Non Infectious Uveitis: Non-infectious uveitis is a form of intraocular inflammation not caused by pathogens but driven by immune-mediated or idiopathic mechanisms. It affects the uvea—the middle layer of the eye consisting of the iris, ciliary body, and choroid—and may extend to adjacent tissues such as the retina and vitreous body.
This condition represents a significant cause of vision impairment and blindness worldwide, especially in working-age adults. Early diagnosis and effective management are crucial for preserving visual function and minimizing complications.
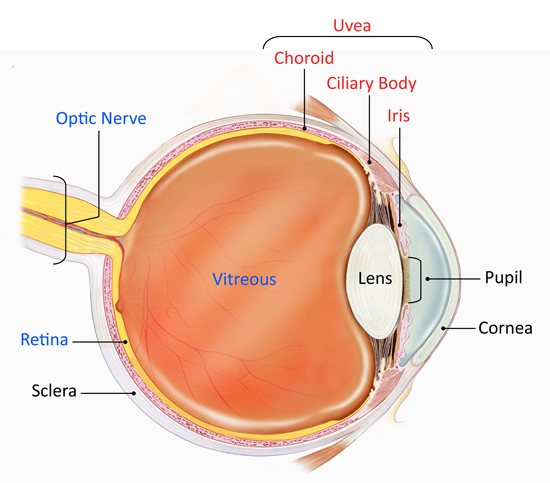
Classification of Non Infectious Uveitis by Anatomical Location
Anterior Uveitis
- Location: Iris and ciliary body
- Symptoms: Redness, photophobia, pain, blurred vision
- Common in: HLA-B27-associated diseases (e.g., ankylosing spondylitis)
Intermediate Uveitis
- Location: Vitreous, peripheral retina
- Symptoms: Floaters, mild vision loss
- Associated with: Multiple sclerosis, sarcoidosis
Posterior Uveitis
- Location: Retina and choroid
- Symptoms: Blurred vision, floaters, scotomas
- Causes: Sarcoidosis, birdshot retinochoroidopathy
Panuveitis
- Location: Involves all uveal segments
- Symptoms: Severe vision loss, ocular pain, inflammation
- Examples: Vogt-Koyanagi-Harada (VKH) disease, Behçet’s disease
Underlying Causes
Autoimmune and Systemic Inflammatory Diseases
- HLA-B27-related conditions: Ankylosing spondylitis, reactive arthritis
- Behçet’s disease: Recurrent panuveitis with retinal vasculitis
- Sarcoidosis: Granulomatous inflammation affecting lungs and eyes
- Juvenile idiopathic arthritis (JIA): Common in children with chronic anterior uveitis
- Systemic lupus erythematosus (SLE) and granulomatosis with polyangiitis
Idiopathic Uveitis
- In many cases, no underlying cause is identified. These are labeled as idiopathic non-infectious uveitis and often follow a recurrent or chronic course.
Clinical Manifestations and Symptoms
Common Ocular Symptoms
- Eye redness and pain
- Photophobia (light sensitivity)
- Blurred vision
- Floaters (small dark shapes in the visual field)
- Visual field loss in severe cases
Chronic and Recurrent Features
- Progressive vision loss
- Posterior synechiae (iris adherence to lens)
- Cataract formation
- Glaucoma
- Cystoid macular edema (CME)
Diagnostic Approach
Clinical Examination
- Slit-lamp biomicroscopy to assess anterior chamber cells and flare
- Fundus examination for vitreous haze, retinal vasculitis, choroidal lesions
- Tonometry to monitor intraocular pressure
Imaging and Laboratory Testing
- Optical coherence tomography (OCT): Detects macular edema and retinal layers
- Fluorescein angiography (FA): Visualizes retinal vasculature leakage
- Chest X-ray/CT: Evaluates sarcoidosis or tuberculosis (to exclude infectious causes)
- Serological markers: ANA, HLA-B27, ACE, ANCA
Exclusion of Infectious Causes
A definitive diagnosis of non-infectious uveitis necessitates rule-out of infectious etiologies, including:
- Herpes viruses
- Toxoplasmosis
- Tuberculosis
- Syphilis
Treatment Strategies
Topical Corticosteroids
- Mainstay for anterior uveitis
- Examples: Prednisolone acetate, dexamethasone drops
- Frequency depends on severity
Systemic Corticosteroids
- Indicated for posterior or panuveitis
- Prednisone is commonly used with tapering schedules
- Monitor for systemic side effects: weight gain, hypertension, osteoporosis
Immunomodulatory Therapy (IMT)
For corticosteroid-sparing and chronic cases:
- Methotrexate
- Azathioprine
- Mycophenolate mofetil
- Requires regular monitoring of liver function and blood counts
Biologic Agents
Used in refractory or vision-threatening uveitis:
- Anti-TNF agents (e.g., adalimumab, infliximab) for Behçet’s and HLA-B27-related uveitis
- Interleukin inhibitors (e.g., tocilizumab)
- FDA-approved options like adalimumab (Humira) for non-infectious intermediate, posterior, and panuveitis
Surgical Interventions
- Vitrectomy: For persistent vitreous haze or tractional membranes
- Cataract extraction: In steroid-induced cataract cases
- Glaucoma surgery: If intraocular pressure is uncontrolled
Complications of Non-Infectious Uveitis
- Cataract formation
- Secondary glaucoma
- Macular edema
- Retinal detachment
- Optic nerve damage
These complications underscore the importance of early diagnosis and aggressive management.
Prognosis and Long-Term Outlook
The visual outcome is heavily dependent on:
- Anatomic type and severity
- Timeliness and adequacy of treatment
- Presence of systemic autoimmune disease
- With modern therapies, many patients can maintain functional vision and lead a normal life, provided that chronic inflammation is controlled and follow-up is consistent.
Frequently Asked Questions:
What distinguishes non-infectious uveitis from infectious uveitis?
Non-infectious uveitis is caused by autoimmune or idiopathic inflammation without any infectious pathogen. It requires different treatment approaches focused on immune suppression.
Can non-infectious uveitis lead to permanent vision loss?
Yes, especially if left untreated. Persistent inflammation can damage the retina, optic nerve, or macula, resulting in irreversible vision impairment.
Is non-infectious uveitis curable?
While not always curable, non-infectious uveitis can be controlled effectively with immunosuppressive therapy and regular ophthalmologic care.
How long does treatment last?
Treatment duration depends on severity and response. Some cases require only short-term therapy, while others may need long-term or lifelong immunosuppression.
Can children develop non-infectious uveitis?
Yes. Juvenile idiopathic arthritis is a major cause of chronic anterior uveitis in children and requires careful, long-term management.
Non-infectious uveitis is a complex, immune-mediated ocular disorder that requires prompt diagnosis, tailored treatment, and long-term surveillance. With advancements in biologic therapies and refined clinical strategies, the potential for vision preservation and improved quality of life has significantly increased for patients affected by this condition.