused by Neisseria gonorrhoeae, typically due to Chlamydia or other pathogens.
Is NGU sexually transmitted?
Yes, the majority of NGU cases are sexually transmitted through vaginal, oral, or anal sex.
Can NGU be asymptomatic?
Yes, especially in early stages or in female carriers, NGU can be completely silent.
What is the best treatment for NGU?
Doxycycline is currently the preferred first-line antibiotic due to its high efficacy and low resistance profile.
Can NGU come back after treatment?
Yes, reinfection from an untreated partner or antibiotic resistance can lead to recurrence.
Nongonococcal urethritis is a prevalent and clinically important condition requiring prompt diagnosis, targeted treatment, and partner management. With growing antimicrobial resistance, especially in Mycoplasma genitalium, accurate diagnosis and compliance with treatment guidelines are essential to prevent complications and transmission. Continued public health awareness and adherence to preventive strategies remain key in reducing NGU incidence worldwide.