Neonatal Group B Streptococcal (GBS) septicemia is a severe bacterial infection affecting newborns, leading to sepsis, pneumonia, and meningitis. GBS, caused by Streptococcus agalactiae, is a leading cause of early-onset and late-onset neonatal infections, with transmission occurring vertically from the mother during childbirth or postnatally from caregivers. Despite routine prenatal screening and intrapartum antibiotic prophylaxis (IAP), GBS infections remain a major contributor to neonatal morbidity and mortality.
Pathophysiology of GBS Septicemia
GBS infection in neonates follows a progressive invasion of the bloodstream, leading to systemic inflammatory response and organ dysfunction.
- Colonization – GBS colonizes the maternal vaginal and rectal flora without causing symptoms.
- Vertical Transmission – During labor, neonates can aspirate infected amniotic fluid or acquire GBS during vaginal delivery.
- Bacteremia and Dissemination – The bacteria enter the bloodstream, triggering immune activation.
- Systemic Sepsis – Uncontrolled bacterial growth leads to shock, organ failure, and potential death.
Types of Neonatal GBS Infection
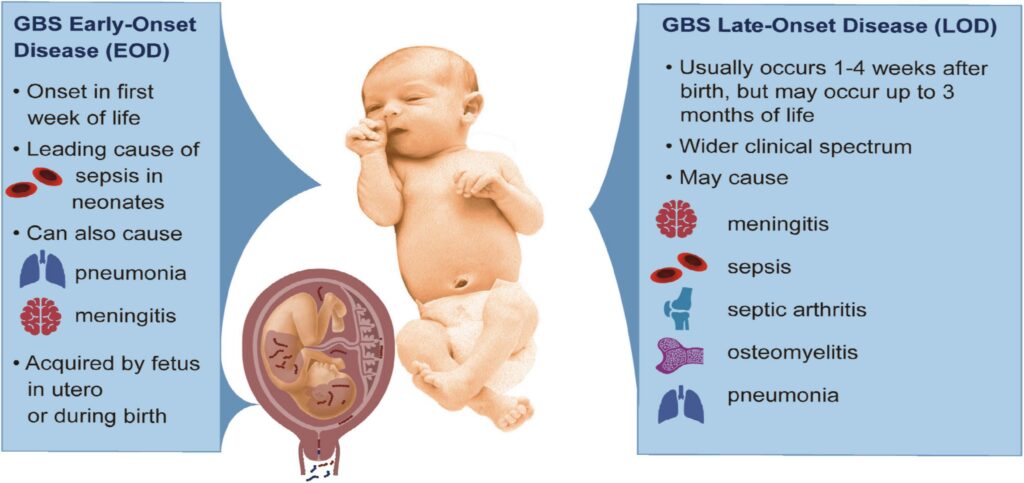
1. Early-Onset GBS Disease (EOGBS)
- Occurs within the first 7 days of life (usually within 24-48 hours).
- Source: Vertical transmission during delivery.
- Clinical Manifestations:
- Sepsis (most common form, 80%)
- Pneumonia (respiratory distress, grunting, tachypnea)
- Meningitis (bulging fontanelle, lethargy, seizures in severe cases)
2. Late-Onset GBS Disease (LOGBS)
- Occurs between 7 days and 3 months of age.
- Source: Postnatal acquisition from caregivers or hospital environments.
- Clinical Manifestations:
- Bacteremia without focus (most common)
- Meningitis (more frequent than in early-onset cases, leading to neurological complications)
- Septic arthritis and osteomyelitis
Risk Factors for Neonatal GBS Infection
Maternal Risk Factors
- GBS colonization in pregnancy (rectovaginal swab positive at 35-37 weeks gestation)
- Premature rupture of membranes (PROM) >18 hours
- Preterm labor (<37 weeks gestation)
- Fever during labor (>38°C)
- Previous infant with GBS disease
- Chorioamnionitis (intra-amniotic infection)
Neonatal Risk Factors
- Prematurity (underdeveloped immune response)
- Low birth weight (<2500g)
- Immune deficiencies
Symptoms and Clinical Presentation
1. General Sepsis Symptoms
- Temperature instability (hypothermia or fever)
- Lethargy, poor feeding, weak cry
- Irritability, difficulty breathing (grunting, flaring, retractions)
- Pallor or cyanosis (blue skin discoloration)
- Tachycardia or bradycardia, hypotension
2. Respiratory Distress Syndrome (EOGBS)
- Grunting respirations
- Intercostal retractions
- Cyanosis (bluish skin due to low oxygen levels)
- Tachypnea (>60 breaths per minute)
3. Meningitis Symptoms (More Common in LOGBS)
- Bulging fontanelle (soft spot swelling in newborns)
- Seizures, stiff neck, high-pitched cry
- Hypotonia (floppy baby syndrome)
Diagnosis of Neonatal GBS Septicemia
1. Blood Culture (Gold Standard)
- Confirms GBS bacteremia in suspected neonates.
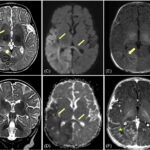
2. Lumbar Puncture (CSF Analysis for Meningitis)
- Elevated white blood cells (WBCs), low glucose, and high protein indicate infection.
3. Complete Blood Count (CBC)
- Elevated C-reactive protein (CRP) and procalcitonin suggest systemic infection.
4. Chest X-ray (For Pneumonia Cases)
- Reveals diffuse infiltrates or lobar consolidation in GBS pneumonia.
Treatment of Neonatal GBS Septicemia
1. Empirical Antibiotic Therapy
- Ampicillin + Gentamicin (first-line treatment for suspected cases).
- Penicillin G is preferred after confirmed diagnosis.
- Cefotaxime may be used in meningitis cases (avoiding ceftriaxone in neonates).
2. Supportive NICU Management
- Mechanical ventilation for respiratory distress.
- Intravenous fluids and vasopressors for septic shock.
- Anticonvulsants for GBS meningitis-related seizures.
Prevention Strategies for GBS Infection
1. Universal Maternal GBS Screening
- 35-37 weeks gestation: Rectovaginal swab culture for GBS detection.
2. Intrapartum Antibiotic Prophylaxis (IAP)
- Indicated for:
- GBS-positive mothers
- Previous GBS-infected newborn
- Preterm labor with unknown GBS status
- PROM >18 hours
| Recommended IAP Regimen | Drug | Dosage |
|---|---|---|
| First-line | Penicillin G | 5 million units IV, then 2.5-3 million units IV every 4 hours until delivery |
| Alternative (Penicillin allergy) | Cefazolin | 2g IV, then 1g IV every 8 hours |
| High-risk allergy alternative | Clindamycin or Vancomycin | Clindamycin 900 mg IV every 8 hours (if susceptible); Vancomycin 20 mg/kg IV every 12 hours |
3. Neonatal Post-Exposure Monitoring
- Asymptomatic neonates with GBS-positive mothers receive 48 hours of observation.
- Symptomatic neonates require immediate workup and antibiotic therapy.
Prognosis and Long-Term Outcomes
- Survival rates are high with early treatment, but untreated GBS septicemia can lead to fatal outcomes.
- Neurological complications (cerebral palsy, developmental delays) occur in severe GBS meningitis cases.
- Hearing loss risk due to GBS-related meningitis.
Neonatal Group B Streptococcal septicemia is a life-threatening bacterial infection requiring early recognition, aggressive antibiotic therapy, and maternal screening programs for prevention. Advances in intrapartum antibiotic prophylaxis (IAP) have significantly reduced early-onset GBS infections, but vigilance remains crucial for late-onset disease. With prompt NICU intervention, most affected neonates recover fully, though long-term follow-up is essential for high-risk cases.