Non-small cell lung cancer (NSCLC) accounts for approximately 85% of all lung cancer cases. It encompasses several histological subtypes, including adenocarcinoma, squamous cell carcinoma, and large cell carcinoma. This form of lung cancer tends to grow and spread more slowly than small cell lung cancer (SCLC), allowing for more varied and potentially curative treatment options.
Classification of NSCLC Subtypes
NSCLC includes the following primary histologic types:
- Adenocarcinoma: The most prevalent subtype, typically arising in peripheral lung tissue. Frequently observed in non-smokers.
- Squamous Cell Carcinoma: Often linked with smoking, originating in the central bronchi.
- Large Cell Carcinoma: An undifferentiated group known for rapid growth and poor differentiation.
Risk Factors and Etiology
Primary Risk Factors
- Cigarette smoking (including secondhand exposure)
- Radon gas exposure
- Asbestos and other occupational toxins
- Air pollution
- Genetic susceptibility
- History of chronic obstructive pulmonary disease (COPD)
Genetic and Molecular Alterations
Molecular testing has identified several actionable genetic mutations that guide targeted therapies:
- EGFR mutations
- ALK rearrangements
- ROS1 fusions
- KRAS mutations
- MET exon 14 skipping
- BRAF mutations
Symptoms and Early Warning Signs of NSCLC
NSCLC may be asymptomatic in early stages but typically presents with:
- Persistent cough
- Hemoptysis (coughing up blood)
- Chest pain
- Dyspnea (shortness of breath)
- Unexplained weight loss
- Hoarseness
- Fatigue
Advanced disease may involve bone pain, neurological deficits, or liver dysfunction due to metastasis.
Staging of Non-Small Cell Lung Cancer
NSCLC staging follows the TNM classification:
- T (Tumor size and location)
- N (Lymph node involvement)
- M (Distant metastasis)
The stages are grouped as follows:
| Stage | Description |
|---|---|
| Stage 0 | Carcinoma in situ |
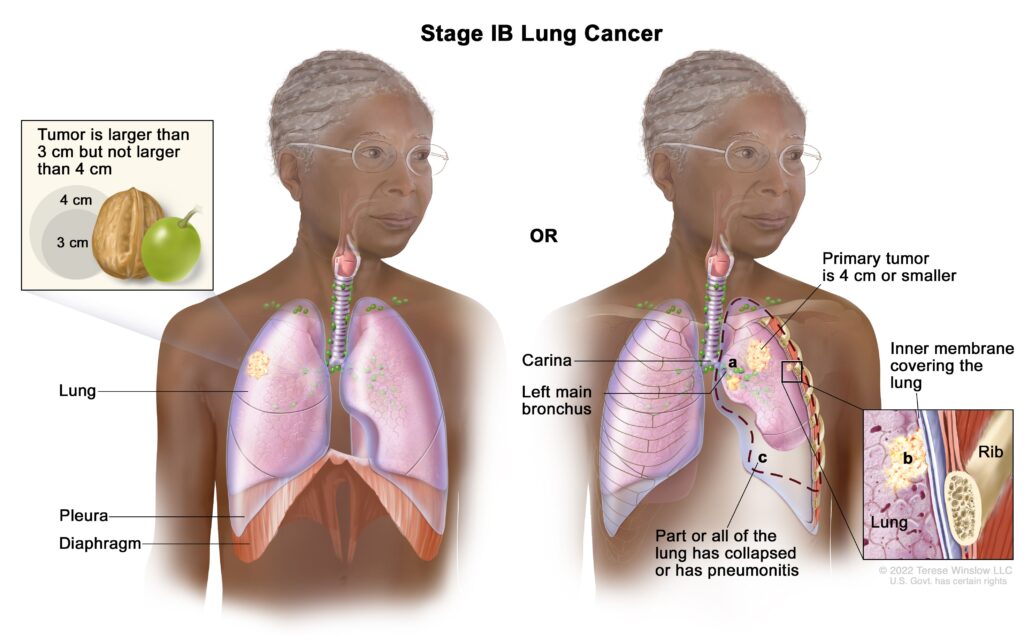
| Stage I | Localized tumor, no lymph node involvement |
| Stage II | Larger tumor, may involve nearby lymph nodes |
| Stage III | Locally advanced, extensive lymph node spread |
| Stage IV | Metastatic disease, distant organ involvement |
Diagnosis of NSCLC
Imaging Techniques
- Chest X-ray: Often the first imaging performed
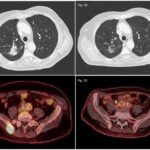
- CT scan: Provides detailed anatomic imaging
- PET-CT scan: Evaluates metabolic activity and metastasis
- MRI: Especially useful for brain metastases
Tissue Sampling
- Bronchoscopy with biopsy
- CT-guided needle biopsy
- Thoracoscopy or mediastinoscopy
Molecular Testing and Biomarkers
- EGFR, ALK, ROS1, BRAF, and PD-L1 expression
- Determines eligibility for targeted or immune therapies
Treatment Options for NSCLC
Surgical Management
Best suited for early-stage (I-II) tumors:
- Lobectomy: Standard approach for resectable disease
- Segmentectomy or wedge resection: For patients with limited pulmonary reserve
- Pneumonectomy: Complete lung removal in select cases
Radiation Therapy
Used in:
- Patients ineligible for surgery
- Postoperative settings (adjuvant)
- Palliation of symptoms
Stereotactic Body Radiotherapy (SBRT) offers high-dose precision treatment for early-stage tumors.
Systemic Therapy
Chemotherapy
- Standard for stage III and IV NSCLC
- Common regimens: Platinum-based doublets (e.g., cisplatin + pemetrexed)
Targeted Therapy
For patients with driver mutations:
| Mutation | Targeted Drugs |
|---|---|
| EGFR | Osimertinib, Erlotinib, Gefitinib |
| ALK | Alectinib, Crizotinib, Lorlatinib |
| ROS1 | Entrectinib, Crizotinib |
| BRAF | Dabrafenib + Trametinib |
Immunotherapy
Checkpoint inhibitors have revolutionized treatment:
- PD-1 inhibitors: Nivolumab, Pembrolizumab
- PD-L1 inhibitors: Atezolizumab, Durvalumab
Used alone or in combination with chemotherapy, depending on PD-L1 expression.
Treatment Strategies by Stage
| Stage | Preferred Treatment |
|---|---|
| Stage I–II | Surgery ± adjuvant chemotherapy or radiation |
| Stage IIIA | Multimodal: Chemoradiotherapy ± surgery |
| Stage IIIB–IIIC | Chemoradiation ± consolidation immunotherapy |
| Stage IV | Targeted therapy or immunotherapy ± chemotherapy |
Survival Rates and Prognosis
Prognosis is largely stage-dependent:
| Stage | 5-Year Survival Rate |
|---|---|
| Stage I | ~68–92% |
| Stage II | ~53–60% |
| Stage III | ~13–36% |
| Stage IV | ~0–10% |
Molecular markers, performance status, and treatment response also influence outcomes. Patients with EGFR or ALK mutations treated with targeted agents often demonstrate improved survival.
Follow-Up and Disease Monitoring
Post-treatment surveillance involves:
- Regular imaging (CT scans every 3–6 months)
- Physical exams
- Tumor marker assessments (if applicable)
- Management of treatment side effects and secondary malignancies
Emerging Therapies and Clinical Trials
Ongoing research explores:
- Next-generation ALK and EGFR inhibitors
- Bispecific antibodies
- Cancer vaccines
- Adoptive cell therapies (e.g., CAR-T cells for solid tumors)
- Combination strategies involving immunotherapy and anti-angiogenic agents
Participation in clinical trials is highly encouraged for advanced NSCLC patients to access novel treatments.
Non-small cell lung cancer is a biologically diverse and therapeutically complex malignancy. The integration of molecular diagnostics, precision-targeted therapies, and immunotherapy has significantly enhanced outcomes for many patients. A stage-specific, multidisciplinary approach remains essential in optimizing survival and quality of life. As therapeutic strategies continue to evolve, early diagnosis, personalized care, and patient participation in clinical trials are paramount in the ongoing battle against NSCLC.