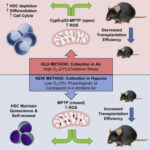
Myeloid engraftment enhancement plays a crucial role in autologous peripheral blood progenitor cell transplantation (PBPC transplant), directly impacting hematopoietic recovery, infection risk, and overall patient outcomes. Effective engraftment ensures rapid restoration of myeloid lineage cells, particularly neutrophils and monocytes, which are vital for immune function. This article explores key strategies, biological mechanisms, and clinical approaches to improve myeloid engraftment post-transplantation.
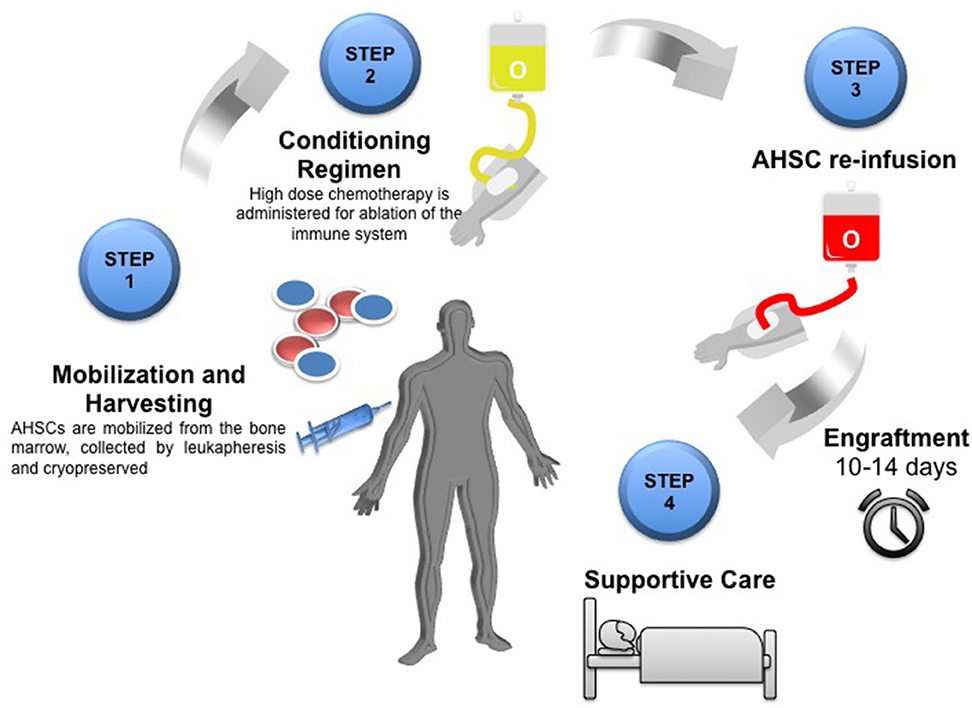
Understanding Myeloid Engraftment in PBPC Transplantation
What Is Myeloid Engraftment?
Myeloid engraftment refers to the successful integration and proliferation of hematopoietic stem cells (HSCs) in the bone marrow following transplantation. It is typically assessed when the absolute neutrophil count (ANC) reaches ≥500/µL for three consecutive days.
Key Factors Affecting Myeloid Engraftment
1. Stem Cell Dose and Quality
- Higher doses of CD34+ hematopoietic progenitor cells accelerate engraftment.
- Stem cell viability and functionality impact engraftment efficiency.
2. Mobilization Strategies
- Granulocyte Colony-Stimulating Factor (G-CSF) is the primary agent used to mobilize progenitor cells.
- Plerixafor (CXCR4 antagonist) enhances mobilization in poor mobilizers.
3. Bone Marrow Microenvironment
- Stromal cell interactions influence stem cell homing and proliferation.
- Cytokine-rich environments improve engraftment efficiency.
4. Post-Transplant Supportive Care
- Growth factor administration (G-CSF, GM-CSF) speeds up neutrophil recovery.
- Optimized antimicrobial prophylaxis reduces post-transplant complications.
Strategies for Enhancing Myeloid Engraftment
1. Stem Cell Optimization Approaches
- Higher CD34+ Cell Infusion: Ensures faster neutrophil and platelet recovery.
- Ex Vivo Expansion: Enhances progenitor cell numbers before reinfusion.
- Cryopreservation Techniques: Reducing stem cell damage improves post-thaw viability.
2. Pharmacological Enhancements
- G-CSF and GM-CSF Administration: Promotes faster neutrophil recovery.
- Thrombopoietin (TPO) Agonists: Enhance platelet engraftment alongside myeloid restoration.
- Erythropoietin (EPO): Supports early red blood cell recovery.
3. Microenvironment Modulation
- Mesenchymal Stem Cell (MSC) Co-Infusion: Enhances hematopoietic niche support.
- Cytokine-Based Therapy: IL-6 and IL-3 improve early myeloid proliferation.
4. Novel Gene and Cellular Therapies
- Gene-Edited HSCs: Enhancing engraftment through targeted modifications.
- Immune Modulation via Treg Cells: Prevents excessive inflammation and supports hematopoiesis.
Clinical Outcomes and Challenges
| Enhancement Strategy | Advantages | Challenges |
|---|---|---|
| High CD34+ Cell Dose | Faster neutrophil recovery | Risk of graft-related complications |
| G-CSF Administration | Reduced infection risk | Potential cytokine-related toxicity |
| MSC Co-Infusion | Supports hematopoietic niche | Limited availability |
| Ex Vivo Expansion | Higher stem cell yield | Cost and technical limitations |
Future Directions in Myeloid Engraftment Enhancement
Emerging advancements, including biomaterial-based scaffolds, artificial bone marrow niches, and personalized genetic modifications, are poised to revolutionize post-transplant engraftment strategies. Further research in stem cell engineering, immunotherapy integration, and cytokine optimization will enhance outcomes in PBPC transplantation.
Enhancing myeloid engraftment after autologous peripheral blood progenitor cell transplantation is critical for optimizing patient recovery. Strategies such as stem cell dose optimization, pharmacological support, and microenvironment engineering continue to evolve, improving transplant success rates.