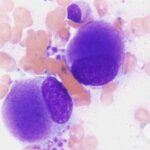
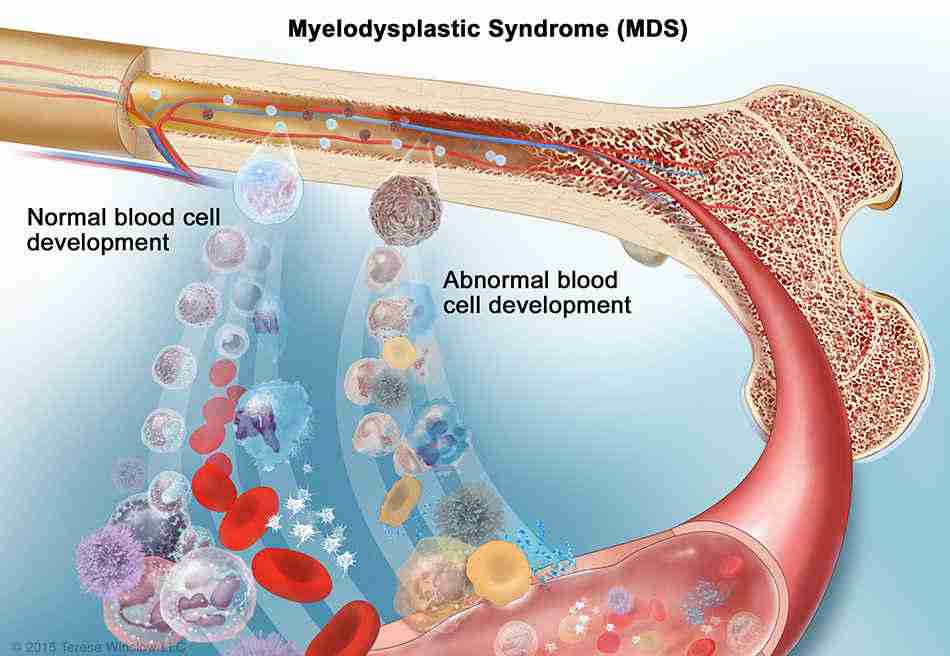
Myelodysplastic syndrome (MDS) is a group of hematologic disorders characterized by ineffective blood cell production due to bone marrow dysfunction. This leads to cytopenias, increasing the risk of anemia, infections, and bleeding complications. MDS can progress to acute myeloid leukemia (AML) in some cases, making early detection and appropriate treatment essential.
Causes and Risk Factors of Myelodysplastic Syndrome
MDS is caused by genetic mutations that impair the normal development of hematopoietic stem cells in the bone marrow. While the exact cause is unknown, several risk factors contribute to its development:
- Age – Most commonly diagnosed in individuals over 60.
- Previous chemotherapy or radiation therapy – Exposure to alkylating agents and topoisomerase inhibitors increases risk.
- Environmental exposure – Long-term contact with benzene, pesticides, and heavy metals is associated with MDS.
- Genetic predisposition – Some inherited conditions, such as Fanconi anemia, increase susceptibility.
- Smoking – Toxins in cigarettes can damage bone marrow cells.
Pathophysiology of Myelodysplastic Syndrome
MDS affects the bone marrow’s ability to produce healthy blood cells. The abnormal function of hematopoietic stem cells leads to dysplastic (abnormal) cells, apoptosis (cell death), and ineffective hematopoiesis.
Symptoms of Myelodysplastic Syndrome
Symptoms vary depending on the severity of cytopenias:
- Anemia (Low Red Blood Cells) – Fatigue, pallor, shortness of breath.
- Leukopenia (Low White Blood Cells) – Increased susceptibility to infections.
- Thrombocytopenia (Low Platelets) – Easy bruising, prolonged bleeding, petechiae.
- General Symptoms – Unexplained weight loss, fever, night sweats.
Diagnosis of Myelodysplastic Syndrome
Diagnosing MDS requires a combination of blood tests, bone marrow examination, and genetic analysis.
1. Complete Blood Count (CBC) and Peripheral Blood Smear
- Shows cytopenias and dysplastic cells.
- Mean corpuscular volume (MCV) may be elevated.
2. Bone Marrow Biopsy and Aspirate
- Reveals hypercellular or hypocellular bone marrow with dysplasia.
- Increased blast cells suggest a higher risk of progression to AML.
3. Cytogenetic and Molecular Testing
- Karyotyping and Fluorescence In Situ Hybridization (FISH) detect chromosomal abnormalities.
- Common mutations: TP53, SF3B1, TET2, ASXL1.
4. Risk Stratification: Revised International Prognostic Scoring System (IPSS-R)
MDS is classified based on:
- Cytogenetic abnormalities
- Percentage of blasts in bone marrow
- Degree of cytopenias
IPSS-R Risk Groups:
- Very Low to Low Risk – Slow disease progression.
- Intermediate to Very High Risk – Higher chance of developing AML.
Treatment Options for Myelodysplastic Syndrome
Treatment is based on the risk category and patient’s overall health.
1. Supportive Care
- Red blood cell transfusions for anemia.
- Platelet transfusions for bleeding risk.
- Erythropoiesis-stimulating agents (ESAs) like epoetin alfa boost red blood cell production.
- Iron chelation therapy prevents iron overload from frequent transfusions.
2. Disease-Modifying Therapies
- Hypomethylating agents (HMAs) – Azacitidine and Decitabine delay progression to AML.
- Immunosuppressive therapy – Antithymocyte globulin (ATG) benefits younger patients with hypoplastic MDS.
- Lenalidomide – Effective in del(5q) MDS, improving red blood cell production.
3. Hematopoietic Stem Cell Transplantation (HSCT)
- The only curative treatment for MDS.
- Best suited for younger patients with high-risk MDS.
Prognosis and Life Expectancy in Myelodysplastic Syndrome
MDS prognosis depends on risk stratification and response to treatment.
| IPSS-R Risk Group | Median Survival | Risk of AML Progression |
|---|---|---|
| Very Low | 8+ years | <5% |
| Low | 5-6 years | 10% |
| Intermediate | 3 years | 30% |
| High | 1.5 years | 54% |
| Very High | <1 year | 84% |
Factors influencing prognosis:
- Younger age and good performance status improve survival.
- Complex cytogenetic abnormalities indicate poorer outcomes.
- HSCT offers long-term remission but carries procedural risks.
Myelodysplastic syndrome is a complex bone marrow disorder requiring early diagnosis and personalized treatment. While supportive care can improve quality of life, disease-modifying therapies and stem cell transplantation offer potential long-term benefits. Advances in genetic research and targeted therapies continue to improve outcomes for MDS patients.