Low cardiac output (LCO) refers to a condition in which the heart fails to pump sufficient blood to meet the body’s metabolic demands. This can lead to organ dysfunction, circulatory failure, and even life-threatening complications. Understanding its causes, symptoms, and management strategies is crucial for early diagnosis and intervention.
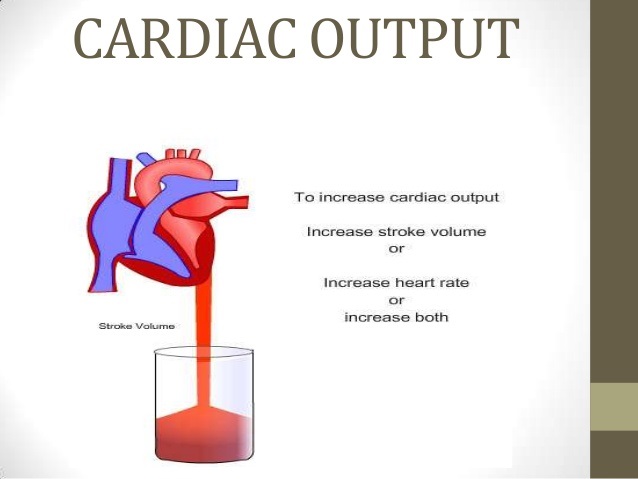
Understanding Cardiac Output
Cardiac output (CO) is the volume of blood pumped by the heart per minute, calculated as:
A normal cardiac output ranges between 4-8 L/min. When this falls below the required levels, tissues and organs receive inadequate oxygen, leading to clinical symptoms.
Causes of Low Cardiac Output
Several conditions can lead to low cardiac output, including:
1. Heart Failure
- Systolic dysfunction (reduced ejection fraction)
- Diastolic dysfunction (impaired ventricular filling)
2. Myocardial Infarction (Heart Attack)
- Damage to the heart muscle reduces its ability to pump effectively.
3. Cardiomyopathy
- Conditions like dilated or hypertrophic cardiomyopathy impair heart function.
4. Hypovolemia
- Severe dehydration or hemorrhage reduces blood volume and cardiac output.
5. Cardiac Arrhythmias
- Irregular heart rhythms, such as atrial fibrillation, can impair stroke volume.
6. Pulmonary Embolism
- A blockage in the pulmonary artery increases right ventricular afterload and reduces left ventricular output.
7. Valvular Heart Disease
- Stenosis or regurgitation of heart valves disrupts normal blood flow.
8. Sepsis and Septic Shock
- Systemic inflammation can cause vasodilation and myocardial depression, leading to low cardiac output.
Symptoms of Low Cardiac Output
The symptoms vary based on the underlying cause and severity. Common symptoms include:
- Fatigue and weakness
- Shortness of breath (dyspnea)
- Cold extremities due to poor perfusion
- Dizziness or fainting (syncope)
- Low blood pressure (hypotension)
- Swelling in legs and feet (peripheral edema)
- Reduced urine output (oliguria)
Diagnosis of Low Cardiac Output
Diagnosis involves a combination of clinical examination, imaging, and hemodynamic assessment:
1. Physical Examination
- Assessment of blood pressure, heart sounds, and signs of organ hypoperfusion.
2. Electrocardiogram (ECG)
- Identifies arrhythmias or ischemic changes.
3. Echocardiography
- Evaluates heart function, ejection fraction, and valvular abnormalities.
4. Hemodynamic Monitoring
- Measures central venous pressure, pulmonary artery pressure, and cardiac index.
5. Laboratory Tests
- Includes cardiac biomarkers (troponin), BNP levels, and blood gases.
Treatment of Low Cardiac Output
Treatment aims to restore adequate cardiac function and improve tissue perfusion.
1. Medications
- Inotropes (e.g., Dobutamine, Milrinone): Enhance myocardial contractility.
- Vasopressors (e.g., Norepinephrine): Improve blood pressure and perfusion.
- Diuretics (e.g., Furosemide): Reduce fluid overload in heart failure.
- Beta-blockers (e.g., Metoprolol): Manage heart rate and reduce myocardial oxygen demand.
2. Mechanical Support
- Intra-aortic Balloon Pump (IABP): Improves coronary perfusion.
- Left Ventricular Assist Device (LVAD): Provides circulatory support in severe cases.
3. Surgical Interventions
- Coronary Artery Bypass Grafting (CABG): Restores blood flow in ischemic heart disease.
- Heart Valve Repair or Replacement: Addresses valvular disorders.
- Heart Transplant: Considered for end-stage heart failure.
4. Lifestyle Modifications
- Dietary Changes: Low sodium, heart-healthy diet.
- Exercise Therapy: Supervised cardiac rehabilitation.
- Smoking and Alcohol Cessation: Improves cardiovascular health.
Prognosis and Prevention
The prognosis depends on the underlying condition and the timeliness of intervention. Prevention strategies include:
- Regular cardiovascular check-ups
- Managing risk factors like hypertension and diabetes
- Maintaining an active lifestyle
- Following prescribed treatments diligently
Low cardiac output is a critical condition that requires timely diagnosis and management. Understanding its causes, symptoms, and treatment options can improve patient outcomes and quality of life. Early intervention and preventive measures play a pivotal role in reducing the burden of this condition.