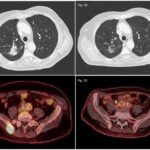
Non-small cell lung cancer (NSCLC) encompasses a heterogeneous group of malignancies that together represent approximately 85% of all lung cancers. Among these, EGFR exon 19 deletion mutations account for nearly 45% of all EGFR mutations and are particularly significant due to their strong sensitivity to EGFR tyrosine kinase inhibitors (TKIs). These mutations result in aberrant signaling in the epidermal growth factor receptor (EGFR) pathway, driving tumorigenesis in a subset of patients.
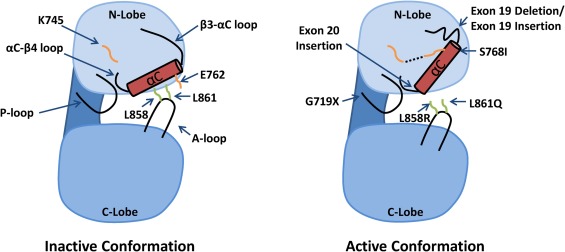
Molecular Pathogenesis of EGFR Exon 19 Deletion
EGFR is a transmembrane tyrosine kinase receptor that regulates cell proliferation and survival. Exon 19 deletions typically remove amino acids 746–750 within the tyrosine kinase domain, leading to constitutive activation of EGFR and downstream signaling pathways, especially the PI3K/AKT and RAS/RAF/MEK/ERK cascades.
This gain-of-function mutation renders the tumor cells highly dependent on EGFR signaling, making them susceptible to inhibition by targeted agents.
Epidemiology and Patient Demographics
- Incidence: EGFR mutations are found in 10–15% of NSCLC patients in Western populations and up to 50% in East Asian populations.
- EGFR exon 19 deletion is the most frequent subtype, more common than the L858R point mutation.
- Demographics:
- More prevalent in non-smokers
- More common in females
- Predominantly seen in adenocarcinoma histology
Diagnostic Strategies for EGFR Exon 19 Deletion
Tissue-Based Molecular Testing
- Biopsy and histopathologic confirmation
- Next-generation sequencing (NGS) panels or real-time PCR
- Digital droplet PCR (ddPCR) for high sensitivity
Liquid Biopsy (ctDNA)
- Detects EGFR mutations in circulating tumor DNA
- Useful when tissue biopsy is infeasible
- Also employed to track resistance mutations such as T790M
Routine molecular profiling is essential for all advanced NSCLC cases, and EGFR mutation testing is standard-of-care in initial workups.
Targeted Therapy Options for EGFR Exon 19 Deletion
First-Line Treatment: Osimertinib
Osimertinib is a third-generation EGFR-TKI that irreversibly inhibits both sensitizing mutations (exon 19 deletion and L858R) and the resistance mutation T790M.
FLAURA Trial Outcomes
- Progression-Free Survival (PFS): 18.9 months (vs. 10.2 months with 1st-gen TKIs)
- Overall Survival (OS): 38.6 months
- CNS Penetration: Effective against brain metastases
Comparison of EGFR-TKIs
| Drug | Generation | PFS (months) | CNS Activity | T790M Activity |
|---|---|---|---|---|
| Gefitinib | 1st | ~10 | Limited | No |
| Erlotinib | 1st | ~10 | Limited | No |
| Afatinib | 2nd | ~11 | Moderate | No |
| Dacomitinib | 2nd | ~14.7 | Moderate | No |
| Osimertinib | 3rd | 18.9 | High | Yes |
Osimertinib is now considered standard first-line therapy for patients with EGFR exon 19 deletion.
Treatment Resistance in EGFR Exon 19 NSCLC
Despite initial responses, resistance to EGFR-TKIs is inevitable.
Mechanisms of Resistance
- EGFR T790M mutation (common after 1st/2nd-gen TKIs)
- MET amplification
- HER2 amplification
- Small cell transformation
- KRAS mutations
- Histologic evolution
Strategies to Overcome Resistance
- Re-biopsy to identify resistance mechanism
- Osimertinib if resistance is due to T790M
- MET inhibitors or combination regimens if MET amplification is present
- Chemotherapy or immunotherapy in cases without targetable mutations
Role of Chemotherapy and Immunotherapy
Chemotherapy
Still plays a role:
- For patients without targetable resistance mutations
- As salvage therapy post-TKI progression
Standard regimens: Platinum-doublet chemotherapy ± bevacizumab
Immunotherapy
Generally less effective in EGFR-mutated NSCLC due to:
- Lower tumor mutational burden (TMB)
- Lower PD-L1 expression
- Immunologically “cold” tumor microenvironment
However, immunotherapy may be combined with chemotherapy in selected cases or used in later lines.
Surveillance and Monitoring
Initial Staging
- CT chest and abdomen
- Brain MRI for asymptomatic CNS involvement
- PET-CT for distant metastases
Monitoring During Therapy
- Imaging every 8–12 weeks
- ctDNA for early detection of resistance
- Periodic brain imaging, particularly with CNS involvement at baseline
Prognostic Considerations
Patients with EGFR exon 19 deletion typically demonstrate:
- Better response rates to EGFR-TKIs than those with L858R
- Longer survival with osimertinib
- Higher chance of CNS involvement, necessitating drugs with CNS activity
Median overall survival in optimized care settings can exceed 3 years.
Future Directions in EGFR-Mutated NSCLC
Emerging Therapies
- Amivantamab: EGFR/MET bispecific antibody
- Lazertinib + amivantamab: Promising in osimertinib-resistant settings
- Antibody-drug conjugates (ADCs): EGFR-targeted payload delivery
- Combination regimens: EGFR-TKI + chemotherapy + anti-angiogenics
Personalized Monitoring
- Longitudinal ctDNA tracking
- AI-assisted radiomics
- Integration of multi-omics data for individualized therapy
Non-small cell lung cancer with EGFR exon 19 deletion is a clinically and molecularly distinct subtype with high responsiveness to EGFR-targeted therapy. The advent of third-generation TKIs like osimertinib has redefined treatment paradigms, offering extended survival and improved quality of life. Timely molecular diagnostics, vigilant resistance monitoring, and participation in clinical trials remain essential to achieving optimal outcomes in this evolving landscape of precision oncology.