Nesidioblastosis is a rare pancreatic disorder characterized by the abnormal proliferation of insulin-producing beta cells, leading to persistent hyperinsulinemic hypoglycemia (PHH). This condition primarily affects newborns and infants, though cases in adults have been reported. It is closely related to congenital hyperinsulinism (CHI), a severe endocrine disorder that causes uncontrolled insulin secretion, resulting in frequent hypoglycemic episodes. Early recognition and management are critical to preventing neurological damage and long-term complications.
Causes and Pathophysiology of Nesidioblastosis
Nesidioblastosis is caused by abnormal differentiation and proliferation of pancreatic beta cells within the islets of Langerhans. These dysfunctional beta cells secrete excessive insulin, leading to hypoglycemia despite low blood glucose levels.
1. Genetic Causes
- Mutations in genes regulating insulin secretion and pancreatic development.
- Commonly associated with ABCC8 and KCNJ11 gene mutations, affecting the ATP-sensitive potassium (KATP) channels in beta cells.
- Some cases are sporadic, while others follow an autosomal recessive inheritance pattern.
2. Acquired Nesidioblastosis in Adults
- Post-gastric bypass surgery: Increased beta-cell proliferation and insulin sensitivity.
- Chronic hyperglycemia leading to reactive beta-cell hyperplasia.
- Tumor-like pancreatic cell growth (non-insulinoma PHH).
Symptoms of Nesidioblastosis
Nesidioblastosis presents with hypoglycemic symptoms, which can range from mild to severe.
1. Early Symptoms
- Irritability and excessive hunger (polyphagia).
- Sweating (diaphoresis) and tremors.
- Weakness, fatigue, and dizziness.
2. Neurological Symptoms (Due to Prolonged Hypoglycemia)
- Seizures and altered consciousness.
- Developmental delays and poor feeding in infants.
- Visual disturbances and cognitive impairment.
3. Severe Complications
- Coma due to prolonged hypoglycemia.
- Permanent neurological damage in untreated cases.
- Increased risk of sudden infant death syndrome (SIDS).
Diagnosis of Nesidioblastosis
Early diagnosis is essential for preventing irreversible complications.
1. Laboratory Tests
- Blood glucose levels – Repeated hypoglycemia (<50 mg/dL).
- Insulin levels – Inappropriately high insulin despite low blood sugar.
- C-Peptide test – Differentiates nesidioblastosis from exogenous insulin administration.
- Beta-hydroxybutyrate levels – Low in insulin-mediated hypoglycemia.
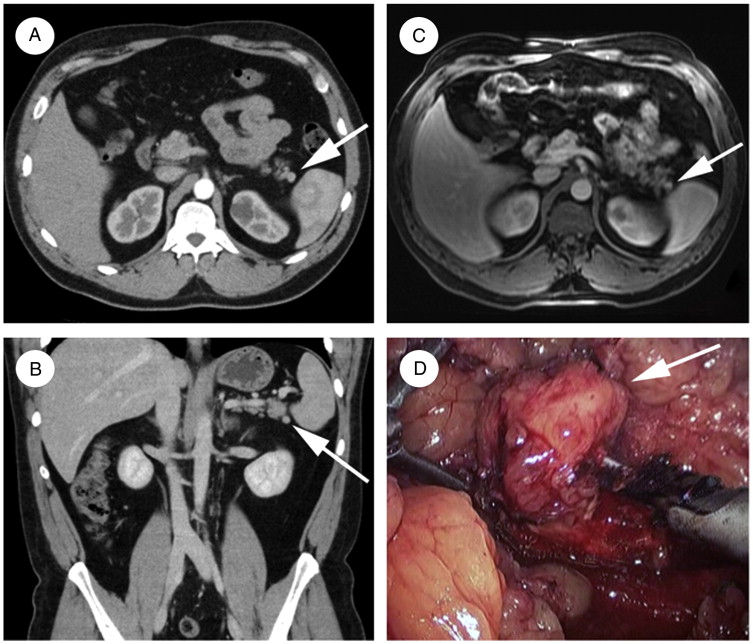
2. Imaging Studies
- Pancreatic ultrasound – May show diffuse or focal islet cell hyperplasia.
- 18F-DOPA PET scan – Identifies focal pancreatic lesions in congenital cases.
- Magnetic resonance imaging (MRI) – Used for differentiating pancreatic hyperplasia from insulinoma.
3. Pancreatic Biopsy (Definitive Diagnosis)
- Histological examination reveals beta-cell hypertrophy and nesidioblastosis.
- Helps in differentiating focal vs. diffuse nesidioblastosis, influencing treatment decisions.
Treatment Options for Nesidioblastosis
Treatment strategies focus on managing hypoglycemia and controlling excessive insulin secretion.
1. Medical Management
| Treatment | Mechanism | Indication |
|---|---|---|
| Diazoxide | Activates KATP channels, suppressing insulin release | First-line for mild cases |
| Octreotide | Somatostatin analog inhibiting insulin secretion | Used in severe cases |
| Glucagon | Raises blood glucose during hypoglycemic episodes | Emergency use |
| Hydrocortisone | Reduces insulin sensitivity | Adjunct therapy in refractory cases |
2. Nutritional Therapy
- Frequent carbohydrate-rich meals to prevent hypoglycemia.
- Continuous nasogastric or gastrostomy feeding for infants with severe forms.
- Avoiding simple sugars that trigger excessive insulin release.
3. Surgical Intervention
For medication-resistant nesidioblastosis, surgery may be required.
- Focal Nesidioblastosis: Partial pancreatectomy (removal of affected region).
- Diffuse Nesidioblastosis: Near-total pancreatectomy (up to 95% of pancreas removed).
- Post-surgical risks: Diabetes mellitus and exocrine pancreatic insufficiency.
Long-Term Prognosis and Outcomes
1. Prognosis in Infants and Children
- Early diagnosis and treatment reduce neurological damage.
- Lifelong monitoring required for metabolic complications.
2. Prognosis in Adults
- Post-bariatric surgery nesidioblastosis may resolve with dietary control.
- Some patients develop persistent hypoglycemia requiring medication.
Prevention and Risk Reduction
- Genetic screening for at-risk families.
- Close monitoring of neonates with perinatal distress.
- Regular glucose monitoring in post-gastric bypass patients.
Nesidioblastosis is a complex pancreatic disorder requiring early diagnosis and targeted management to prevent life-threatening hypoglycemia. With advances in genetic testing, imaging techniques, and medical therapies, we can improve patient outcomes and ensure better long-term health for affected individuals.