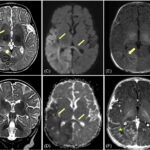
Neonatal hypocalcemic tetany is a calcium metabolism disorder that affects newborns, leading to neuromuscular excitability, muscle spasms, and seizures. It occurs due to low ionized calcium levels in the blood, disrupting normal nerve and muscle function. The condition is often associated with parathyroid hormone (PTH) deficiency, vitamin D deficiency, or maternal metabolic disorders. Early diagnosis and management are crucial to prevent complications and long-term neurological deficits.

Pathophysiology of Neonatal Hypocalcemic Tetany
Calcium plays a critical role in neuromuscular transmission, bone mineralization, and enzymatic functions. The parathyroid glands regulate calcium homeostasis through parathyroid hormone (PTH), vitamin D metabolism, and renal calcium reabsorption.
In neonates, hypocalcemia can occur due to:
- Impaired parathyroid function (congenital hypoparathyroidism).
- Vitamin D deficiency (maternal or neonatal).
- Maternal conditions affecting calcium transfer.
- Impaired renal calcium reabsorption.
Causes and Risk Factors
Neonatal hypocalcemia can be classified into early-onset (first 72 hours of life) and late-onset (after 3–7 days of life) hypocalcemia.
1. Early-Onset Hypocalcemia (First 72 Hours of Life)
- Maternal Diabetes Mellitus – Increased fetal insulin secretion inhibits calcium transport.
- Prematurity – Immature parathyroid response and inadequate calcium stores.
- Birth Asphyxia – Impaired placental calcium transfer.
- Intrauterine Growth Restriction (IUGR) – Insufficient calcium deposition in fetal bones.
- Perinatal Hypoxia – Alters calcium metabolism, leading to neonatal hypocalcemia.
2. Late-Onset Hypocalcemia (After 3–7 Days of Life)
- Hypoparathyroidism (Congenital or Acquired) – Reduced PTH secretion leading to hypocalcemia.
- Vitamin D Deficiency or Insufficiency – Low 25-hydroxyvitamin D impairs calcium absorption.
- High Phosphate Intake (Formula Feeding) – Excess phosphate leads to hypocalcemia.
- DiGeorge Syndrome (22q11.2 Deletion Syndrome) – Congenital absence or dysfunction of parathyroid glands.
- Maternal Hypocalcemia or Hyperparathyroidism – Affects fetal calcium balance post-birth.
Clinical Presentation of Neonatal Hypocalcemic Tetany
Neuromuscular Symptoms
- Muscle spasms and rigidity.
- Tetany (involuntary muscle contractions).
- Laryngospasm (stridor, respiratory distress).
- Seizures (focal or generalized).
- Jitteriness and irritability.
Autonomic and Cardiac Symptoms
- Bradycardia (slow heart rate).
- Prolonged QT interval on ECG (risk of arrhythmias).
- Cyanosis or apnea due to laryngospasm.
Additional Features in Syndromic Causes
- DiGeorge Syndrome – Facial dysmorphism, congenital heart defects, immunodeficiency.
- Maternal Diabetes-Related Hypocalcemia – Macrosomia, respiratory distress.
Diagnosis of Neonatal Hypocalcemic Tetany
1. Serum Calcium Levels
- Total calcium < 7 mg/dL (normal: 8.5–10.5 mg/dL).
- Ionized calcium < 1.1 mmol/L (normal: 1.1–1.3 mmol/L).
2. Parathyroid Hormone (PTH) and Vitamin D Levels
- Low PTH in hypoparathyroidism.
- Low 25-hydroxyvitamin D in vitamin D deficiency.
3. Serum Phosphate and Magnesium Levels
- Hyperphosphatemia in late-onset hypocalcemia.
- Hypomagnesemia in associated electrolyte imbalances.
4. Electrocardiogram (ECG) Findings
- Prolonged QT interval, risk of arrhythmias.
5. Genetic and Imaging Studies
- FISH (Fluorescence In Situ Hybridization) for 22q11.2 deletion (DiGeorge Syndrome).
- Neck ultrasound or MRI to assess parathyroid gland presence in congenital cases.
Treatment of Neonatal Hypocalcemic Tetany
1. Acute Management of Severe Hypocalcemia
- Intravenous (IV) Calcium Gluconate (10%)
- Dose: 100–200 mg/kg slow IV infusion over 10–20 minutes.
- Continuous ECG monitoring to prevent cardiac arrhythmias.
- Magnesium Supplementation (if hypomagnesemia is present).
2. Maintenance Therapy for Chronic Hypocalcemia
- Oral Calcium Supplementation
- Calcium carbonate 50–75 mg/kg/day in divided doses.
- Vitamin D Therapy
- Calcitriol (Active Vitamin D, 0.05–0.2 mcg/kg/day) for PTH deficiency.
- Cholecalciferol (Vitamin D3, 400–800 IU/day) for nutritional deficiency.
3. Long-Term Monitoring and Follow-Up
- Serum calcium and phosphate levels to assess treatment efficacy.
- Cardiac monitoring for prolonged QT syndrome in high-risk infants.
- Developmental screening for neurological sequelae.
Prevention of Neonatal Hypocalcemia
1. Maternal Nutrition and Supplementation
- Vitamin D supplementation during pregnancy (600–2000 IU/day).
- Calcium-rich diet to prevent maternal hypocalcemia.
2. Neonatal Screening and Early Intervention
- Routine serum calcium checks in high-risk neonates (preterm, IUGR, maternal diabetes).
- Avoiding high-phosphate formula feeding in at-risk newborns.
3. Management of Syndromic Causes
- Early genetic testing and PTH monitoring in infants with congenital anomalies.
- Multidisciplinary care for infants with DiGeorge Syndrome or severe hypoparathyroidism.
Prognosis and Long-Term Outcomes
- Early treatment reduces neurological complications and prevents seizures.
- Untreated severe hypocalcemia can lead to intellectual disability, epilepsy, and cardiac complications.
- Most cases resolve with appropriate supplementation, but lifelong monitoring is required in congenital hypoparathyroidism.
Neonatal hypocalcemic tetany is a critical metabolic disorder that requires prompt recognition and intervention. Early calcium and vitamin D supplementation, maternal screening, and neonatal monitoring are essential in preventing complications. Multidisciplinary care, including pediatric endocrinologists, neonatologists, and cardiologists, ensures optimal management of affected infants.