Nocturia is a urinary disorder characterized by frequent urination during the night, disrupting sleep and affecting overall well-being. Unlike typical nighttime awakenings, nocturia involves waking up two or more times to urinate. This condition is often linked to aging, medical conditions, lifestyle habits, or underlying urinary tract issues. Proper diagnosis and treatment are essential to improving sleep quality and overall health.
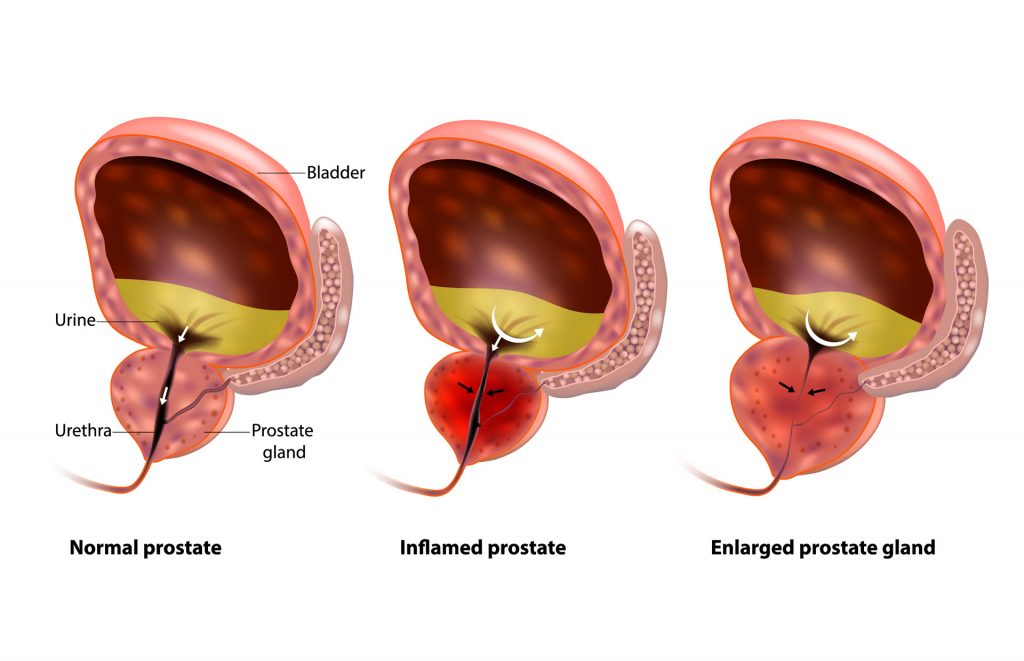
Understanding Nocturia: What Causes Frequent Nighttime Urination?
1. Increased Urine Production (Nocturnal Polyuria)
Nocturnal polyuria occurs when the body produces excessive urine at night, surpassing normal levels. Causes include:
- Excess fluid intake before bed
- Diabetes mellitus or diabetes insipidus
- Congestive heart failure (CHF)
- Kidney dysfunction
- Use of diuretics (water pills)
- Sleep disorders like obstructive sleep apnea (OSA)
2. Reduced Bladder Capacity
A small bladder capacity or overactive bladder (OAB) can lead to frequent nighttime urination. Causes include:
- Bladder infections (cystitis)
- Enlarged prostate (benign prostatic hyperplasia, BPH) in men
- Bladder stones or tumors
- Interstitial cystitis (chronic bladder inflammation)
3. Hormonal Changes
- Aging leads to a decline in antidiuretic hormone (ADH) production, resulting in increased nighttime urine output.
- Menopause and pregnancy can contribute to bladder dysfunction in women.
4. Sleep Disorders and Lifestyle Factors
- Poor sleep patterns, insomnia, and restless leg syndrome (RLS) can trigger nocturia.
- Alcohol, caffeine, and excessive fluid intake before bedtime worsen symptoms.
Symptoms of Nocturia
- Frequent nighttime urination (two or more times per night)
- Disrupted sleep leading to daytime fatigue
- Urgency to urinate at night with or without incontinence
- Increased urine volume at night (polyuria)
- Lower back pain or pelvic discomfort in cases of bladder infections
Who Is at Risk for Nocturia?
- Older adults (above 60 years) due to natural aging changes
- Men with prostate enlargement (BPH)
- Women undergoing pregnancy or menopause
- Individuals with diabetes or kidney disease
- People with heart failure or liver disease
- Patients taking diuretics or medications affecting urine production
Diagnosis: How Is Nocturia Evaluated?
1. Medical History and Symptom Assessment
A healthcare provider will assess:
- Frequency of urination at night
- Fluid intake patterns
- Existing medical conditions and medications
2. Urinalysis and Blood Tests
- Urinalysis detects infections, kidney disease, or diabetes.
- Blood tests evaluate electrolyte levels and kidney function.
3. Bladder Diary (Voiding Chart)
Patients track their urination patterns, fluid intake, and volume of urine output for 24-72 hours.
4. Imaging and Specialized Tests
- Ultrasound or CT scans to check for bladder abnormalities.
- Uroflowmetry and cystometry assess bladder function.
- Sleep studies (polysomnography) to diagnose underlying sleep disorders.
Treatment and Management of Nocturia
1. Lifestyle Modifications
- Limit fluid intake in the evening, especially caffeinated or alcoholic beverages.
- Reduce salt consumption to control fluid retention.
- Elevate legs during the day to prevent fluid buildup.
2. Medications for Nocturia
- Desmopressin (synthetic ADH) reduces nighttime urine production.
- Anticholinergic drugs help manage overactive bladder.
- Alpha-blockers (Tamsulosin, Doxazosin) for men with enlarged prostates.
- Diuretics (taken earlier in the day) reduce fluid retention.
3. Treating Underlying Conditions
- Manage diabetes and kidney disease to regulate urine production.
- Address heart failure or liver disease to prevent excess fluid accumulation.
- Treat infections and bladder disorders with antibiotics or anti-inflammatory medications.
4. Bladder Training and Pelvic Floor Exercises
- Timed voiding techniques help regulate urination patterns.
- Kegel exercises strengthen pelvic muscles to reduce urgency.
Complications of Untreated Nocturia
- Chronic sleep deprivation, leading to daytime fatigue and cognitive impairment.
- Increased risk of falls and fractures, especially in elderly individuals.
- Mental health issues, including anxiety and depression due to poor sleep.
Preventing Nocturia: Practical Tips
- Monitor and limit fluid intake before bedtime.
- Maintain a healthy weight to reduce pressure on the bladder.
- Avoid bladder irritants like alcohol, caffeine, and acidic foods.
- Use compression stockings to prevent leg swelling and fluid retention.
- Practice good sleep hygiene by maintaining a regular sleep schedule.
Nocturia significantly impacts sleep quality, daily functioning, and overall health. Understanding its causes, symptoms, and treatment options is crucial for managing this condition effectively. By making lifestyle changes, seeking medical treatment, and addressing underlying conditions, individuals can improve their nighttime urination patterns and enhance their quality of life.