Neonatal pneumonia is a serious lung infection in newborns that can occur due to bacterial, viral, or fungal pathogens. It is a leading cause of neonatal morbidity and mortality, especially in preterm and low-birth-weight infants. The condition can be classified as congenital (intrauterine), early-onset, or late-onset pneumonia, depending on the time of infection. Early identification and prompt medical intervention are crucial for reducing complications and mortality risk.
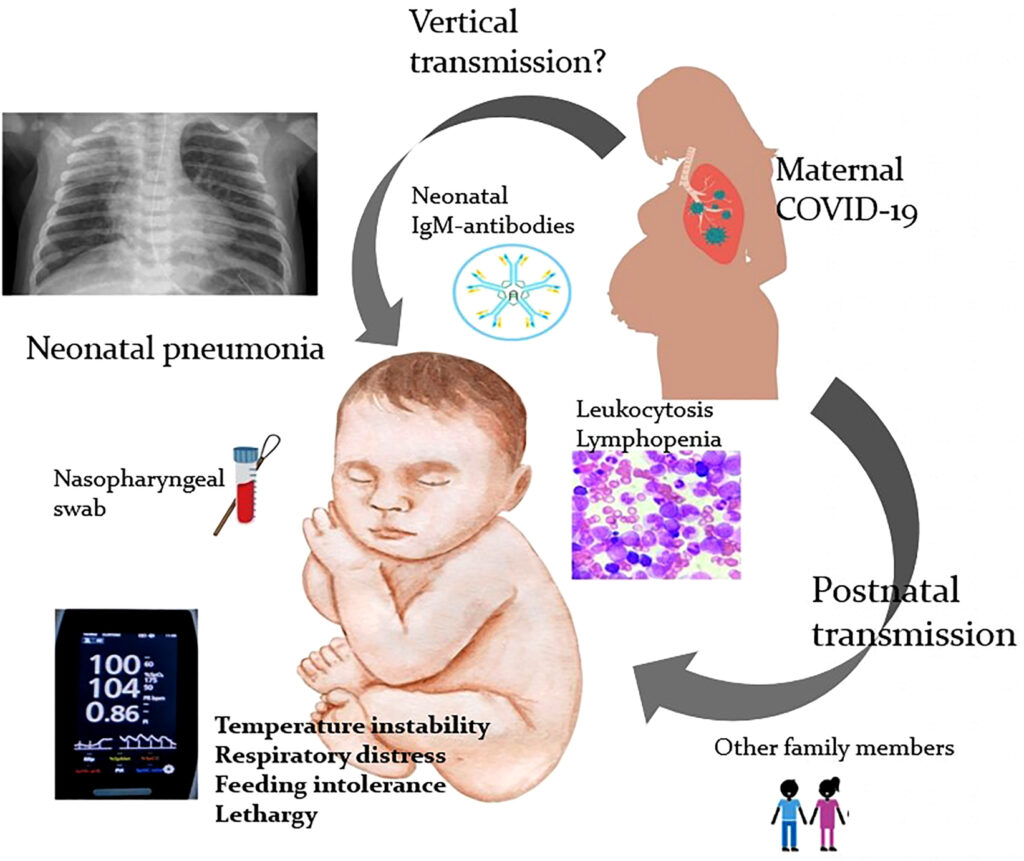
Causes of Neonatal Pneumonia
Neonatal pneumonia results from microbial infections acquired before, during, or after birth. The most common causative organisms include:
1. Bacterial Infections
- Group B Streptococcus (GBS) – Leading cause of early-onset neonatal pneumonia.
- Escherichia coli (E. coli) – Common in premature infants.
- Klebsiella pneumoniae – Affects hospital-admitted neonates.
- Staphylococcus aureus – Includes methicillin-resistant strains (MRSA).
- Listeria monocytogenes – Transmitted via the placenta or contaminated food.
2. Viral Infections
- Cytomegalovirus (CMV) – Congenital infection linked to intrauterine pneumonia.
- Herpes Simplex Virus (HSV) – Causes severe respiratory complications.
- Respiratory Syncytial Virus (RSV) – Common in community-acquired neonatal pneumonia.
3. Fungal Infections
- Candida species – Affects immunocompromised and very low birth weight infants.
Types of Neonatal Pneumonia
1. Congenital Pneumonia
- Acquired in utero due to maternal infections.
- Often caused by CMV, rubella, syphilis, or Listeria monocytogenes.
- Infants present with respiratory distress at birth.
2. Early-Onset Neonatal Pneumonia (EOP)
- Occurs within the first 48-72 hours after birth.
- Usually caused by GBS, E. coli, or Listeria.
- Associated with prolonged rupture of membranes (PROM) and maternal chorioamnionitis.
3. Late-Onset Neonatal Pneumonia (LOP)
- Develops after 3-7 days of life.
- Commonly associated with nosocomial infections, ventilator-associated pneumonia (VAP), or hospital-acquired bacterial infections.
Symptoms of Neonatal Pneumonia
Neonatal pneumonia symptoms can overlap with sepsis and respiratory distress syndrome (RDS), making diagnosis challenging.
1. Respiratory Symptoms
- Tachypnea (rapid breathing) – Over 60 breaths per minute.
- Grunting – A sign of increased respiratory effort.
- Intercostal retractions – Visible chest wall pulling due to difficulty breathing.
- Nasal flaring – Indicates respiratory distress.
- Cyanosis – Bluish skin due to poor oxygenation.
2. Systemic Symptoms
- Poor feeding or difficulty sucking.
- Lethargy and decreased activity.
- Hypothermia or fever (depends on pathogen type).
3. Severe Cases (Complications)
- Apnea (breathing cessation).
- Hypotension and shock.
- Multiorgan failure in severe sepsis cases.
Diagnosis of Neonatal Pneumonia
1. Clinical Examination
- Assessment of respiratory distress signs.
- Evaluation for risk factors (maternal infection, prolonged rupture of membranes).
2. Laboratory Investigations
- Complete Blood Count (CBC) – Elevated white blood cells indicate infection.
- C-reactive protein (CRP) – High levels suggest systemic inflammation.
- Blood culture – Identifies bacterial infection.
3. Radiological Imaging
- Chest X-ray – Shows diffuse infiltrates, consolidation, or ground-glass opacities.
- Lung ultrasound – Increasingly used for rapid bedside diagnosis.
4. Microbiological Tests
- Tracheal aspirate culture (in ventilated infants).
- Polymerase chain reaction (PCR) – Identifies viral and bacterial pathogens.
Treatment of Neonatal Pneumonia
1. Supportive Care
- Oxygen therapy – For infants with respiratory distress or hypoxemia.
- Fluid management – Prevents dehydration and electrolyte imbalance.
- Mechanical ventilation – Required for severe respiratory failure.
2. Antibiotic Therapy (Bacterial Pneumonia)
| Antibiotic | Pathogen | Duration |
|---|---|---|
| Ampicillin + Gentamicin | GBS, E. coli | 7-10 days |
| Cefotaxime | Severe cases or gram-negative bacteria | 10-14 days |
| Vancomycin | MRSA or resistant infections | 10-14 days |
3. Antiviral and Antifungal Therapy
- Acyclovir – For HSV pneumonia.
- Ganciclovir – For CMV-related congenital pneumonia.
- Fluconazole – For Candida pneumonia in immunocompromised neonates.
Complications of Neonatal Pneumonia
- Neonatal sepsis – Can progress to septic shock and organ failure.
- Bronchopulmonary dysplasia (BPD) – Long-term lung disease.
- Pneumothorax – Air leakage into the chest cavity.
- Persistent pulmonary hypertension of the newborn (PPHN) – Severe complication leading to hypoxia.
Prevention of Neonatal Pneumonia
1. Maternal Preventive Measures
- Routine prenatal screening for GBS (administer intrapartum antibiotics if positive).
- Timely treatment of maternal infections (chorioamnionitis, UTIs).
- Sterile delivery practices to prevent early-onset infections.
2. Neonatal Preventive Strategies
- Strict hand hygiene in NICU settings.
- Early feeding with breast milk to boost immune defense.
- Reducing unnecessary ventilator use to prevent ventilator-associated pneumonia (VAP).
Long-Term Outlook and Prognosis
The prognosis of neonatal pneumonia depends on infection severity, gestational age, and timely treatment. While most newborns recover with early intervention, premature infants remain at higher risk for chronic lung disease and developmental delays. Long-term follow-up with pulmonary and neurological assessments is essential for at-risk infants.
Neonatal pneumonia is a life-threatening respiratory infection requiring prompt recognition, accurate diagnosis, and aggressive treatment. By implementing preventive maternal care, early neonatal screening, and evidence-based treatment protocols, we can significantly reduce neonatal mortality and improve outcomes for affected newborns.