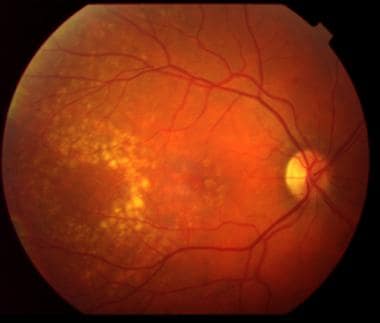
Nonexudative age-related macular degeneration (AMD), commonly referred to as dry AMD, is a chronic, progressive retinal disorder that affects the macula, the central portion of the retina responsible for sharp, detailed vision. It is the most prevalent form of AMD, accounting for approximately 85–90% of all AMD cases, especially in populations aged over 60. Unlike the exudative or “wet” form, dry AMD progresses gradually without the presence of abnormal blood vessel growth or fluid leakage.
Pathophysiology of Nonexudative AMD
Dry AMD begins with the accumulation of drusen, which are lipid-rich extracellular deposits that form between the retinal pigment epithelium (RPE) and Bruch’s membrane. Over time, these deposits can lead to RPE dysfunction, photoreceptor death, and ultimately, geographic atrophy (GA) — an advanced stage of dry AMD marked by irreversible vision loss.
Key Risk Factors for Nonexudative AMD
- Age: Incidence sharply increases after age 60
- Genetics: Variants in genes such as CFH, ARMS2, and HTRA1
- Smoking: Strongly associated with higher risk and faster progression
- Diet: Low intake of antioxidants and omega-3 fatty acids
- UV Exposure: May contribute to retinal oxidative stress
- Cardiovascular health: Hypertension, high cholesterol, and obesity are contributory
Stages of Nonexudative AMD
1. Early Dry AMD
- Clinical Signs: Small to medium-sized drusen, minimal pigment changes
- Symptoms: Usually asymptomatic
- Diagnosis: Detected through routine retinal exams and OCT
2. Intermediate Dry AMD
- Clinical Signs: Large drusen (>125 microns), more pronounced pigmentary changes
- Symptoms: Blurred or distorted central vision under dim lighting
- Diagnosis: Fundus photography, fluorescein angiography, OCT imaging
3. Advanced Dry AMD (Geographic Atrophy)
- Clinical Signs: RPE and photoreceptor atrophy, visible areas of retinal thinning
- Symptoms: Central scotoma, difficulty reading or recognizing faces
- Impact: Permanent central vision loss; peripheral vision remains intact
Symptoms of Nonexudative AMD
- Gradual loss of central vision
- Blurriness when reading or driving
- Distorted vision (metamorphopsia)
- Difficulty in low light or adjusting to darkness
- Faded colors
- Trouble recognizing faces at a distance
Diagnostic Techniques for Dry AMD
Optical Coherence Tomography (OCT)
Provides high-resolution cross-sectional imaging of retinal layers to identify drusen, thinning of RPE, and areas of geographic atrophy.
Fundus Autofluorescence (FAF)
Detects lipofuscin accumulation and helps visualize early signs of retinal stress or degeneration.
Fluorescein Angiography (FA)
Used primarily to rule out wet AMD by visualizing blood vessels and leakage patterns.
Visual Acuity and Amsler Grid Testing
Helps monitor functional vision and detect progression.
Progression from Dry to Wet AMD
Although dry AMD progresses slowly, approximately 10–15% of patients with intermediate or advanced dry AMD will convert to the exudative form, characterized by neovascularization. Timely monitoring is essential to detect this transition, as anti-VEGF therapies can limit vision loss in wet AMD.
Current Management Strategies for Nonexudative AMD
1. Lifestyle and Nutritional Interventions
- AREDS2 formula supplements: Vitamins C and E, lutein, zeaxanthin, zinc, and copper
- Diet rich in leafy greens, fish, and antioxidants
- Smoking cessation
- UV-protective eyewear
- Blood pressure and cholesterol control
2. Low Vision Aids
Patients with geographic atrophy may benefit from:
- Magnifiers
- Electronic reading devices
- Specialized lighting
- Vision rehabilitation programs
3. Monitoring and Follow-Up
- Routine OCT and fundus exams
- Amsler Grid self-monitoring
- Annual or semi-annual visits for intermediate AMD cases
Emerging Treatments and Clinical Trials
While there is no FDA-approved treatment for early or intermediate dry AMD, several promising approaches are in development:
Complement Inhibition
- Pegcetacoplan (Empaveli) – targets C3 in the complement pathway; Phase 3 trials show reduced progression of geographic atrophy
- Avacincaptad pegol (Zimura) – C5 inhibitor showing similar effects
Neuroprotection
- Brimonidine implants and CNTF-based therapies are being evaluated to protect retinal cells from degeneration.
Stem Cell Therapies
- Research underway on RPE cell transplantation using embryonic or induced pluripotent stem cells.
Gene Therapy
- Investigational vectors aim to deliver complement-regulating genes to the retina to halt progression.
Preventive Strategies for At-Risk Populations
- Routine eye exams after age 50
- Genetic counseling for those with family history
- Healthy diet, regular exercise, and smoking avoidance
- Using digital screens responsibly to reduce eye strain
- Managing comorbid conditions like diabetes and hypertension
Prognosis of Nonexudative AMD
- Early-stage dry AMD may remain stable for years without vision loss
- Intermediate AMD progresses slowly, often over decades
- Geographic atrophy leads to permanent central vision loss but typically spares peripheral vision
- Early detection and adherence to lifestyle modifications greatly improve long-term outcomes
Frequently Asked Questions:
What is nonexudative AMD?
Nonexudative AMD, or dry age-related macular degeneration, is a retinal condition involving drusen accumulation and gradual vision loss without abnormal blood vessel growth.
How is dry AMD diagnosed?
It is diagnosed via retinal imaging techniques such as OCT, fundus photography, and autofluorescence, often during routine eye exams.
Can dry AMD lead to complete blindness?
Dry AMD causes central vision loss, but peripheral vision is usually preserved, so complete blindness is rare.
Is there a cure for nonexudative AMD?
There is no cure, but progression can be slowed with nutritional supplements, healthy lifestyle changes, and close monitoring.
How often should patients with dry AMD see an eye specialist?
Patients should have at least annual follow-ups, with more frequent visits if symptoms worsen or if they have intermediate-stage AMD.
Nonexudative age-related macular degeneration remains a significant cause of visual impairment among the elderly. Understanding its etiology, identifying early signs, and implementing timely management strategies are essential to preserving vision and quality of life. With advances in retinal imaging and ongoing clinical trials, the future holds promise for patients with this progressive condition.