Myocardial reinfarction refers to the recurrence of a heart attack in patients who have previously experienced myocardial infarction (MI). Preventing reinfarction is critical to reducing mortality, minimizing cardiac damage, and improving long-term survival. Effective strategies involve a combination of pharmacological therapy, lifestyle modifications, and medical interventions.
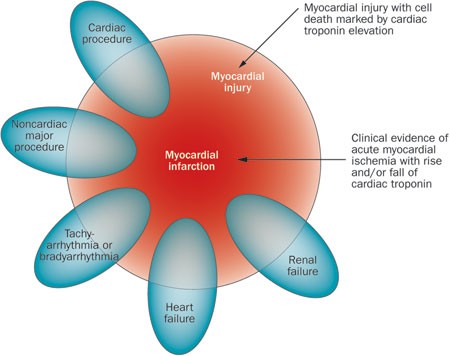
Risk Factors for Myocardial Reinfarction
Identifying and managing risk factors is essential to preventing another heart attack. Key risk factors include:
- Uncontrolled Hypertension: Increased blood pressure puts stress on the heart, increasing the risk of reinfarction.
- Hyperlipidemia: Elevated LDL cholesterol contributes to plaque buildup in coronary arteries.
- Diabetes Mellitus: High blood sugar damages blood vessels, accelerating atherosclerosis.
- Smoking: A major modifiable risk factor that significantly increases cardiovascular disease risk.
- Obesity and Sedentary Lifestyle: Lack of physical activity and excess weight contribute to metabolic syndrome.
- Psychosocial Stress: Chronic stress and depression negatively impact cardiovascular health.
Pharmacological Strategies for Prevention
1. Antiplatelet and Anticoagulant Therapy
- Aspirin: A cornerstone in secondary prevention, reducing platelet aggregation and clot formation.
- P2Y12 Inhibitors (Clopidogrel, Ticagrelor, Prasugrel): Recommended for patients post-stent placement or those at high thrombotic risk.
- Anticoagulants (Warfarin, DOACs): Used selectively in patients with atrial fibrillation or high clotting risk.
2. Lipid-Lowering Therapy
- Statins (Atorvastatin, Rosuvastatin): Lower LDL cholesterol and stabilize plaque, reducing reinfarction risk.
- PCSK9 Inhibitors: An option for patients with statin intolerance or extremely high cholesterol levels.
3. Beta-Blockers and ACE Inhibitors
- Beta-Blockers (Metoprolol, Carvedilol): Reduce heart rate and myocardial oxygen demand.
- ACE Inhibitors/ARBs (Lisinopril, Losartan): Improve cardiac function and lower blood pressure.
4. Diabetes and Hypertension Management
- SGLT2 Inhibitors and GLP-1 Agonists: Shown to provide cardiovascular benefits in diabetic patients.
- Calcium Channel Blockers and Diuretics: Used in resistant hypertension cases.
Lifestyle Modifications for Long-Term Prevention
1. Dietary Changes
- Heart-Healthy Diet: Emphasizing whole grains, lean proteins, fruits, vegetables, and healthy fats.
- Reduced Sodium and Processed Foods: Helps in blood pressure control.
- Omega-3 Fatty Acids: Found in fish and flaxseeds, beneficial for cardiovascular health.
2. Regular Physical Activity
- Aerobic Exercises: Walking, cycling, and swimming improve cardiac endurance.
- Strength Training: Enhances metabolism and muscle health.
- Supervised Cardiac Rehabilitation: Essential for post-MI recovery and reinfarction prevention.
3. Smoking Cessation and Alcohol Moderation
- Quitting Smoking: Drastically reduces cardiovascular risk.
- Limiting Alcohol: Excessive alcohol consumption contributes to hypertension and arrhythmias.
4. Stress Management and Mental Health Care
- Mindfulness, Meditation, and Yoga: Effective in reducing stress levels.
- Psychological Support: Therapy or support groups for post-MI anxiety and depression.
Interventional and Surgical Approaches
1. Coronary Revascularization
- Percutaneous Coronary Intervention (PCI): Stent placement to restore blood flow.
- Coronary Artery Bypass Grafting (CABG): Recommended for multi-vessel disease cases.
2. Implantable Cardiac Devices
- ICDs and Pacemakers: Used in patients with arrhythmia risks post-MI.
Importance of Regular Follow-Up and Monitoring
Routine cardiovascular check-ups, medication adherence, and lifestyle consistency are crucial in preventing myocardial reinfarction. Patients should actively engage with healthcare providers to optimize their risk management strategies.
Preventing myocardial reinfarction requires a multifaceted approach involving medications, lifestyle changes, and, when necessary, medical interventions. By addressing modifiable risk factors and adhering to evidence-based therapies, patients can significantly reduce their chances of experiencing another heart attack and improve their overall cardiovascular health.