Neonatal herpes meningoencephalitis is a life-threatening central nervous system (CNS) infection caused by the herpes simplex virus (HSV), primarily HSV-2 and, less commonly, HSV-1. It affects newborns during or shortly after birth, leading to severe neurological damage and high mortality rates if untreated. Despite advances in antiviral therapy, early diagnosis and intervention remain critical in reducing morbidity.
Pathogenesis and Transmission of Neonatal HSV Infection
Neonatal herpes infection occurs through vertical transmission from a mother with an active or asymptomatic HSV infection.
- Intrauterine Transmission (Congenital HSV) – Rare, accounting for less than 5% of cases. It occurs via transplacental transmission, leading to congenital malformations, microcephaly, or intrauterine growth restriction (IUGR).
- Peripartum Transmission (During Delivery) – The most common route (85% of cases), occurring when a newborn passes through an infected birth canal.
- Postnatal Transmission – Accounts for 10% of cases, primarily from caregivers with active HSV lesions through direct contact.
Types of Neonatal HSV Infection
1. Skin, Eye, and Mouth (SEM) Disease
- Localized form affecting the skin, eyes, and oral mucosa.
- Presents with vesicular lesions, conjunctivitis, and ulcerations.
- Least severe form, but progression to CNS infection is possible.
2. Neonatal Herpes Meningoencephalitis (CNS Involvement)
- Most severe and life-threatening form of neonatal herpes.
- Affects the brain and spinal cord, leading to seizures, lethargy, and respiratory distress.
- High risk of neurological complications, including cerebral palsy, intellectual disability, and epilepsy.
3. Disseminated Neonatal Herpes
- Widespread viral infection involving multiple organs (lungs, liver, adrenal glands, CNS).
- Causes septic-like shock, jaundice, respiratory distress, and coagulation abnormalities.
- High mortality rate (up to 80%) if untreated.
Risk Factors for Neonatal Herpes Meningoencephalitis
- Primary maternal HSV infection during pregnancy (highest transmission risk).
- Maternal genital HSV shedding during labor.
- Premature rupture of membranes (PROM) >6 hours.
- Preterm birth (<37 weeks gestation).
- Use of invasive fetal monitoring (scalp electrodes, forceps delivery).
- Immunocompromised neonates.
Symptoms and Clinical Manifestations
Early Symptoms (First 1-2 Weeks of Life)
- Poor feeding, irritability, fever, lethargy.
- Vesicular skin rash (may be absent in CNS and disseminated cases).
- Hypothermia or fever (temperature instability).
Neurological Symptoms (CNS Disease Progression)
- Seizures (focal or generalized).
- Hypotonia (floppy baby syndrome) or hypertonia (rigid posturing).
- Apnea (breathing difficulties).
- Bulging fontanelle (increased intracranial pressure).
- Lethargy, poor suck reflex, abnormal eye movements.
Severe Disseminated Disease Symptoms
- Respiratory distress, tachypnea, cyanosis.
- Hepatic dysfunction (jaundice, elevated liver enzymes).
- Coagulopathy (petechiae, purpura, disseminated intravascular coagulation – DIC).
- Multiorgan failure in severe cases.
Diagnosis of Neonatal Herpes Meningoencephalitis
1. Lumbar Puncture (CSF Analysis for HSV Meningoencephalitis)
- PCR testing for HSV DNA (Gold Standard).
- CSF findings: pleocytosis, elevated protein, low glucose.
2. HSV Polymerase Chain Reaction (PCR) Testing
- Blood, CSF, or vesicle swabs confirm HSV DNA presence.
- High sensitivity and specificity for early detection.
3. Electroencephalography (EEG) for Neurological Assessment
- Identifies epileptiform activity, focal slowing, or burst suppression patterns in HSV encephalitis.
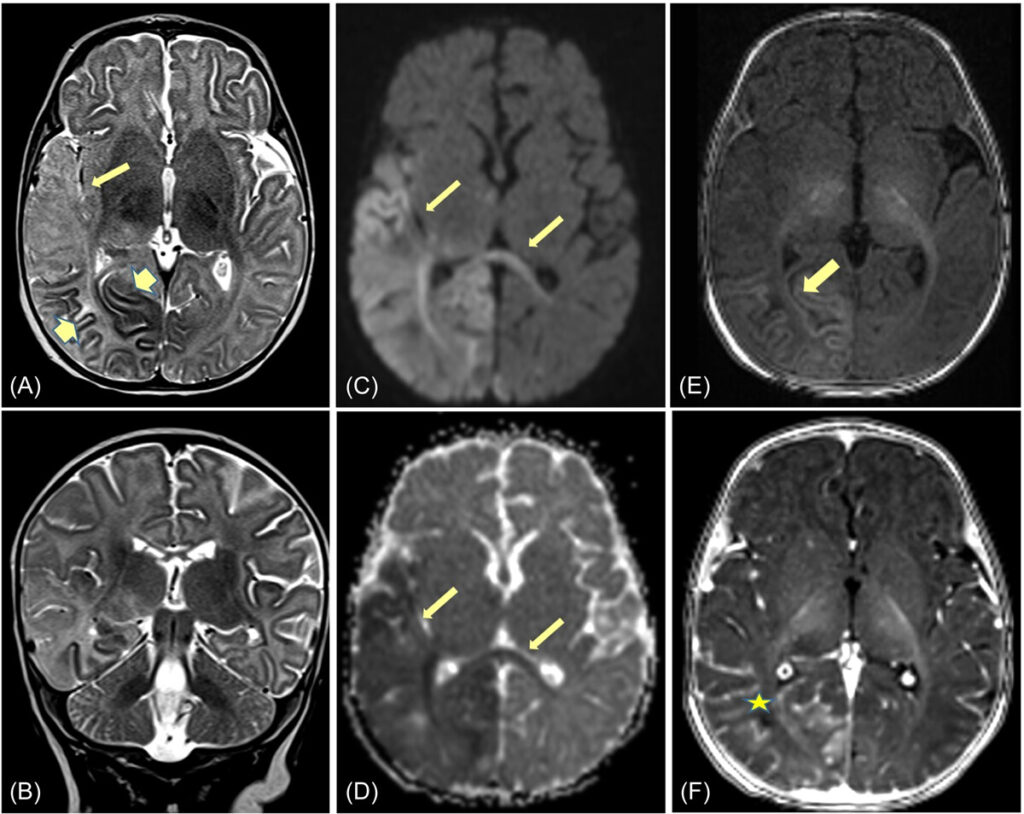
4. Magnetic Resonance Imaging (MRI) of the Brain
- Reveals temporal lobe abnormalities, edema, and necrotic changes.
- Helps distinguish HSV encephalitis from other neonatal infections.
Treatment of Neonatal Herpes Meningoencephalitis
1. Antiviral Therapy (Gold Standard: IV Acyclovir)
- Neonatal CNS or disseminated disease:
- Acyclovir 20 mg/kg IV every 8 hours for 21 days.
- SEM disease:
- Acyclovir 20 mg/kg IV every 8 hours for 14 days.
2. Supportive NICU Management
- Seizure control – Phenobarbital or levetiracetam.
- Mechanical ventilation for respiratory failure.
- Intravenous fluids and electrolyte management.
- Blood transfusions in case of coagulopathy.
3. Long-Term Oral Acyclovir Suppression
- 6-month suppressive therapy (Acyclovir 300 mg/m² PO three times daily) reduces neurological impairment risk.
Prevention Strategies for Neonatal HSV Infection
1. Maternal HSV Screening and Risk Reduction
- Routine HSV serologic testing in pregnant women with recurrent genital herpes.
- Antiviral suppression therapy (Acyclovir or Valacyclovir from 36 weeks gestation) reduces perinatal transmission.
2. Delivery Considerations
- Cesarean section (C-section) is recommended for women with active genital HSV lesions at labor onset.
- Avoid fetal scalp electrodes and invasive monitoring in HSV-positive mothers.
3. Postnatal Infection Prevention
- Strict hand hygiene for caregivers with HSV lesions.
- Isolate neonates with suspected HSV to prevent nosocomial spread.
Prognosis and Long-Term Outcomes
- Early antiviral treatment improves survival rates, but long-term neurological sequelae are common.
- CNS involvement (meningoencephalitis) increases the risk of developmental delays, seizures, and motor dysfunction.
- Disseminated neonatal herpes has a high mortality rate (up to 60% even with treatment).
Neonatal herpes meningoencephalitis is a devastating CNS infection requiring rapid diagnosis and aggressive antiviral therapy. Maternal screening, antiviral suppression, and delivery precautions play a crucial role in prevention. Despite treatment advances, neurological impairment remains a significant concern, emphasizing the need for early intervention and long-term follow-up in affected neonates.