Male hypogonadism is a medical condition characterized by the body’s inability to produce sufficient testosterone, the primary male sex hormone. This deficiency can result in developmental issues, sexual dysfunction, and various health complications. The condition may be congenital or acquired and is classified into primary hypogonadism and secondary hypogonadism based on its origin.
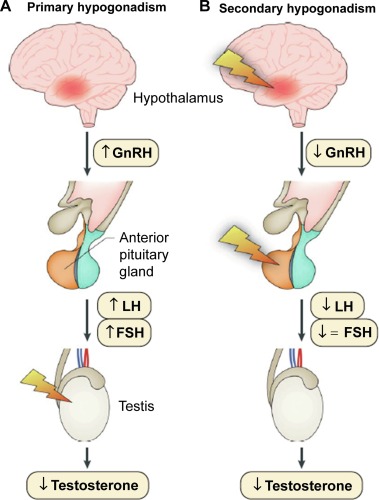
Types of Male Hypogonadism
Primary Hypogonadism
Primary hypogonadism, also known as primary testicular failure, occurs when the testes fail to produce adequate levels of testosterone despite normal stimulation from the brain. Causes include:
- Klinefelter syndrome – A genetic disorder with an extra X chromosome affecting testicular function.
- Undescended testes (cryptorchidism) – A condition where the testes fail to descend into the scrotum during fetal development.
- Mumps orchitis – Inflammation of the testicles due to a viral infection.
- Testicular injury or radiation exposure – Trauma or cancer treatments damaging testicular tissue.
Secondary Hypogonadism
Secondary hypogonadism is caused by problems in the hypothalamus or pituitary gland, which regulate testosterone production. Common causes include:
- Pituitary disorders – Tumors or pituitary gland dysfunction affecting hormone secretion.
- Kallmann syndrome – A genetic disorder impairing hormone-releasing neurons.
- Obesity and metabolic disorders – Excess weight affecting hormone balance.
- Chronic illnesses – Conditions like diabetes and HIV affecting hormonal regulation.
Symptoms of Male Hypogonadism
Symptoms vary depending on the onset of testosterone deficiency:
In Adolescents
- Delayed puberty
- Lack of deepened voice
- Reduced muscle mass and body hair
- Undeveloped genitals
In Adults
- Decreased libido and erectile dysfunction
- Fatigue and reduced muscle strength
- Depression and cognitive issues
- Increased body fat and gynecomastia
- Infertility due to low sperm production
Diagnosis of Male Hypogonadism
Diagnosis involves a thorough medical evaluation, including:
- Physical Examination – Assessment of body hair, muscle mass, and genital development.
- Blood Tests – Measurement of testosterone levels, luteinizing hormone (LH), and follicle-stimulating hormone (FSH).
- Imaging Studies – MRI or CT scans to evaluate pituitary abnormalities.
- Genetic Testing – To identify chromosomal disorders like Klinefelter syndrome.
Treatment Options for Male Hypogonadism
Testosterone Replacement Therapy (TRT)
TRT is the most common treatment, administered via:
- Injections – Long-acting testosterone esters injected into muscles.
- Gels and Patches – Applied to the skin for absorption.
- Implants and Pills – Sustained-release options for continuous hormone levels.
Lifestyle Modifications
- Weight Management – Reducing obesity to improve hormone balance.
- Exercise and Strength Training – Boosting testosterone levels naturally.
- Adequate Sleep and Stress Reduction – Optimizing hormonal function.
Medications for Secondary Hypogonadism
- Clomiphene citrate – Stimulates natural testosterone production.
- Human Chorionic Gonadotropin (hCG) – Promotes testicular function in fertility treatment.
Complications of Untreated Hypogonadism
If left untreated, male hypogonadism can lead to:
- Osteoporosis – Reduced bone density and increased fracture risk.
- Cardiovascular Issues – Higher risk of heart disease due to lipid imbalance.
- Psychological Disorders – Increased likelihood of depression and anxiety.
Male hypogonadism is a manageable condition with proper diagnosis and treatment. Early intervention with hormone replacement therapy, lifestyle changes, and medications can significantly improve quality of life. If you experience symptoms of low testosterone, consult an endocrinologist for proper assessment and personalized treatment options.

