Multifocal Atrial Tachycardia (MAT) is a rare yet clinically significant cardiac arrhythmia characterized by multiple ectopic foci within the atria generating electrical impulses. It is commonly seen in patients with underlying pulmonary disease and is associated with significant morbidity if left untreated. Unlike atrial fibrillation, MAT features distinct P waves with varying morphologies, reflecting multiple active pacemaker sites.
Causes and Risk Factors
MAT is frequently secondary to underlying medical conditions rather than a primary cardiac disorder. The most common causes include:
- Chronic obstructive pulmonary disease (COPD) – The leading cause of MAT, due to hypoxia-induced atrial irritability.
- Congestive heart failure (CHF) – Increased atrial pressure and stretch contribute to arrhythmia.
- Electrolyte imbalances – Low potassium (hypokalemia) and magnesium (hypomagnesemia) can precipitate MAT.
- Sepsis and systemic illness – Increased sympathetic activity triggers arrhythmogenic foci.
- Beta-agonist therapy (e.g., albuterol, salbutamol) – Commonly used in COPD patients, contributing to enhanced atrial automaticity.
- Post-surgical states – Especially after cardiac or thoracic surgery.
- Theophylline toxicity – Used for COPD and asthma management, excessive levels increase arrhythmic risk.
Symptoms of Multifocal Atrial Tachycardia
Patients with MAT often experience symptoms related to both the tachyarrhythmia and the underlying disease:
- Palpitations – Irregular and rapid heartbeat sensation.
- Shortness of breath (Dyspnea) – Often exacerbated by concurrent lung disease.
- Chest discomfort – Not typical of ischemia but may be present due to rapid heart rate.
- Fatigue and dizziness – Due to reduced cardiac efficiency.
- Syncope (rare) – Seen in severe cases with hemodynamic instability.
Diagnosis of Multifocal Atrial Tachycardia
The definitive diagnosis of MAT is made via electrocardiography (ECG) and is supported by clinical history.
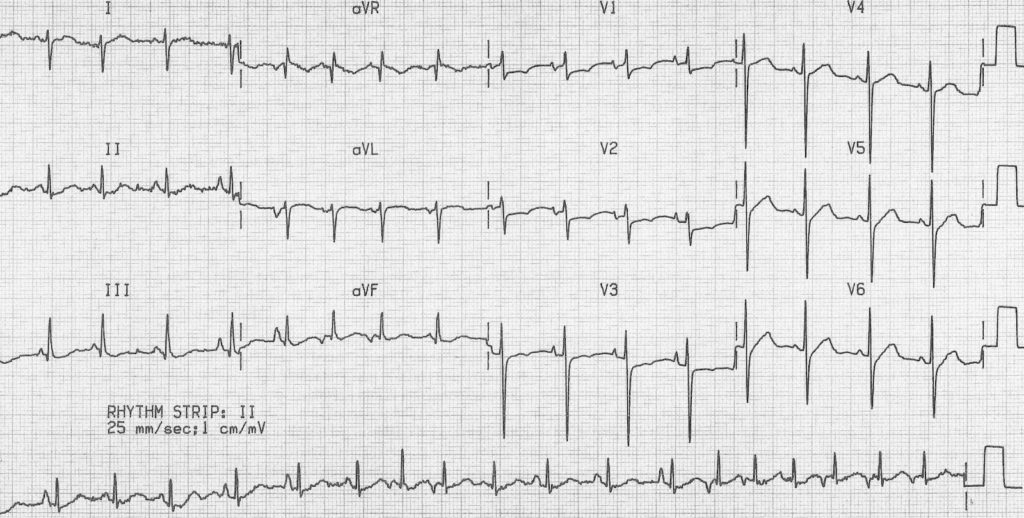
1. ECG Characteristics
- Heart rate: 100–250 beats per minute.
- Irregular rhythm with changing P-wave morphologies (≥3 distinct shapes).
- Variable PR intervals and inconsistent atrioventricular conduction.
- No dominant atrial pacemaker site, differentiating it from other supraventricular tachycardias.
2. Laboratory Tests and Imaging
- Arterial blood gas (ABG): Assesses hypoxia and hypercapnia in COPD patients.
- Electrolyte panel: Detects potassium and magnesium imbalances.
- Echocardiogram: Evaluates left atrial and ventricular function.
- Chest X-ray or CT scan: Identifies underlying pulmonary pathology.
Treatment Strategies for Multifocal Atrial Tachycardia
1. Addressing the Underlying Cause
Successful treatment of MAT requires managing the primary condition:
- Optimizing COPD therapy: Oxygen therapy, bronchodilators (with caution), and corticosteroids.
- Correcting electrolyte imbalances: IV potassium and magnesium supplementation.
- Managing infections and sepsis: Appropriate antibiotics and supportive care.
- Stopping offending drugs: Adjusting beta-agonists, theophylline, and catecholamine usage.
2. Pharmacological Management
- Calcium Channel Blockers (Verapamil, Diltiazem): Reduce atrial automaticity and control ventricular response.
- Beta-Blockers (Metoprolol, Esmolol): Used cautiously, particularly in patients without severe bronchospasm.
- Magnesium Sulfate: Shown to be beneficial even in normomagnesemic patients.
- Amiodarone (in select cases): Rarely used due to pulmonary toxicity concerns.
3. Non-Pharmacological Approaches
- Oxygen Therapy: Essential for hypoxic patients.
- Non-invasive ventilation (BiPAP or CPAP): Supports respiratory function in COPD exacerbations.
- Ablation therapy (rare cases): Considered in refractory symptomatic patients.
Prognosis and Complications
1. Prognosis
- Depends primarily on the underlying condition.
- MAT alone is not life-threatening but signifies significant systemic disease.
- Heart failure and severe pulmonary disease worsen long-term outcomes.
2. Potential Complications
- Progression to atrial fibrillation or flutter.
- Reduced cardiac output due to persistent tachycardia.
- Respiratory failure in COPD patients.
- Increased mortality if untreated.
Recent Research and Future Directions
Current studies focus on:
- New antiarrhythmic agents with lower pulmonary side effects.
- Improved risk stratification for patients prone to MAT progression.
- Advanced imaging for earlier detection of atrial conduction abnormalities.
Multifocal Atrial Tachycardia is a secondary arrhythmia strongly associated with pulmonary and systemic illnesses. Early identification and treatment of the underlying cause remain the cornerstone of management. Advances in electrophysiology, targeted drug therapy, and pulmonary care continue to improve patient outcomes. Proper diagnosis and comprehensive treatment significantly reduce complications and improve the quality of life for affected individuals.