Major Depressive Disorder (MDD) is a debilitating mental health condition that often requires a combination of treatments to achieve remission. While antidepressants and psychotherapy are the first-line treatments, many individuals require adjunct therapies to enhance their recovery. This article explores various adjunct treatment options, including pharmacological, psychotherapeutic, and lifestyle-based interventions.
Pharmacological Adjunct Treatments
1. Atypical Antipsychotics
Atypical antipsychotics are commonly used as adjuncts for individuals with treatment-resistant depression (TRD). These medications help regulate dopamine and serotonin levels to enhance the effects of antidepressants.
- Commonly Used Drugs: Aripiprazole, Quetiapine, Brexpiprazole
- Effectiveness: Studies show improved response rates when combined with SSRIs or SNRIs.
- Side Effects: Weight gain, metabolic changes, sedation.
2. Mood Stabilizers
Mood stabilizers like lithium and lamotrigine are effective in preventing relapse in MDD patients, particularly those with recurrent depressive episodes.
- Lithium: Reduces suicidal ideation and enhances antidepressant response.
- Lamotrigine: Helps in mood stabilization and preventing depressive recurrence.
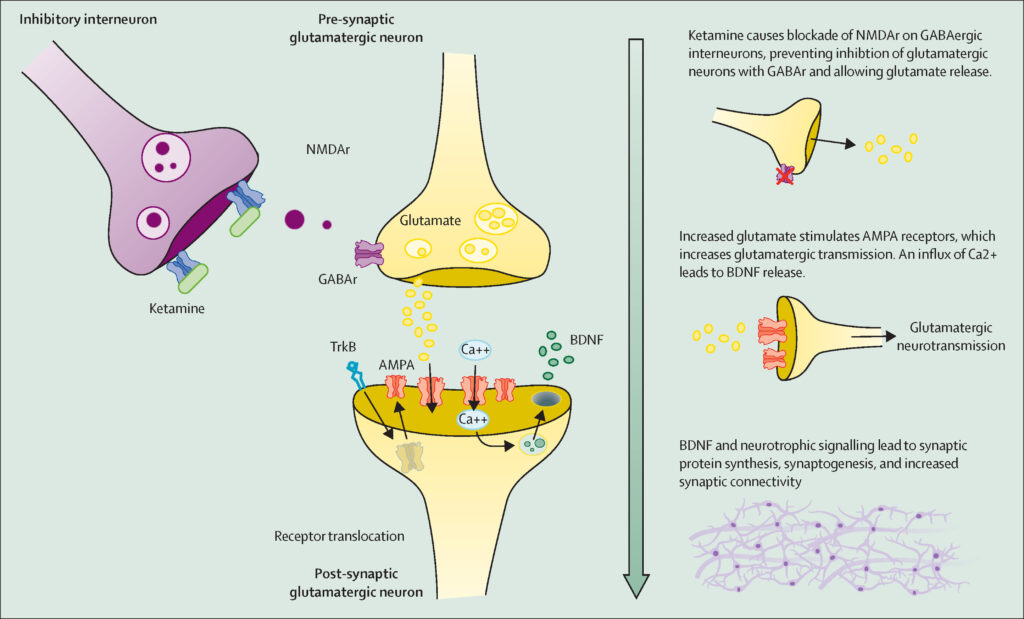
3. N-Methyl-D-Aspartate (NMDA) Receptor Modulators
Ketamine and esketamine are gaining recognition for their rapid-acting antidepressant effects.
- Ketamine: Administered via IV infusion, producing fast relief in severe depression.
- Esketamine (Spravato): FDA-approved nasal spray for treatment-resistant depression.
4. Thyroid Hormone Supplementation
Hypothyroidism can contribute to depressive symptoms. Supplementing with triiodothyronine (T3) has shown positive outcomes in some patients.
Psychotherapeutic Adjuncts
1. Cognitive Behavioral Therapy (CBT)
CBT is a widely recognized therapy for depression that helps individuals reframe negative thought patterns and develop coping strategies.
2. Mindfulness-Based Cognitive Therapy (MBCT)
MBCT combines traditional cognitive therapy with mindfulness practices to reduce depressive relapse rates.
3. Interpersonal Therapy (IPT)
IPT focuses on improving interpersonal relationships and addressing social factors contributing to depression.
Lifestyle and Alternative Treatments
1. Exercise and Physical Activity
Regular physical activity has been shown to enhance mood by increasing endorphin and serotonin levels.
- Recommended Activities: Aerobic exercise, yoga, resistance training.
2. Diet and Nutrition
A balanced diet rich in omega-3 fatty acids, antioxidants, and B vitamins supports brain health and improves depressive symptoms.
- Key Nutrients: Omega-3s, Vitamin D, Folate, Zinc.
3. Light Therapy
Light therapy is particularly effective for individuals with Seasonal Affective Disorder (SAD) but also benefits those with non-seasonal depression.
- Recommended Dosage: 10,000 lux exposure for 30 minutes daily.
4. Transcranial Magnetic Stimulation (TMS)
TMS is a non-invasive neuromodulation technique used for treatment-resistant depression.
- Mechanism: Uses magnetic fields to stimulate nerve cells in the brain.
- Efficacy: Proven to reduce depressive symptoms with minimal side effects.
Emerging Treatments
1. Psychedelic-Assisted Therapy
Research suggests that psilocybin and MDMA-assisted therapy may offer rapid and sustained relief for severe depression.
- Current Status: Under clinical trials, promising results.
2. Vagus Nerve Stimulation (VNS)
An implanted device stimulates the vagus nerve to regulate mood.
3. Deep Brain Stimulation (DBS)
Used in severe cases, DBS involves implanting electrodes in specific brain regions.
For individuals with major depressive disorder, adjunct treatments can significantly enhance the effectiveness of primary therapies. A personalized approach combining pharmacological, psychotherapeutic, and lifestyle interventions can improve treatment outcomes and quality of life.