Nonfunctional Neuroendocrine Tumors of Lung Origin: Nonfunctional neuroendocrine tumors (NETs) of lung origin represent a subset of bronchopulmonary neuroendocrine neoplasms characterized by neuroendocrine differentiation without active hormone secretion. These tumors primarily arise from Kulchitsky cells in the bronchial mucosa and do not cause endocrine-related symptoms, such as those seen in functional NETs.
They are often diagnosed incidentally during imaging for unrelated pulmonary complaints. Despite their non-secretory nature, these tumors can be locally aggressive or metastatic, necessitating a careful and strategic clinical approach.
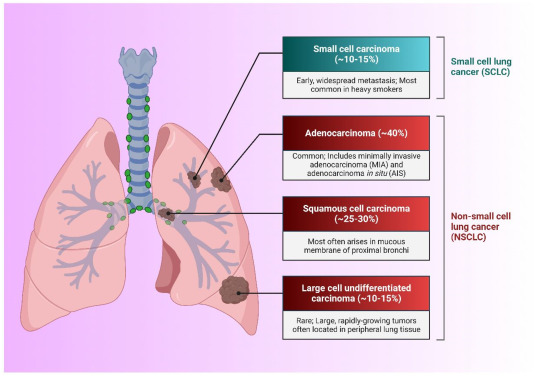
Classification of Pulmonary NETs Based on Differentiation
Lung NETs are histologically divided into four major types according to the World Health Organization (WHO) classification:
| Type | Grade | Mitotic Rate (per 2mm²) | Necrosis |
|---|---|---|---|
| Typical Carcinoid (TC) | Low | <2 | Absent |
| Atypical Carcinoid (AC) | Intermediate | 2–10 | Focal |
| Large Cell Neuroendocrine Carcinoma (LCNEC) | High | >10 | Prominent |
| Small Cell Lung Carcinoma (SCLC) | High | >10 | Prominent |
Nonfunctional NETs can occur across all four categories but are most commonly observed in typical and atypical carcinoids.
Pathogenesis and Molecular Mechanisms
Pulmonary NETs arise from pulmonary neuroendocrine cells (PNECs) located in the bronchial epithelium. Genetic mutations, epigenetic changes, and signaling pathway alterations lead to neoplastic transformation.
Clinical Presentation and Detection
Since nonfunctional NETs do not secrete active hormones, symptoms are due to tumor size, location, and metastasis, including:
- Persistent cough
- Wheezing
- Hemoptysis
- Chest discomfort
- Recurrent pneumonia
- Asymptomatic (incidentally detected on chest imaging)
Diagnostic Evaluation of Nonfunctional Lung NETs
1. Radiologic Imaging
- Chest CT with contrast: Initial imaging modality for tumor localization
- PET/CT with 68Ga-DOTATATE: Preferred for well-differentiated NETs; assesses somatostatin receptor expression
- FDG-PET/CT: Useful in high-grade or poorly differentiated tumors
2. Bronchoscopy and Biopsy
- Allows direct visualization and tissue sampling
- Endobronchial ultrasound (EBUS) assists in evaluating nodal involvement
3. Histological and Immunohistochemical Analysis
- Key markers: Chromogranin A, Synaptophysin, CD56
- Ki-67 index helps grade tumor proliferation and guide treatment
Tumor Staging and Metastasis Patterns
Pulmonary NETs are staged using the TNM classification (8th Edition, AJCC):
- T – Tumor size and invasion
- N – Nodal involvement (mediastinal, hilar)
- M – Metastasis (liver, bone, adrenal glands)
Common metastatic sites include liver, brain, bone, and adrenal glands, especially in atypical carcinoids and high-grade NECs.
Treatment Strategies for Nonfunctional Pulmonary NETs
1. Surgical Resection
- First-line treatment for localized tumors
- Options include lobectomy, segmentectomy, and wedge resection, often with mediastinal lymph node dissection
2. Medical Therapy
- Somatostatin analogs (Octreotide, Lanreotide): Used in metastatic or progressive disease to control tumor growth
- Targeted therapies:
- Everolimus (mTOR inhibitor) for progressive lung NETs
- Peptide Receptor Radionuclide Therapy (PRRT) with Lu-177 DOTATATE in advanced cases
- Chemotherapy:
- Reserved for high-grade tumors (LCNEC, SCLC)
- Regimens include platinum-based agents (cisplatin, carboplatin + etoposide)
3. Radiation Therapy
- Indicated for inoperable tumors, palliation, or brain metastases
Prognostic Indicators and Survival Rates
Prognosis depends heavily on tumor grade, stage, and presence of metastasis:
| Tumor Type | 5-Year Survival Rate |
|---|---|
| Typical Carcinoid | 85–95% |
| Atypical Carcinoid | 50–70% |
| LCNEC | 15–25% |
| SCLC | <10% |
Early-stage typical carcinoids have excellent outcomes, while high-grade NECs portend poor survival even with aggressive treatment.
Distinction Between Functional and Nonfunctional Lung NETs
| Feature | Functional NET | Nonfunctional NET |
|---|---|---|
| Hormone Production | Yes (e.g., ACTH, serotonin) | No |
| Paraneoplastic Syndromes | Common (Cushing’s, carcinoid syndrome) | Absent |
| Diagnosis Triggered By | Hormonal symptoms | Imaging or incidental findings |
| Biomarker Elevation | High serotonin, ACTH, urinary 5-HIAA | Usually normal |
Evolving Research and Future Directions
Biomarkers and Liquid Biopsy
Emerging circulating tumor cells (CTCs) and NET-specific gene expression assays (e.g., NETest) may allow earlier diagnosis and dynamic monitoring.
Immunotherapy
- Under evaluation for high-grade pulmonary NETs
- Immune checkpoint inhibitors show potential benefit in PD-L1-positive LCNEC and SCLC subtypes
Genomic and Molecular Targeting
- Use of next-generation sequencing (NGS) to identify actionable mutations
- Studies underway on DLL3, BCL-2, and RET inhibitors
Frequently Asked Questions on Nonfunctional Neuroendocrine Tumors of Lung Origin
What is a nonfunctional lung neuroendocrine tumor?
It is a tumor in the lungs arising from neuroendocrine cells that does not produce hormones in clinically significant amounts.
Are nonfunctional lung NETs cancerous?
Yes, they are neoplastic and can be benign or malignant depending on the grade and stage.
Can nonfunctional lung NETs metastasize?
Yes. Atypical carcinoids and high-grade NECs have a significant risk of metastasis, particularly to the liver and brain.
What is the most effective treatment?
Surgical resection is the mainstay for localized tumors. For advanced cases, multimodal therapy including PRRT and targeted therapy may be employed.
Is long-term follow-up necessary?
Yes. Recurrence or late metastasis can occur, especially with atypical carcinoids. Lifelong surveillance with imaging and biomarkers is recommended.
Nonfunctional neuroendocrine tumors of lung origin, though clinically silent, demand a multidisciplinary and nuanced management approach. Advances in imaging, histopathology, and targeted therapeutics continue to reshape diagnostic and therapeutic strategies. Accurate grading, thorough staging, and individualized treatment are essential to optimizing patient outcomes in this heterogeneous tumor group.