Non-radiographic axial spondyloarthritis (nr-axSpA) is a subtype of axial spondyloarthritis (axSpA), a chronic inflammatory disease that primarily affects the spine and sacroiliac joints. Unlike ankylosing spondylitis (AS), which shows structural damage on X-rays, nr-axSpA lacks definitive radiographic sacroiliitis but may demonstrate inflammation on MRI and is associated with characteristic clinical features.
nr-axSpA can affect both men and women, with onset typically before the age of 45. The disease may remain non-radiographic indefinitely or progress to radiographic axial SpA over time.
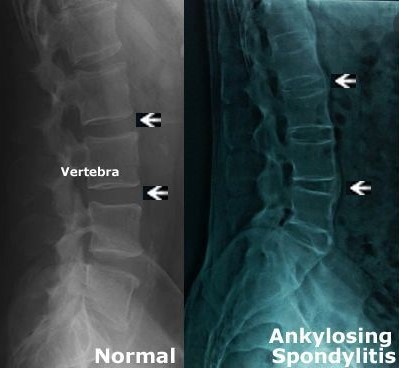
Differentiating Axial Spondyloarthritis Subtypes
Axial spondyloarthritis is classified into two major forms based on imaging:
- Radiographic axSpA (ankylosing spondylitis): Evident structural changes on pelvic X-rays
- Non-radiographic axSpA (nr-axSpA): No definitive changes on X-rays, but may show inflammation on MRI or have positive clinical markers
Pathophysiology and Genetic Associations
nr-axSpA involves chronic inflammation of the axial skeleton, particularly the sacroiliac joints, spine, and entheses (sites where tendons or ligaments attach to bone). The inflammatory process is immune-mediated, with an important genetic predisposition.
HLA-B27 Association
- Up to 90% of patients with axSpA are HLA-B27 positive
- Presence of this allele is a significant risk factor, particularly in individuals with early-onset inflammatory back pain
Other genetic and environmental factors also contribute, including:
- Gut microbiome dysbiosis
- Mechanical stress at entheses
- Cytokine dysregulation (TNF-α, IL-17)
Clinical Features of nr-axSpA
Core Symptoms
Patients commonly report:
- Inflammatory back pain (IBP):
- Onset < 45 years of age
- Insidious onset, lasting >3 months
- Morning stiffness >30 minutes
- Improvement with exercise, not rest
- Alternating buttock pain
- Peripheral arthritis (especially lower limbs)
- Enthesitis (e.g., Achilles tendon, plantar fascia)
- Fatigue
Extra-articular Manifestations
- Uveitis (acute anterior)
- Psoriasis
- Inflammatory bowel disease (IBD)
- Dactylitis (sausage digits)
Diagnosis of Non-Radiographic Axial Spondyloarthritis
ASAS Classification Criteria
The Assessment of SpondyloArthritis International Society (ASAS) developed criteria for early diagnosis of axSpA, including both imaging and clinical arms.
ASAS criteria for nr-axSpA (≥ 3 months back pain, age <45):
- Imaging arm:
- Sacroiliitis on MRI plus ≥1 SpA feature
- Clinical arm:
- HLA-B27 positive plus ≥2 SpA features
SpA features include:
- Inflammatory back pain
- Arthritis
- Enthesitis
- Uveitis
- Dactylitis
- Psoriasis
- Crohn’s disease/ulcerative colitis
- Good response to NSAIDs
- Family history of SpA
- Elevated CRP
Diagnostic Workup
- MRI of the sacroiliac joints: Detects active inflammation (bone marrow edema)
- X-rays: Absence of sacroiliac joint erosion or sclerosis
- Blood tests: HLA-B27, ESR, CRP
- Physical exam: Schober test, sacroiliac joint tenderness
Treatment Strategies for nr-axSpA
Non-Pharmacological Management
- Exercise programs: Daily physical therapy and spinal mobility exercises improve posture, pain, and function
- Patient education: Critical for adherence and self-management
- Smoking cessation: Smoking worsens disease progression and reduces treatment response
Pharmacological Treatment
| Medication Class | Role in nr-axSpA |
|---|---|
| NSAIDs | First-line for pain and stiffness |
| TNF inhibitors | Indicated for NSAID-refractory cases |
| IL-17 inhibitors | Alternative to TNFi, especially in psoriasis |
| Analgesics | Adjunct for symptom control |
| DMARDs | Limited role in axial disease, used for peripheral symptoms |
Biologic Therapies
- TNF inhibitors:
- Etanercept, Adalimumab, Infliximab, Certolizumab pegol
- Demonstrated efficacy in reducing inflammation, improving MRI findings
- IL-17 inhibitors:
- Secukinumab, Ixekizumab
- Beneficial in TNFi failures or psoriasis comorbidity
Disease Monitoring and Outcome Measures
Regular monitoring is essential to evaluate disease activity and response to therapy.
Assessment Tools
- BASDAI (Bath Ankylosing Spondylitis Disease Activity Index)
- ASDAS (Ankylosing Spondylitis Disease Activity Score)
- MRI imaging: Periodic reassessment of sacroiliac inflammation
- CRP/ESR: Inflammatory markers for tracking flare-ups
Prognosis and Risk of Progression
Progression to Radiographic axSpA
- Approximately 10–40% of nr-axSpA patients develop AS over 10 years
- Risk factors for progression:
- Male sex
- Elevated CRP
- MRI evidence of sacroiliitis
- HLA-B27 positivity
- Smoking
Early intervention with biologic therapy may slow or prevent structural damage.
Non-Radiographic Axial Spondyloarthritis in Women
- Women with nr-axSpA often present with more peripheral symptoms and fatigue
- Tend to have delayed diagnosis
- Less likely to progress to AS but may experience significant functional impairment
- Emphasizes need for gender-sensitive diagnostic approaches
Emerging Therapies and Future Directions
Ongoing research aims to refine treatments and improve early diagnosis.
New and Investigational Therapies
- Janus kinase inhibitors (JAKi): Tofacitinib, upadacitinib showing potential in SpA
- Dual inhibitors targeting IL-17 and TNF pathways
- Personalized medicine based on biomarkers and genetic profiling
Advanced Imaging
- Whole-body MRI: To assess enthesitis and axial inflammation
- Quantitative MRI metrics: For objective monitoring of treatment response
Non-radiographic axial spondyloarthritis represents a significant burden due to invisible inflammation, delayed diagnosis, and variable progression. Recognition of early symptoms, prompt use of MRI, and implementation of ASAS criteria enable accurate diagnosis and timely intervention. A multidisciplinary approach combining physical therapy and biologic therapy ensures optimal outcomes, while ongoing advancements in imaging and therapeutics continue to enhance the care paradigm.