Necrotizing pneumonia (NP) is a rare but severe complication of bacterial pneumonia characterized by extensive lung tissue necrosis, abscess formation, and cavitary lesions. It is associated with high morbidity and requires prompt diagnosis and aggressive treatment to prevent respiratory failure and sepsis. The condition is most commonly caused by Streptococcus pneumoniae, Staphylococcus aureus, and Klebsiella pneumoniae, though other bacterial and fungal pathogens may contribute.
Causes and Risk Factors
1. Common Causative Pathogens
Necrotizing pneumonia is most often associated with the following bacterial infections:
- Streptococcus pneumoniae – The leading cause of bacterial pneumonia.
- Staphylococcus aureus (including MRSA) – Produces toxins that accelerate lung tissue destruction.
- Klebsiella pneumoniae – A common pathogen in hospital-acquired pneumonia.
- Pseudomonas aeruginosa – Frequently affects immunocompromised patients.
- Anaerobic bacteria – Often seen in aspiration pneumonia cases.
2. Risk Factors for Necrotizing Pneumonia
- Weakened immune system (HIV, chemotherapy, organ transplant recipients)
- Chronic lung diseases (COPD, cystic fibrosis, bronchiectasis)
- Previous bacterial pneumonia or respiratory infections
- Aspiration of oropharyngeal secretions (due to stroke, alcoholism, or neurological disorders)
- Hospital-acquired infections and prolonged mechanical ventilation
Symptoms of Necrotizing Pneumonia
Patients with necrotizing pneumonia often exhibit severe respiratory symptoms along with systemic signs of infection.
Early Symptoms
- Persistent high fever and chills
- Severe cough with purulent, foul-smelling sputum
- Chest pain (pleuritic pain worsening with breathing)
- Dyspnea (shortness of breath)
Advanced Symptoms
- Hemoptysis (coughing up blood)
- Cyanosis (bluish discoloration due to lack of oxygen)
- Respiratory distress requiring oxygen therapy or ventilation
- Altered mental status in severe cases due to hypoxia and sepsis
Diagnosis of Necrotizing Pneumonia
Early detection is critical to prevent lung destruction and systemic complications.
1. Imaging Studies
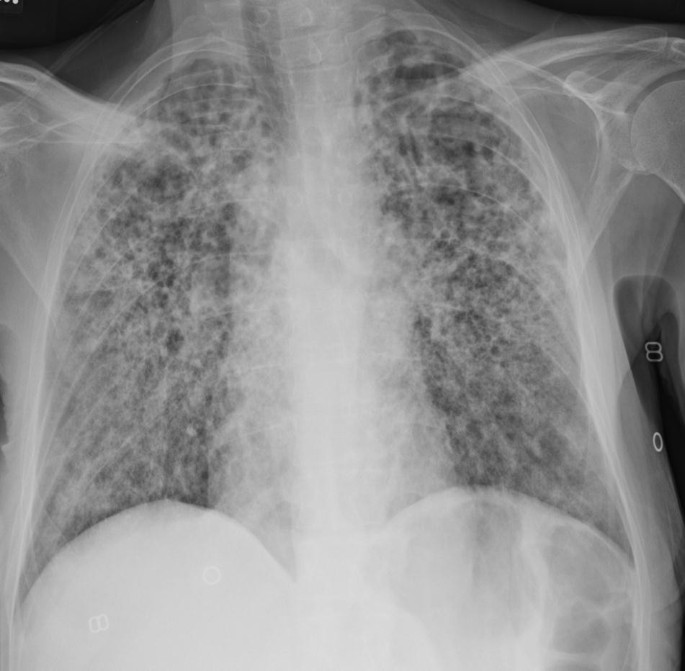
- Chest X-ray – Reveals patchy lung consolidation and cavitary lesions.
- CT scan of the chest – Provides detailed imaging of necrotic areas and abscess formation.
2. Laboratory Tests
- Complete Blood Count (CBC) – Shows elevated white blood cells.
- Inflammatory markers (CRP, ESR, Procalcitonin) – Help assess infection severity.
- Blood and sputum cultures – Identify causative bacteria and guide antibiotic therapy.
3. Bronchoscopy and Lung Biopsy
- In cases of diagnostic uncertainty, bronchoscopy helps obtain lung tissue samples for bacterial analysis.
Treatment of Necrotizing Pneumonia
Management of necrotizing pneumonia involves aggressive medical and, in some cases, surgical intervention.
1. Broad-Spectrum Antibiotics
Initial treatment includes intravenous broad-spectrum antibiotics targeted at common pathogens.
- Beta-lactams + Clindamycin (for Streptococcus pneumoniae)
- Vancomycin or Linezolid (for Methicillin-resistant Staphylococcus aureus [MRSA])
- Carbapenems (for Klebsiella pneumoniae or multidrug-resistant bacteria)
2. Oxygen Therapy and Ventilation Support
Patients with severe respiratory distress may require:
- High-flow oxygen therapy
- Non-invasive ventilation (BiPAP/CPAP)
- Mechanical ventilation in cases of respiratory failure
3. Surgical Interventions
Surgery is considered for patients with extensive lung damage.
- Percutaneous drainage – For large lung abscesses.
- Lobectomy or Pneumonectomy – In cases of non-resolving necrosis and cavitation.
4. Supportive Care
- IV fluids and nutritional support
- Pain management with opioids or NSAIDs
- Pulmonary rehabilitation and physiotherapy
Complications of Necrotizing Pneumonia
If left untreated, necrotizing pneumonia can lead to life-threatening complications.
1. Respiratory Failure
Severe lung tissue destruction reduces oxygen exchange, necessitating ventilatory support.
2. Sepsis and Septic Shock
Bacterial invasion into the bloodstream leads to systemic inflammatory response and multi-organ failure.
3. Lung Abscesses and Empyema
Necrotic lung tissue may result in abscesses or pus accumulation in the pleural cavity.
4. Bronchopleural Fistula
Destruction of lung tissue can create abnormal connections between the bronchial tree and pleural cavity, leading to persistent air leaks.
Prevention of Necrotizing Pneumonia
Preventive measures focus on reducing bacterial pneumonia risk and maintaining lung health.
1. Vaccination
- Pneumococcal vaccine (PCV13, PPSV23) – Reduces Streptococcus pneumoniae infections.
- Influenza vaccine – Prevents secondary bacterial pneumonia after flu infection.
2. Early Treatment of Pneumonia
Prompt antibiotic therapy for bacterial pneumonia reduces the risk of necrotizing complications.
3. Good Respiratory Hygiene
- Regular handwashing and avoiding exposure to infectious respiratory droplets.
- Wearing masks in high-risk healthcare settings.
4. Managing Underlying Conditions
- Smoking cessation to improve lung function.
- Control of diabetes and chronic diseases to enhance immune defense.
Necrotizing pneumonia is a life-threatening pulmonary condition requiring immediate medical attention. Characterized by extensive lung necrosis, abscess formation, and cavitary destruction, it primarily results from bacterial infections such as Streptococcus pneumoniae and Staphylococcus aureus. Early diagnosis through imaging and laboratory tests, coupled with aggressive antibiotic therapy and supportive care, is crucial in improving patient outcomes. Preventative measures, including vaccination and early pneumonia treatment, play a vital role in reducing the incidence of this severe respiratory infection.