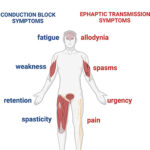
Muscle spasticity of cerebral origin is a condition characterized by involuntary muscle stiffness and exaggerated reflexes due to damage in the central nervous system (CNS). It commonly affects individuals with cerebral palsy, stroke, traumatic brain injury, and other neurological disorders. This article explores the underlying causes, symptoms, and available treatment options to improve mobility and quality of life.
What Is Muscle Spasticity of Cerebral Origin?
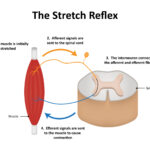
Muscle spasticity results from hyperactive stretch reflexes caused by damage to the brain’s motor pathways. It leads to increased muscle tone (hypertonia), involuntary contractions, and resistance to movement. Unlike temporary muscle stiffness, spasticity is a persistent neurological condition that affects motor control and daily activities.
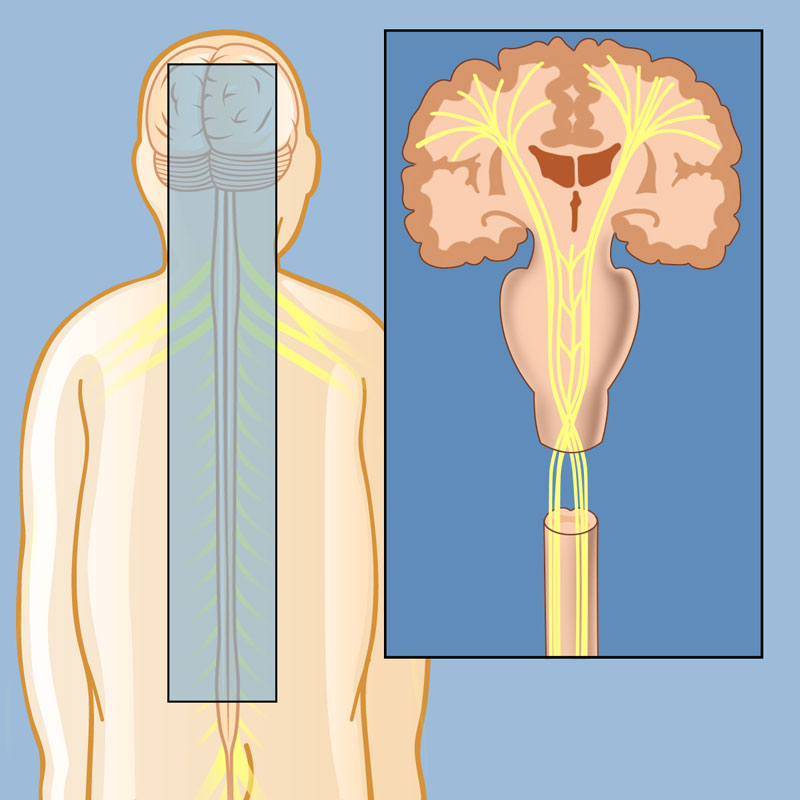
Role of the Central Nervous System in Spasticity
The central nervous system regulates voluntary and involuntary muscle movements. When a neurological injury disrupts motor pathways, the balance between excitatory and inhibitory signals is lost, causing continuous muscle contractions and spasticity.
Causes of Muscle Spasticity of Cerebral Origin
Muscle spasticity arises from conditions that affect the brain’s ability to control voluntary movements. The most common causes include:
1. Cerebral Palsy (CP)
Cerebral palsy is a group of movement disorders caused by early brain damage, often before or shortly after birth. Spastic CP, the most prevalent type, leads to muscle tightness and difficulty with coordination.
2. Stroke
A stroke occurs when blood flow to the brain is interrupted, causing cell damage in motor control areas. Post-stroke spasticity affects limbs, leading to stiffness, muscle spasms, and reduced function.
3. Traumatic Brain Injury (TBI)
Severe head injuries can damage neural pathways, impairing muscle control and causing spasticity. The severity of symptoms depends on the extent and location of brain trauma.
4. Multiple Sclerosis (MS)
MS is an autoimmune disorder that affects the myelin sheath, disrupting nerve communication. This leads to muscle spasticity, weakness, and mobility issues.
5. Hypoxic-Ischemic Encephalopathy (HIE)
A lack of oxygen to the brain, particularly in newborns, can cause spasticity and motor dysfunction, contributing to cerebral palsy or other neurological impairments.
Symptoms of Muscle Spasticity
The severity of spasticity varies based on the extent of brain damage. Common symptoms include:
1. Increased Muscle Tone (Hypertonia)
Muscles remain abnormally tight, leading to stiffness and limited range of motion.
2. Involuntary Muscle Contractions
Spasms occur unexpectedly, often triggered by movement or touch.
3. Exaggerated Reflexes (Hyperreflexia)
The body’s normal reflex responses become overly sensitive, leading to uncontrolled jerking movements.
4. Pain and Discomfort
Prolonged muscle contractions can cause significant pain and interfere with daily activities.
5. Joint Deformities and Contractures
Long-term spasticity can result in joint deformities, where muscles and tendons shorten and restrict movement.
Diagnosis of Muscle Spasticity
A thorough neurological assessment is essential for diagnosing spasticity. The evaluation includes:
- Clinical Examination: Assessing muscle tone, reflexes, and movement limitations.
- Modified Ashworth Scale (MAS): A grading system to measure spasticity severity.
- Electromyography (EMG): Identifying abnormal muscle activity.
- MRI or CT Scan: Detecting brain lesions, stroke damage, or other neurological abnormalities.
Treatment Options for Muscle Spasticity
Effective spasticity management requires a combination of medical, therapeutic, and surgical interventions. Treatment goals focus on reducing muscle stiffness, improving mobility, and enhancing daily functioning.
1. Medications for Spasticity Management
Several drugs help alleviate spasticity by targeting neural pathways:
- Baclofen: A muscle relaxant that reduces spasticity by acting on the spinal cord.
- Tizanidine: Blocks nerve signals to decrease muscle tightness.
- Diazepam (Valium): A benzodiazepine that provides short-term spasticity relief.
- Dantrolene Sodium: Reduces muscle contractions at the cellular level.
- Botulinum Toxin (Botox) Injections: Temporarily weakens overactive muscles, reducing spasticity for several months.
2. Physical Therapy and Rehabilitation
Physical therapy is crucial for maintaining muscle function and preventing contractures:
- Stretching Exercises: Improve flexibility and prevent joint stiffness.
- Strength Training: Helps counteract muscle weakness caused by spasticity.
- Splints and Orthotics: Support joints and prevent deformities.
3. Occupational Therapy
Occupational therapists teach adaptive techniques to enhance independence in daily tasks such as dressing and mobility.
4. Surgical Interventions
For severe spasticity, surgical treatments may be necessary:
- Selective Dorsal Rhizotomy (SDR): Cutting specific nerve roots in the spinal cord to reduce spasticity.
- Tendon Release Surgery: Lengthening tight tendons to improve movement.
- Intrathecal Baclofen Pump (ITB): A device implanted under the skin delivers baclofen directly to the spinal fluid, providing continuous spasticity relief.
5. Alternative and Assistive Therapies
Additional approaches include:
- Aquatic Therapy: Water-based exercises to relax muscles.
- Electrical Stimulation: Neuromuscular electrical stimulation (NMES) strengthens weak muscles.
- Acupuncture: May help improve muscle relaxation.
Lifestyle and Home Care Strategies
Patients and caregivers can implement lifestyle modifications to manage spasticity effectively:
- Consistent Stretching Routine: Regular stretching reduces muscle stiffness.
- Proper Posture and Positioning: Avoiding prolonged sitting or lying in the same position prevents contractures.
- Hydration and Nutrition: Adequate hydration supports muscle function, while balanced nutrition prevents weight-related complications.
Prognosis and Long-Term Outlook
The prognosis of muscle spasticity of cerebral origin depends on the underlying cause and treatment response. Early intervention, personalized therapy, and ongoing management significantly improve mobility, reduce discomfort, and enhance independence. By combining medical treatments with rehabilitation strategies, individuals with spasticity can achieve greater functional outcomes and a better quality of life.