Nephrogenic diabetes insipidus (NDI) is a rare kidney disorder characterized by the inability of the kidneys to concentrate urine, leading to excessive urination (polyuria) and extreme thirst (polydipsia). Unlike central diabetes insipidus, which results from deficient antidiuretic hormone (ADH) production, NDI occurs when the kidneys do not respond properly to ADH (vasopressin). This resistance causes impaired water reabsorption, leading to chronic dehydration and electrolyte imbalances.
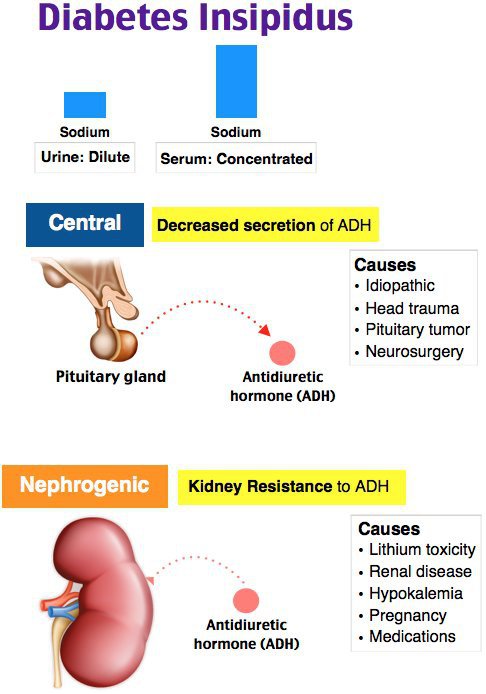
Causes and Pathophysiology of Nephrogenic Diabetes Insipidus
NDI is caused by a defect in the kidney’s ability to respond to vasopressin (antidiuretic hormone, ADH). Normally, ADH binds to receptors in the kidney’s collecting ducts, stimulating aquaporin-2 (AQP2) channels to promote water retention. However, in NDI, these mechanisms fail, resulting in excessive water loss.
Types of NDI
- Congenital Nephrogenic Diabetes Insipidus
- Caused by genetic mutations affecting vasopressin receptors or aquaporin-2 proteins.
- X-linked recessive (AVPR2 gene mutation) – Most common, affecting males.
- Autosomal recessive (AQP2 gene mutation) – Less common, affecting both genders.
- Acquired Nephrogenic Diabetes Insipidus
- More common than congenital NDI.
- Often results from prolonged use of certain medications, kidney disease, or metabolic imbalances.
Common Causes of Acquired NDI
| Cause | Mechanism | Examples |
|---|---|---|
| Lithium toxicity | Damages renal tubules | Long-term lithium therapy |
| Hypercalcemia | Reduces aquaporin function | Hyperparathyroidism |
| Hypokalemia | Impairs kidney responsiveness | Chronic diuretic use |
| Kidney disorders | Tubular dysfunction | Polycystic kidney disease |
Symptoms of Nephrogenic Diabetes Insipidus
The hallmark symptoms of NDI arise due to excessive water loss and the body’s inability to retain fluids.
Primary Symptoms
- Polyuria (excessive urination) – Can exceed 15 liters per day.
- Polydipsia (excessive thirst) – Due to severe dehydration.
- Nocturia – Frequent nighttime urination.
- Dehydration symptoms – Dry skin, low blood pressure, dizziness.
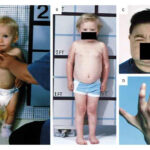
- Failure to thrive (in infants with congenital NDI) – Poor weight gain, irritability, vomiting.
Complications
- Electrolyte imbalances (low sodium, potassium abnormalities).
- Kidney damage due to chronic excessive urine production.
- Hypernatremia (elevated blood sodium levels) leading to neurological symptoms.
Diagnosis of Nephrogenic Diabetes Insipidus
Early diagnosis is crucial for preventing dehydration-related complications.
1. Clinical Assessment
- Patient history – Medication use (especially lithium), kidney disease, family history of NDI.
- Physical examination – Signs of dehydration, excessive urine output.
2. Laboratory Tests
- Urine osmolality test – Measures urine concentration (low in NDI).
- Plasma osmolality test – Elevated due to excessive water loss.
- Serum sodium levels – Often high due to dehydration.
3. Water Deprivation Test
- Evaluates the body’s ability to concentrate urine in response to water restriction.
- No improvement in urine concentration despite ADH administration confirms NDI.
4. Genetic Testing (for Congenital NDI)
- AVPR2 gene mutation (X-linked) or AQP2 gene mutation (autosomal) confirmation.
Treatment and Management of Nephrogenic Diabetes Insipidus
Currently, there is no cure for NDI, but treatment focuses on reducing symptoms, preventing dehydration, and managing electrolyte imbalances.
1. Fluid Management
- Adequate water intake to compensate for excessive urine loss.
- Low-solute diet – Reducing dietary salt and protein intake minimizes urine output.
2. Medications for NDI
| Medication | Mechanism | Usage |
|---|---|---|
| Thiazide diuretics | Reduces urine volume by inducing mild dehydration | Hydrochlorothiazide (HCTZ) |
| NSAIDs (Indomethacin) | Enhances kidney response to ADH | Adjunct therapy |
| Amiloride | Blocks lithium-induced NDI effects | For lithium users |
3. Dietary Modifications
- Low-sodium diet – Reduces urine output by decreasing kidney solute load.
- Adequate potassium intake – Essential for renal function.
4. Treatment of Underlying Causes (for Acquired NDI)
- Discontinuation of lithium if drug-induced NDI is suspected.
- Correction of hypercalcemia or hypokalemia to restore kidney function.
Long-Term Outlook and Prognosis
With early diagnosis and proper management, individuals with NDI can lead relatively normal lives. However, untreated cases may develop severe dehydration, kidney damage, and electrolyte disorders.
Key Strategies for Managing NDI
✅ Regular hydration monitoring to prevent dehydration.
✅ Frequent follow-ups with nephrologists for electrolyte balance assessments.
✅ Avoidance of dehydration triggers such as extreme heat and excessive sweating.
For congenital NDI, lifelong management is required, but advances in research, including gene therapy approaches, offer hope for future treatments.
FAQs:
Q1. How is nephrogenic diabetes insipidus different from central diabetes insipidus?
A1. NDI results from kidney resistance to ADH, while central diabetes insipidus is due to insufficient ADH production from the brain.
Q2. Can nephrogenic diabetes insipidus be cured?
A2. There is no cure for congenital NDI, but acquired NDI may be reversible if the underlying cause is treated.
Q3. How much water should a person with NDI drink daily?
A3. Fluid intake should match urine output, which can range from 3 to 15 liters per day.
Q4. Does nephrogenic diabetes insipidus affect life expectancy?
A4. If properly managed, NDI does not reduce life expectancy, but complications like severe dehydration can be life-threatening.
Q5. Can children with congenital NDI lead normal lives?
A5. With early diagnosis, proper hydration, and dietary management, children with NDI can grow and develop normally.
Nephrogenic diabetes insipidus is a rare but manageable kidney disorder that disrupts the body’s ability to retain water. Early diagnosis, hydration strategies, and medication therapy play crucial roles in preventing complications and ensuring a good quality of life for affected individuals. As medical advancements continue, newer treatment options may provide even better management solutions in the future.