Neurocysticercosis (NCC) is a parasitic infection of the central nervous system (CNS) caused by the larvae of Taenia solium, the pork tapeworm. It is the most common cause of acquired epilepsy worldwide, particularly in endemic regions such as Latin America, sub-Saharan Africa, and South Asia. Transmission occurs through ingestion of T. solium eggs, often via contaminated food or water. The condition manifests with a broad range of neurological symptoms, including seizures, headaches, hydrocephalus, and cognitive impairment.
Causes and Transmission of Neurocysticercosis
1. Life Cycle of Taenia solium
Neurocysticercosis results from the accidental ingestion of T. solium eggs, which hatch in the intestine and migrate to various tissues, including the brain, muscles, and eyes.
2. Modes of Transmission
- Fecal-Oral Route: Poor hygiene and ingestion of food or water contaminated with T. solium eggs.
- Autoinfection: Individuals infected with the adult tapeworm may ingest eggs through contaminated hands.
- Consumption of Undercooked Pork: Though pork consumption leads to intestinal taeniasis, neurocysticercosis occurs only when eggs are ingested.
Clinical Manifestations of Neurocysticercosis
Symptoms depend on the location, number, and stage of cysticerci in the brain.
1. Parenchymal Neurocysticercosis
- Seizures: The most common symptom, occurring in 70-90% of cases.
- Headache and Nausea: Often due to inflammatory response to dying cysts.
- Cognitive Decline: Chronic infection may cause memory loss and personality changes.
2. Extraparenchymal Neurocysticercosis
- Hydrocephalus and Increased Intracranial Pressure (ICP): Due to cyst obstruction in the ventricles.
- Meningitis and Vasculitis: Inflammation caused by cyst rupture leads to stroke-like symptoms.
- Vision Loss: Occurs when cysts invade the optic nerves or subarachnoid space.
Diagnosis of Neurocysticercosis
1. Neuroimaging
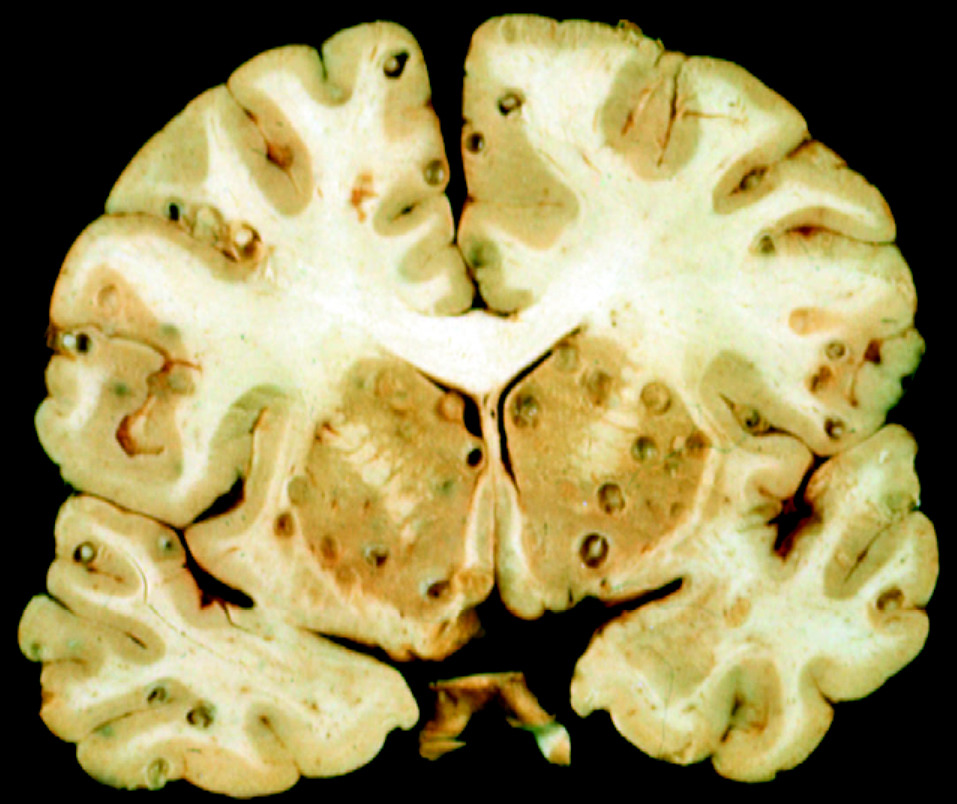
- MRI and CT Scans reveal cystic lesions with or without calcifications.
- Contrast-enhanced MRI shows enhancing rings around inflamed cysts.
2. Serological and Molecular Tests
- Enzyme-Linked Immunoelectrotransfer Blot (EITB): Highly specific for detecting T. solium antibodies.
- ELISA (Enzyme-Linked Immunosorbent Assay): Useful for detecting T. solium antigens in CSF or blood.
- Polymerase Chain Reaction (PCR): Confirms infection by identifying parasitic DNA in cerebrospinal fluid (CSF).
3. Cerebrospinal Fluid (CSF) Analysis
- Increased white blood cells, protein, and reduced glucose suggest inflammatory NCC.
- Positive T. solium DNA or antigens confirm the presence of active infection.
Classification and Staging of Neurocysticercosis
The disease progresses through four pathological stages:
| Stage | Description | Imaging Features |
|---|---|---|
| Vesicular Stage | Viable cyst with a translucent fluid and live parasite | Clear cyst with no inflammation |
| Colloidal Stage | Cyst degeneration triggers immune response | Enhancing cyst with edema |
| Granular Nodular Stage | Host response leads to fibrosis and granuloma formation | Thick-walled lesion |
| Calcified Stage | Dead cyst turns into a calcified nodule | Small calcifications |
Treatment of Neurocysticercosis
1. Antiparasitic Therapy
- Albendazole (15 mg/kg/day) for 7-14 days – First-line drug for active cysts.
- Praziquantel (50-100 mg/kg/day) for 10-14 days – Alternative treatment, often combined with Albendazole.
2. Corticosteroids
- Dexamethasone or Prednisone reduces inflammation and edema during antiparasitic therapy.
- Important in preventing worsening of neurological symptoms.
3. Antiepileptic Drugs (AEDs)
- Carbamazepine, Levetiracetam, or Phenytoin for seizure control.
- Duration of therapy depends on lesion resolution in imaging.
4. Surgical Management
- Ventriculoperitoneal (VP) Shunting for hydrocephalus relief.
- Endoscopic Cyst Removal for ventricular or subarachnoid cysts.
Prognosis and Long-Term Outcomes
- Parenchymal NCC with calcified lesions has a good prognosis, but seizures may persist.
- Extraparenchymal forms (e.g., ventricular NCC) require aggressive management due to high mortality risk.
- Seizure recurrence risk: 20-50% even after cyst resolution.
Prevention of Neurocysticercosis
1. Hygiene and Sanitation Measures
- Handwashing after using the restroom and before meals.
- Proper sewage disposal to prevent contamination of soil and water.
2. Food Safety Practices
- Cooking pork at ≥160°F (71°C) to kill T. solium cysticerci.
- Avoiding raw or undercooked pork in endemic regions.
3. Mass Drug Administration (MDA) in Endemic Areas
- Deworming programs using Praziquantel or Niclosamide reduce tapeworm prevalence.
- Vaccination of pigs against T. solium prevents transmission.
Neurocysticercosis remains a significant global health burden, particularly in low-income regions where sanitation and food safety measures are inadequate. Advances in diagnostics, antiparasitic therapies, and surgical techniques have improved outcomes, but early detection and prevention remain key to reducing morbidity and mortality. Addressing public health challenges through education, hygiene promotion, and parasite control programs will be critical in eradicating this disease.