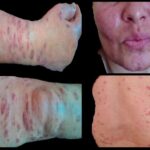
Multicentric Castleman’s Disease (MCD) is a rare and complex lymphoproliferative disorder characterized by an overgrowth of lymphoid tissue in multiple lymph node regions. Unlike the unicentric form, which affects a single lymph node, MCD impacts multiple sites and is often associated with systemic inflammatory symptoms. It is classified into two main subtypes:
- HHV-8-associated MCD: Caused by human herpesvirus-8 (HHV-8), commonly seen in individuals with immunosuppression, such as HIV-positive patients.
- Idiopathic MCD (iMCD): Occurs in individuals without HHV-8 infection, with an unknown underlying cause.
Symptoms of Multicentric Castleman’s Disease
MCD presents with a wide range of systemic symptoms due to excessive cytokine production, particularly interleukin-6 (IL-6). Common symptoms include:
- Fever and night sweats
- Unexplained weight loss
- Fatigue and weakness
- Generalized lymphadenopathy (swollen lymph nodes in multiple areas)
- Enlarged spleen (splenomegaly) and liver (hepatomegaly)
- Edema and fluid retention
- Anemia and low blood cell counts
Causes and Risk Factors
The exact cause of idiopathic MCD remains unknown, but research suggests immune dysregulation plays a crucial role. The known causes and risk factors include:
- HHV-8 infection: Activates the immune system, leading to abnormal B-cell proliferation.
- HIV/AIDS: Increases susceptibility to HHV-8-associated MCD.
- Autoimmune factors: Some patients with iMCD exhibit autoantibodies and immune system hyperactivity.
- Genetic predisposition: Although not well-defined, some genetic mutations may contribute to MCD development.
Diagnosis of Multicentric Castleman’s Disease
Diagnosing MCD requires a comprehensive clinical evaluation, including:
1. Laboratory Tests
- Elevated C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR)
- High levels of IL-6 and vascular endothelial growth factor (VEGF)
- Anemia and thrombocytopenia
2. Imaging Studies
- CT or MRI scans: Detect widespread lymphadenopathy, splenomegaly, and organ involvement.
- PET-CT scans: Identify hypermetabolic lymph nodes.
3. Lymph Node Biopsy
A biopsy is crucial for confirming MCD, showing characteristic hypervascularity, germinal center expansion, and plasma cell infiltration.
Treatment Options for Multicentric Castleman’s Disease
Treatment strategies depend on the subtype of MCD, disease severity, and presence of HHV-8 infection.
1. Targeted Therapy
- Siltuximab (Anti-IL-6 monoclonal antibody): FDA-approved for iMCD, effectively reduces IL-6-mediated inflammation.
- Tocilizumab (IL-6 receptor blocker): Alternative for patients intolerant to siltuximab.
2. Chemotherapy and Immunotherapy
- Rituximab (Anti-CD20 monoclonal antibody): First-line therapy for HHV-8-associated MCD.
- Etoposide-based chemotherapy: Used in severe cases with aggressive disease.
- Corticosteroids: Help control inflammation in combination with other therapies.
3. Antiviral Therapy (For HHV-8-Associated MCD)
- Ganciclovir and Valganciclovir: Target HHV-8 replication.
- HIV antiretroviral therapy (ART): Essential for HIV-positive patients.
4. Supportive Care
- Blood transfusions for anemia
- Plasma exchange in severe cytokine storm cases
- Nutritional support and pain management
Prognosis and Outlook
The prognosis of MCD varies based on subtype and response to treatment. Early diagnosis and targeted therapy have significantly improved survival rates.
- HHV-8-associated MCD: Managed effectively with rituximab-based therapy and antiviral treatment.
- Idiopathic MCD: Patients responding to siltuximab or tocilizumab often achieve long-term disease control.
- Severe cases with multiorgan involvement: Require aggressive treatment but may have a poorer prognosis.
Current Research and Advances
Recent studies are exploring:
- New IL-6 inhibitors and combination therapies
- Genetic factors influencing MCD susceptibility
- Better diagnostic biomarkers for early detection
- Immunomodulatory treatments for refractory cases
Multicentric Castleman’s Disease is a challenging disorder requiring a multidisciplinary approach. Advances in targeted therapies and immunomodulation have revolutionized management, offering better patient outcomes. Ongoing research continues to enhance our understanding of this complex disease, paving the way for improved treatment strategies.