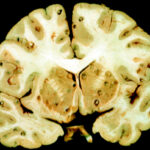
Neuroblastoma is a rare pediatric cancer that originates in the sympathetic nervous system, often affecting the adrenal glands or nerve tissue along the spine. It is the most common extracranial solid tumor in children, accounting for 8-10% of all childhood cancers. Most cases occur in children under 5 years of age, with approximately 90% diagnosed before the age of 10.
This highly heterogeneous tumor presents a wide spectrum of behavior, ranging from spontaneous regression to aggressive metastatic disease. Research has identified genetic markers, such as MYCN amplification, that influence prognosis and treatment strategies.
Causes and Risk Factors
1. Genetic Mutations and Molecular Mechanisms
Neuroblastoma arises from neural crest cells, which contribute to the development of the sympathetic nervous system. Key genetic alterations include:
- MYCN amplification – Present in 20-25% of cases, associated with high-risk tumors.
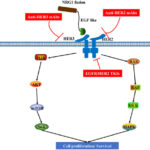
- ALK (Anaplastic Lymphoma Kinase) mutations – Found in sporadic and familial cases.
- Chromosomal abnormalities – 1p and 11q deletions indicate poor prognosis.
2. Environmental and Hereditary Factors
- Familial Neuroblastoma: 1-2% of cases show an autosomal dominant inheritance pattern due to ALK or PHOX2B gene mutations.
- Environmental Exposure: Limited evidence suggests that prenatal exposure to toxins may increase risk.
- Congenital Conditions: Some neurodevelopmental disorders have been linked to an increased incidence of neuroblastoma.
Signs and Symptoms of Neuroblastoma
The clinical presentation varies depending on the tumor location and extent of metastasis.
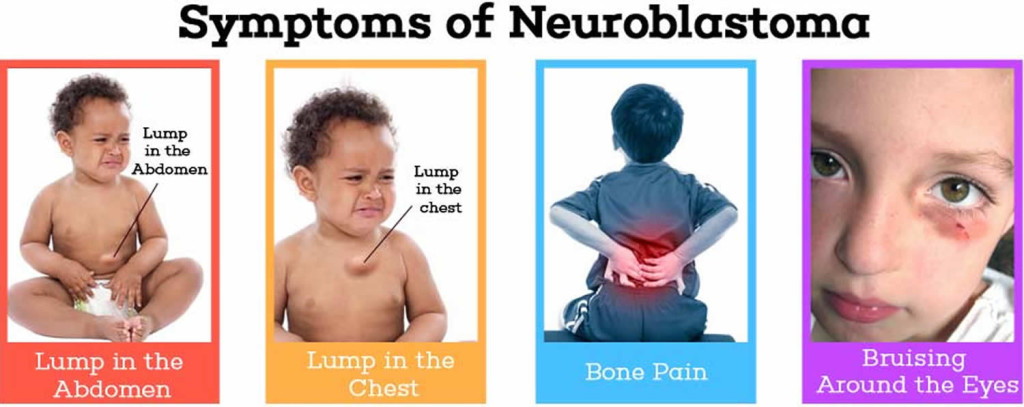
1. Primary Tumor Symptoms
- Abdominal Mass – Often detected as a firm, non-tender lump.
- Bone Pain – If the tumor has spread to the bone marrow or skeletal system.
- Horner’s Syndrome – Ptosis (drooping eyelid), miosis (pupil constriction), and anhidrosis (lack of sweating) if the tumor affects the cervical sympathetic chain.
2. Systemic Symptoms
- Fever, Weight Loss, Fatigue – Signs of advanced disease.
- Hypertension and Sweating – Due to excessive catecholamine secretion from tumor cells.
3. Paraneoplastic Syndromes
- Opsoclonus-Myoclonus Syndrome (OMS) – Rapid eye movements and muscle jerks, linked to an immune response against neuroblastoma.
- Secretory Diarrhea – Caused by tumor production of vasoactive intestinal peptide (VIP).
Staging of Neuroblastoma
Neuroblastoma is classified using the International Neuroblastoma Staging System (INSS) and the newer International Neuroblastoma Risk Group (INRG) system.
INSS Staging System
| Stage | Description | Prognosis |
|---|---|---|
| Stage 1 | Localized tumor, complete resection possible | Excellent |
| Stage 2A/2B | Localized tumor with/without lymph node involvement | Good |
| Stage 3 | Unresectable tumor crossing the midline | Moderate |
| Stage 4 | Metastatic disease in bone marrow, liver, or skin | Poor |
| Stage 4S | Special stage for infants (<1 year) with limited metastasis | Favorable |
Diagnosis of Neuroblastoma
1. Laboratory Tests
- Urine Catecholamines: Increased levels of HVA (homovanillic acid) and VMA (vanillylmandelic acid) confirm neuroblastoma.
- Blood Markers: LDH, NSE (neuron-specific enolase), and ferritin levels may be elevated.
2. Imaging Studies
- Ultrasound and CT/MRI scans to determine tumor size and spread.
- MIBG (Metaiodobenzylguanidine) Scintigraphy – A highly specific imaging technique for neuroblastoma metastases.
3. Biopsy and Genetic Testing
- Tumor biopsy confirms histological diagnosis.
- Genetic profiling assesses MYCN amplification and other risk factors.
Treatment Options for Neuroblastoma
1. Surgery
- Preferred for localized tumors (Stage 1-2) when complete resection is possible.
- Partial resection may be performed in high-risk cases before chemotherapy.
2. Chemotherapy
- Induction chemotherapy for high-risk neuroblastoma (Cyclophosphamide, Cisplatin, Doxorubicin, Vincristine).
- Maintenance chemotherapy to prevent recurrence.
3. Radiation Therapy
- Used in residual disease after surgery or for palliative care in metastatic cases.
4. Immunotherapy and Targeted Therapy
- Anti-GD2 Monoclonal Antibodies (Dinutuximab, Naxitamab) – Standard treatment for high-risk neuroblastoma.
- ALK Inhibitors (Crizotinib, Lorlatinib) for ALK-mutated tumors.
- Retinoids (Isotretinoin) to prevent relapse in high-risk cases.
5. Stem Cell Transplantation
- Autologous stem cell transplant (ASCT) improves survival in high-risk neuroblastoma patients.
Prognosis and Survival Rates
| Risk Group | 5-Year Survival Rate |
|---|---|
| Low-Risk | >90% |
| Intermediate-Risk | 70-90% |
| High-Risk | 40-50% |
Factors affecting prognosis:
- Age at Diagnosis: Infants (<18 months) have better outcomes.
- MYCN Status: Amplification worsens prognosis.
- Metastatic Spread: Stage 4 disease has poorer survival.
Ongoing Research and Future Directions
- CAR-T Cell Therapy targeting GD2 and ALK proteins.
- Gene Editing Approaches using CRISPR to reverse oncogenic mutations.
- New Targeted Therapies inhibiting neuroblastoma-specific signaling pathways.
Neuroblastoma is a complex pediatric cancer with diverse clinical behavior. Advances in genomic profiling, targeted therapy, and immunotherapy have significantly improved outcomes, especially in high-risk patients. Early diagnosis and multidisciplinary treatment approaches remain key to achieving better survival rates and reducing long-term complications.