Neutropenia Secondary to AML Treatment: Neutropenia is a severe reduction in neutrophil count, a type of white blood cell essential for fighting infections. In patients undergoing treatment for acute myeloid leukemia (AML), neutropenia is a frequent and dangerous side effect caused by chemotherapy, radiation therapy, and bone marrow suppression. This condition increases susceptibility to infections, complicating AML treatment and recovery.
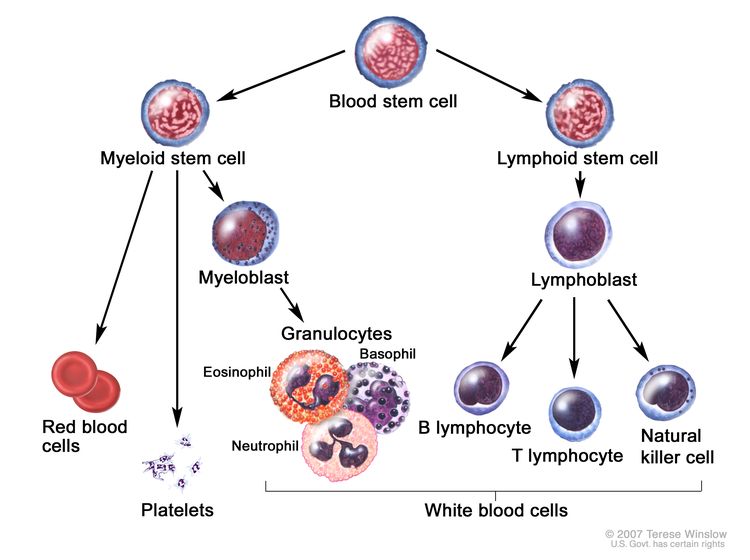
Pathophysiology of Neutropenia in AML Treatment
Neutropenia occurs due to bone marrow suppression, which inhibits the production of neutrophils. AML itself disrupts normal hematopoiesis, and aggressive treatments further impair bone marrow function, reducing the body’s ability to fight infections.
Causes of Neutropenia in AML Treatment
1. Chemotherapy-Induced Neutropenia
- Cytotoxic drugs (e.g., cytarabine, daunorubicin) destroy both cancerous and healthy cells, leading to bone marrow suppression.
- Neutrophil counts typically decline 7-10 days post-chemotherapy.
2. Radiation Therapy Effects
- Radiation targeting the bone marrow directly affects neutrophil production, prolonging neutropenia.
3. Bone Marrow Transplantation (BMT)
- High-dose chemotherapy before stem cell transplantation leads to prolonged neutropenia until engraftment occurs.
4. Disease-Related Factors
- AML itself disrupts normal myeloid cell production, contributing to neutropenia even before treatment begins.
Symptoms and Complications of Neutropenia
Neutropenia often presents without symptoms, but its primary danger lies in increased infection susceptibility.
Common Symptoms
- Fever (>38.3°C or >101°F) – A hallmark of febrile neutropenia.
- Chills, sweats, or body aches.
- Sore throat or mouth ulcers.
- Fatigue and general weakness.
Complications of Severe Neutropenia
- Febrile Neutropenia (FN): A life-threatening condition requiring immediate hospitalization and IV antibiotics.
- Sepsis: Severe infections can progress to organ failure and death.
- Delayed AML Treatment: Prolonged neutropenia may require dose reductions or treatment delays, affecting AML prognosis.
Diagnosis of Neutropenia in AML Patients
1. Complete Blood Count (CBC) with Differential
- Absolute Neutrophil Count (ANC) is the primary indicator:
- Mild Neutropenia: ANC 1000–1500/μL
- Moderate Neutropenia: ANC 500–1000/μL
- Severe Neutropenia: ANC <500/μL
2. Infection Screening
- Blood cultures, urine analysis, and chest X-rays help identify bacterial, viral, or fungal infections.
3. Bone Marrow Biopsy (If Needed)
- Evaluates bone marrow function and cellularity in cases of persistent neutropenia.
Management and Treatment of Neutropenia
1. Infection Prevention Strategies
- Hand hygiene and protective isolation in severe cases.
- Avoidance of raw foods and unpasteurized dairy to reduce exposure to pathogens.
- Daily prophylactic antibiotics in high-risk patients.
2. Granulocyte Colony-Stimulating Factor (G-CSF) Therapy
- Filgrastim (Neupogen) or Pegfilgrastim (Neulasta) stimulates neutrophil production, reducing infection risk and recovery time.
3. Empirical Antibiotic Therapy
- Broad-spectrum IV antibiotics (e.g., cefepime, piperacillin-tazobactam) are given immediately for febrile neutropenia.
4. Antifungal and Antiviral Prophylaxis
- Fluconazole or posaconazole for fungal infection prevention.
- Acyclovir or valacyclovir for viral prophylaxis in immunocompromised patients.
5. Blood and Bone Marrow Support
- Colony-stimulating factors (CSFs) help shorten the duration of neutropenia.
- Stem cell transplantation may be considered in refractory AML cases.
Recovery and Long-Term Outlook
Neutrophil recovery depends on several factors:
- Time since last chemotherapy cycle (neutrophil counts typically recover within 2-3 weeks).
- Response to G-CSF therapy.
- Presence of ongoing infections or AML relapse.
With proactive management, neutropenic complications can be minimized, improving AML treatment outcomes.
Neutropenia secondary to AML treatment is a serious but manageable condition. Through infection prevention, G-CSF therapy, and prompt antimicrobial treatment, patients can navigate neutropenia with reduced risk of life-threatening complications. Regular blood monitoring and personalized treatment adjustments are essential to optimizing recovery and AML treatment success.