Neuropathic pain is a complex, chronic pain condition caused by damage or dysfunction of the nervous system. Unlike nociceptive pain, which results from tissue injury or inflammation, neuropathic pain arises from abnormal nerve signaling. It can be spontaneous, persistent, or triggered by stimuli that normally do not cause pain. Common conditions associated with neuropathic pain include diabetes, shingles, multiple sclerosis, spinal cord injuries, and chemotherapy-induced nerve damage.
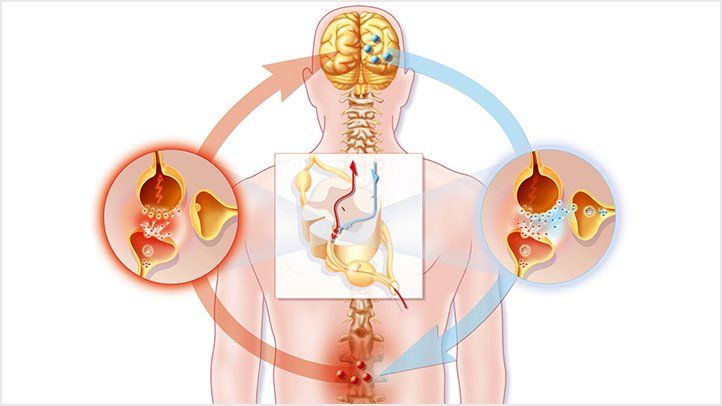
Pathophysiology of Neuropathic Pain
Neuropathic pain results from altered neuronal function and abnormal signal processing in the peripheral and central nervous systems.
- Peripheral nerve damage leads to increased excitability of nociceptive neurons.
- Central sensitization occurs due to persistent nerve stimulation, leading to exaggerated pain responses.
- Dysregulated neurotransmitters such as glutamate and substance P contribute to chronic pain perception.
Causes of Neuropathic Pain
Neuropathic pain can result from various medical conditions and injuries affecting the nervous system.
1. Peripheral Neuropathies
✅ Diabetic neuropathy – High blood sugar damages peripheral nerves.
✅ Postherpetic neuralgia – Nerve damage following a shingles infection.
✅ Trigeminal neuralgia – Intense facial pain due to trigeminal nerve dysfunction.
✅ Entrapment neuropathies – Compression of nerves (e.g., carpal tunnel syndrome).
2. Central Nervous System Disorders
✅ Multiple sclerosis (MS) – Autoimmune attack on myelin sheaths affects nerve transmission.
✅ Spinal cord injury – Disrupted nerve pathways cause chronic neuropathic pain.
✅ Stroke – Damage to the brain’s pain-processing centers.
3. Medication and Treatment-Related Causes
✅ Chemotherapy-induced neuropathy – Nerve toxicity from cancer treatments.
✅ Radiation-induced nerve damage – Following radiotherapy for tumors.
4. Other Conditions
✅ Complex regional pain syndrome (CRPS) – Severe pain post-injury or surgery.
✅ HIV-related neuropathy – Nerve damage due to viral infection or medications.
Symptoms of Neuropathic Pain
Neuropathic pain presents with a wide range of sensory abnormalities.
1. Primary Symptoms
- Burning pain – Persistent sensation of heat or tingling.
- Electric shock-like sensations – Sudden jolts of pain.
- Stabbing or shooting pain – Intermittent, sharp pain episodes.
2. Sensory Changes
- Allodynia – Pain caused by normally non-painful stimuli (e.g., light touch).
- Hyperalgesia – Exaggerated pain response to mild stimuli.
- Paresthesia – Abnormal tingling, prickling, or numbness.
3. Autonomic and Motor Symptoms
- Skin color changes – In CRPS, skin may appear mottled or swollen.
- Muscle weakness or atrophy – Due to nerve damage affecting motor function.
Diagnosis of Neuropathic Pain
Accurate diagnosis is critical for effective pain management.
1. Clinical History and Physical Examination
- Medical history – Identifying conditions like diabetes, infections, or prior nerve injuries.
- Pain characterization – Describing pain onset, location, intensity, and triggering factors.
- Neurological examination – Testing reflexes, sensory responses, and motor function.
2. Diagnostic Tests
- Nerve conduction studies (NCS) – Evaluates electrical nerve signaling.
- Electromyography (EMG) – Assesses muscle and nerve function.
- Skin biopsy – Detects small fiber neuropathy.
- MRI or CT scans – Identifies structural abnormalities affecting nerves.
Treatment of Neuropathic Pain
Effective management requires a multimodal approach, combining medications, physical therapy, and interventional procedures.
1. Pharmacological Treatments
First-Line Medications
- Anticonvulsants (Gabapentin, Pregabalin) – Modulate nerve signaling and reduce hyperexcitability.
- Tricyclic antidepressants (Amitriptyline, Nortriptyline) – Inhibit pain pathways.
- Serotonin-norepinephrine reuptake inhibitors (Duloxetine, Venlafaxine) – Block pain neurotransmitters.
Second-Line Medications
- Opioids (Tramadol, Tapentadol) – Used for severe, refractory cases.
- Topical agents (Lidocaine patches, Capsaicin cream) – Reduce localized nerve pain.
2. Interventional Therapies
- Nerve blocks – Injections of local anesthetics near affected nerves.
- Spinal cord stimulation (SCS) – Implanted device that modulates pain signals.
- Intrathecal drug delivery – Direct pain medication administration to the spinal cord.
3. Physical Therapy and Lifestyle Modifications
- Transcutaneous electrical nerve stimulation (TENS) – Non-invasive nerve stimulation.
- Exercise and physiotherapy – Improves mobility and reduces stiffness.
- Acupuncture and alternative therapies – May provide additional relief.
Complications of Neuropathic Pain
Without proper treatment, neuropathic pain can lead to significant physical and psychological consequences.
- Chronic disability – Reduced mobility and function.
- Depression and anxiety – Due to persistent pain and limited quality of life.
- Sleep disturbances – Pain exacerbates insomnia and sleep disorders.
Prevention and Long-Term Management
1. Preventive Strategies
- Early blood sugar control to prevent diabetic neuropathy.
- Vaccination for shingles to reduce postherpetic neuralgia risk.
- Proper ergonomics and posture to prevent nerve compression syndromes.
2. Long-Term Management
- Regular medical follow-ups to adjust treatment plans.
- Cognitive behavioral therapy (CBT) to manage pain perception.
- Holistic approaches including meditation, yoga, and biofeedback.
Neuropathic pain is a chronic, debilitating condition that requires early diagnosis and a comprehensive treatment approach. Advances in pain management offer effective therapies, but personalized treatment plans remain essential. By combining pharmacological, interventional, and lifestyle interventions, patients can improve their quality of life and manage long-term pain effectively.