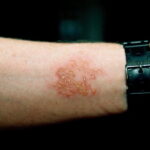
Necrobiosis Lipoidica Diabeticorum (NLD) is a chronic, inflammatory skin condition primarily associated with diabetes mellitus. It manifests as yellowish, atrophic plaques, typically on the lower legs. While the exact cause remains unclear, NLD is linked to microvascular complications in diabetic patients. This article explores the causes, symptoms, diagnostic approaches, and treatment options for NLD.
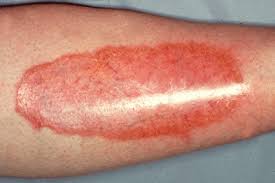
What is Necrobiosis Lipoidica Diabeticorum?
NLD is a rare skin disorder that affects approximately 0.3% of individuals with diabetes. The condition is characterized by degenerative changes in collagen and blood vessels, leading to distinctive skin lesions. Although it predominantly occurs in diabetic patients, NLD can also develop in non-diabetic individuals.
Causes and Risk Factors
The precise cause of NLD remains unknown, but several factors contribute to its development:
- Diabetes Mellitus: NLD is most commonly associated with type 1 diabetes but can also occur in type 2 diabetes.
- Microangiopathy: Damage to small blood vessels impairs blood flow, leading to skin necrosis and inflammation.
- Immune System Dysregulation: Autoimmune reactions may trigger inflammatory processes in the skin.
- Genetic Predisposition: A family history of diabetes or skin disorders may increase susceptibility.
- Trauma: Minor injuries to the skin can exacerbate lesion formation in individuals with NLD.
Symptoms of NLD
NLD presents as distinctive skin lesions that evolve over time. Common symptoms include:
- Reddish or Yellowish Patches: Early lesions appear as small, red papules that gradually develop into atrophic plaques with a yellow center.
- Shiny, Thin Skin: Affected areas become glossy and thin, making them prone to ulceration.
- Pain and Itching: Some patients experience discomfort, tenderness, or itching, particularly in ulcerated lesions.
- Location: Lesions typically occur on the shins but may also appear on the forearms, face, or scalp in rare cases.
Diagnosis of Necrobiosis Lipoidica Diabeticorum
Diagnosis is based on clinical evaluation, patient history, and, if necessary, histopathological examination.
- Physical Examination: Dermatologists assess the characteristic appearance of NLD lesions.
- Skin Biopsy: A biopsy may be performed to confirm the diagnosis and rule out similar conditions, such as diabetic dermopathy or granuloma annulare.
- Blood Tests: Evaluating blood glucose levels helps identify underlying diabetes or assess glycemic control in diabetic patients.
Differential Diagnosis
Several skin conditions mimic NLD, making differential diagnosis crucial:
- Diabetic Dermopathy: Presents as small, brown patches but lacks the atrophic and ulcerative features of NLD.
- Granuloma Annulare: Circular, reddish plaques without the yellowish, atrophic center of NLD.
- Sarcoidosis: Non-caseating granulomas that may resemble NLD lesions.
- Lichen Planus: Purple, itchy papules that differ in morphology from NLD plaques.
Treatment Options for NLD
There is no definitive cure for NLD, but treatment aims to manage symptoms and prevent complications.
Medical Treatments
- Topical Corticosteroids: Reduce inflammation and slow lesion progression.
- Intralesional Steroid Injections: Used for localized treatment of active lesions.
- Calcineurin Inhibitors (Tacrolimus, Pimecrolimus): Help control inflammation in steroid-resistant cases.
- Aspirin and Pentoxifylline: Improve microcirculation and prevent vascular complications.
- Immunomodulators (TNF-alpha inhibitors): Considered for severe or refractory cases.
Lifestyle and Home Care
- Blood Sugar Control: Maintaining optimal glycemic levels can slow disease progression.
- Moisturization: Keeping the skin hydrated reduces discomfort and risk of ulceration.
- Avoiding Trauma: Preventing injuries to affected areas minimizes lesion aggravation.
- Compression Therapy: May improve circulation and reduce symptoms.
Surgical and Advanced Treatments
- Laser Therapy: Fractional CO2 lasers and pulsed-dye lasers can improve the appearance of NLD lesions.
- Skin Grafts: Used in severe ulcerated cases to promote healing.
- Biologic Therapy: Emerging treatments targeting inflammatory pathways are under investigation.
Prognosis and Complications
NLD is a chronic condition that may persist for years, with periods of flare-ups and remission. While some lesions remain stable, others may ulcerate, leading to secondary infections. Rarely, NLD can progress to squamous cell carcinoma, necessitating long-term dermatological monitoring.
Prevention Strategies
Although NLD cannot always be prevented, the following measures may reduce the risk of development or progression:
- Strict Diabetes Management: Keeping blood glucose levels within target ranges.
- Protecting Skin from Injury: Wearing protective clothing and avoiding trauma to vulnerable areas.
- Regular Dermatological Check-ups: Early intervention helps prevent complications.
- Smoking Cessation: Tobacco use exacerbates microvascular damage and worsens NLD.
Necrobiosis Lipoidica Diabeticorum is a challenging dermatological condition closely linked to diabetes. While there is no definitive cure, early diagnosis and comprehensive management strategies can significantly improve quality of life. Individuals with diabetes should prioritize glycemic control and skin care to reduce the risk of NLD and associated complications.