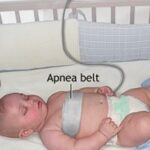
Neonatal alloimmune thrombocytopenia (NAIT) is a rare but serious condition in which maternal antibodies attack fetal platelets, leading to severe thrombocytopenia (low platelet count) in the newborn. This immune response occurs due to incompatibility between maternal and fetal human platelet antigens (HPA), similar to Rh incompatibility in hemolytic disease of the newborn. NAIT increases the risk of intracranial hemorrhage (ICH), life-threatening bleeding, and long-term neurological complications.
Early diagnosis and treatment are critical for improving neonatal outcomes. Understanding NAIT’s pathophysiology, risk factors, and management strategies is essential for healthcare professionals and expectant parents.
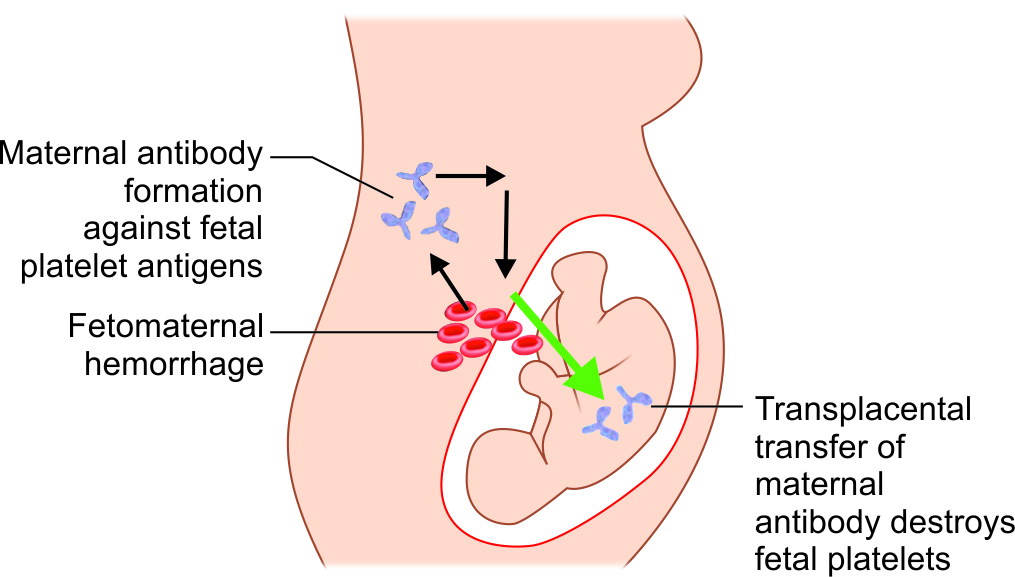
Causes and Pathophysiology of NAIT
1. Maternal-Fetal Platelet Incompatibility
NAIT occurs when a mother who lacks a specific platelet antigen produces antibodies against fetal platelets that express the antigen inherited from the father. The most common incompatibility involves:
- HPA-1a (most frequent cause, accounting for 75-80% of cases)
- HPA-5b, HPA-3a, and other rare HPAs
These antibodies cross the placenta, bind to fetal platelets, and cause immune-mediated destruction, leading to thrombocytopenia.
2. Risk Factors for NAIT
- First pregnancy (can still be affected, but higher risk in subsequent pregnancies due to immune sensitization)
- Paternal antigen positivity (HPA-1a most common)
- Maternal alloimmunization history
- Family history of neonatal bleeding disorders
Symptoms and Clinical Manifestations
NAIT symptoms vary depending on platelet count severity and may appear at birth or within the first few days of life.
1. Common Symptoms
- Petechiae and purpura (small red or purple spots on the skin)
- Ecchymosis (bruising) without trauma
- Mucosal bleeding (nosebleeds, oral bleeding)
- Hematomas (localized blood collections under the skin)
2. Severe Complications
- Intracranial hemorrhage (ICH) – occurs in 10-20% of severe cases, leading to long-term neurological damage
- Gastrointestinal or pulmonary hemorrhage
- Severe anemia due to blood loss
Diagnosis of Neonatal Alloimmune Thrombocytopenia
1. Laboratory Tests for the Newborn
- Complete blood count (CBC): Reveals low platelet count (<50,000/µL in severe cases)
- Peripheral blood smear: No abnormal platelet morphology, ruling out other causes
- Platelet antibody testing: Detects maternal anti-HPA antibodies
2. Maternal and Paternal Testing
- HPA genotyping: Identifies maternal HPA-negative status and paternal antigen compatibility
- Antibody screening: Confirms maternal anti-HPA antibody presence
3. Differential Diagnosis
NAIT must be distinguished from other neonatal thrombocytopenic conditions, including:
| Condition | Key Differentiating Factor |
|---|---|
| Congenital infections (TORCH) | Other systemic symptoms (e.g., hepatosplenomegaly) |
| Autoimmune thrombocytopenia (ITP) | Maternal platelet count is also low |
| Disseminated intravascular coagulation (DIC) | Coagulation abnormalities present |
Treatment of Neonatal Alloimmune Thrombocytopenia
1. Immediate Management for Affected Newborns
- Intravenous Immunoglobulin (IVIG) – First-line therapy, reduces platelet destruction
- Platelet transfusion – Preferably HPA-matched platelets from maternal donors or antigen-negative donors
- Corticosteroids (in severe cases) – Reduces antibody-mediated destruction
2. Treatment in Severe Cases (ICH or Life-Threatening Bleeding)
- Urgent platelet transfusion with HPA-compatible or washed maternal platelets
- Neurosurgical intervention if needed for ICH management
Prevention and Management in Future Pregnancies
1. Prenatal Monitoring for At-Risk Pregnancies
For mothers with a previous history of NAIT or confirmed alloimmunization:
- HPA genotyping of the father to confirm fetal risk
- Serial fetal ultrasound to monitor for intracranial hemorrhage
- Fetal blood sampling (cordocentesis) in severe cases
2. Preventive Treatments During Pregnancy
- IVIG Therapy (from 20-24 weeks gestation) – Reduces maternal antibody effects
- Corticosteroids (adjunctive therapy) – Helps suppress immune response
- Planned early delivery (C-section at 37-38 weeks) – Reduces risk of birth trauma-related bleeding
Long-Term Prognosis and Follow-Up
1. Recovery and Neurological Outcomes
- Mild cases: Spontaneous platelet recovery within 2-3 weeks postpartum
- Severe cases (ICH or major bleeding): Higher risk of cerebral palsy, developmental delays, or epilepsy
2. Follow-Up Care Recommendations
- Neurological assessments for infants with ICH history
- Platelet monitoring until stable counts are reached
- Genetic counseling for future pregnancies
Neonatal alloimmune thrombocytopenia is a life-threatening but manageable disorder that requires early diagnosis, prompt treatment, and preventive measures in future pregnancies. Advances in maternal screening, IVIG therapy, and targeted platelet transfusions have significantly improved neonatal outcomes. Expecting mothers with a history of NAIT should undergo genetic counseling and specialized prenatal care to minimize recurrence risks.