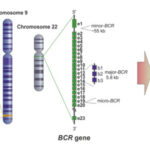
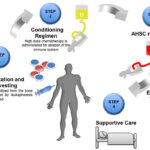
Myeloid engraftment enhancement is a critical factor in hematopoietic stem cell transplantation (HSCT), influencing the speed and success of bone marrow recovery. Efficient engraftment reduces post-transplant complications such as graft failure, delayed immune reconstitution, and infections. Various biological, clinical, and therapeutic interventions have been developed to enhance myeloid engraftment, improving patient outcomes in allogeneic and autologous transplantation.
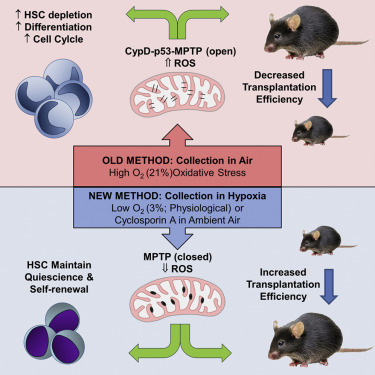
Understanding Myeloid Engraftment
Myeloid engraftment refers to the process by which donor-derived myeloid cells (granulocytes, monocytes, and macrophages) establish and proliferate in the recipient’s bone marrow after transplantation. It is a crucial milestone in hematopoietic recovery, typically measured by absolute neutrophil count (ANC) ≥ 500/µL for three consecutive days.
Factors Influencing Engraftment Success
- Stem Cell Source – Peripheral blood stem cells (PBSCs) engraft faster than bone marrow-derived cells.
- Donor HLA Matching – Better HLA matching improves graft acceptance.
- Conditioning Regimen – Myeloablative conditioning enhances marrow receptivity.
- Graft Composition – Higher CD34+ cell dose correlates with faster myeloid recovery.
- Microenvironmental Factors – Bone marrow niche integrity and cytokine availability affect engraftment.
Strategies to Enhance Myeloid Engraftment
1. Optimization of Hematopoietic Stem Cell Grafts
- Higher CD34+ Cell Dose – Increased stem cell numbers accelerate neutrophil and platelet recovery.
- Ex Vivo Expansion Techniques – Enhancing stem cell proliferation before transplantation improves graft efficacy.
- Umbilical Cord Blood Enhancements – Techniques like co-infusion with haploidentical stem cells improve cord blood engraftment.
2. Cytokine and Growth Factor Support
- Granulocyte Colony-Stimulating Factor (G-CSF) – Mobilizes stem cells and accelerates neutrophil recovery.
- Stem Cell Factor (SCF) – Enhances hematopoietic progenitor cell expansion.
- Interleukin-3 (IL-3) – Promotes early myeloid differentiation.
3. Graft Manipulation Techniques
- T-Cell Depletion Strategies – Reducing alloreactive T-cells mitigates graft-versus-host disease (GVHD) and improves engraftment kinetics.
- Mesenchymal Stem Cell (MSC) Co-Infusion – Supports hematopoietic stem cell engraftment by modifying the bone marrow niche.
- Ex Vivo Gene Editing – Enhancing stem cell survival and proliferation through CRISPR-based modifications.
4. Conditioning Regimen Modifications
- Reduced-Intensity Conditioning (RIC) – Improves engraftment in older or high-risk patients.
- Radiation-Free Conditioning – Uses targeted immunotherapy to create a receptive marrow environment without excessive toxicity.
Clinical Outcomes and Challenges
| Engraftment Strategy | Benefits | Challenges |
|---|---|---|
| High CD34+ Cell Dose | Faster neutrophil recovery | Increased risk of chronic GVHD |
| G-CSF Mobilization | Shortens neutropenia duration | Potential cytokine storm |
| MSC Co-Infusion | Reduces graft failure | Limited donor sources |
| Ex Vivo Expansion | Enhances stem cell numbers | Cost and regulatory hurdles |
Future Perspectives in Myeloid Engraftment Enhancement
Emerging research focuses on gene-modified stem cells, bioengineered grafts, and immunomodulatory therapies to further enhance myeloid engraftment. Artificial bone marrow scaffolds and bioprinted microenvironments represent potential innovations in post-transplant recovery.
Enhancing myeloid engraftment is pivotal for improving hematopoietic stem cell transplant success. Advances in graft manipulation, cytokine therapy, and microenvironment engineering continue to shape the future of transplant medicine, reducing complications and improving survival rates.